Estudios originales
← vista completaPublicado el 11 de agosto de 2016 | http://doi.org/10.5867/medwave.2016.07.6514
Accidentes biológicos en estudiantes del último año de medicina de tres hospitales de Lima, Perú
Biological accidents in last-year medical students from three hospitals in Lima Peru
Resumen
OBJETIVO Determinar la frecuencia y características de los accidentes biológicos en estudiantes del último año de medicina de tres hospitales de Lima.
MÉTODOS Estudio transversal, realizado en tres hospitales del Seguro Social de Salud de Lima, en diciembre de 2014. La población de estudio la constituyen los internos de medicina. Los accidentes biológicos se registraron aplicando un cuestionario sobre exposición a sangre y fluidos corporales, elaborado sobre la base de los formatos utilizados por el sistema Exposure Prevention Information Network y Centers for Disease Control and Prevention. Se interrogó sobre la ocurrencia y número de accidentes biológicos presentados, además de las características del último accidente. Los datos categóricos se presentan como frecuencias absolutas y porcentuales, en tanto los datos numéricos se muestran como mediana y rango intercuartílico.
RESULTADOS En total fueron 100 encuestados. El 85% de ellos presentó algún accidente biológico durante el año, con una mediana de 2 y un rango intercuartílico de 3. El tipo de exposición más frecuente fue el percutáneo (71,8%), siendo el dispositivo más común la guja hueca (54,1%). El lugar y las actividades más frecuentes al momento de la exposición fueron la sala de partos (44,7%), atención de parto (24,7%) y sutura (24,7%). Tres accidentes ocurrieron con pacientes de alto riesgo, pero sólo uno recibió profilaxis antiviral. El 49,4% consideró como causa el cansancio o fatiga. El 75,3% de los accidentes no se reportaron. Los guantes son la medida de protección más utilizada (95%).
CONCLUSIÓN La frecuencia de accidentes biológicos presentados es alta. El escaso reporte y uso inadecuado de barreras de protección, son eventos que elevan el riesgo de los estudiantes de medicina.
Introducción
La práctica médica involucra riesgos biológicos por la alta frecuencia de manipulación de elementos punzocortantes así como de fluidos biológicos, siendo fuentes potenciales de enfermedades serias entre trabajadores de salud y estudiantes de medicina [1],[2],[3].
El internado de medicina es el séptimo y último año en el plan de estudios de la carrera universitaria en Perú. En él, el estudiante realiza prácticas hospitalarias teniendo un contacto más estrecho con el paciente, al realizar diferentes procedimientos clínico quirúrgicos. Algunos de estos son punción lumbar, extracción de sangre arterial (análisis de gases arteriales) y venosa, paracentesis y atención de partos. El objetivo de dichas actividades es dar un apropiado adiestramiento para que los alumnos puedan adquirir las habilidades motrices necesarias para el buen ejercicio profesional [1].
Los estudiantes de medicina, por el hecho de estar en formación, añadiéndose su inexperiencia y falta de desarrollo de habilidades inherentes a su periodo de adiestramiento [1],[4],[5]; se encuentran en mayor riesgo de sufrir accidentes biológicos con exposición a patógenos sanguíneos como los virus de inmunodeficiencia humana, de hepatitis B y de hepatitis C. De igual manera, el uso de medidas de bioseguridad y el adecuado reporte de los accidentes, son aplicados irregularmente por los estudiantes de medicina [5],[6],[7].
En Perú hay escasos estudios sobre los accidentes biológicos en los estudiantes de medicina del último año [4]. Este grupo es el de mayor riesgo al realizar el internado, debido a su contacto más estrecho y real con los pacientes. Los datos estadísticos en Perú y otros países sobre los accidentes biológicos en estudiantes de medicina son el reflejo del enorme subregistro y de la poca sensibilidad que poseen los estudiantes en el reconocimiento y manejo de estos accidentes [1],[2],[3],[4],[5]. Por tales razones, es que nos planteamos realizar el presente estudio en nuestro medio, cuyo objetivo es determinar la frecuencia y características de los accidentes biológicos en estudiantes del último año de medicina de tres hospitales de Lima.
Métodos
El presente es un estudio transversal. Se realizó en diciembre de 2014, en tres hospitales del Seguro Social de Salud de Lima: Hospital Nacional Edgardo Rebagliati Martins, Hospital Nacional Guillermo Almenara Irigoyen y Hospital de Emergencias Grau.
En Perú los establecimientos de salud se categorizan según niveles de atención. En el primer nivel de atención se atienden problemas de salud de baja complejidad, con menor especialización y tecnificación de sus recursos, en ellos se desarrollan principalmente actividades de promoción y protección. En el segundo nivel se atienden necesidades de salud que requieren atención de complejidad intermedia. Y en el tercer nivel se requiere de una atención de salud de alta complejidad, de alta especialización y tecnificación. La categorización del establecimiento de salud, está determinada por la capacidad resolutiva cualitativa (capacidad para producir el tipo de servicios necesarios para solucionar la severidad de las necesidades de la población), y el nivel tecnológico de los recursos (grado de especialización y tecnificación) [8].
El Hospital Rebagliati y el Hospital Almenara están categorizados como Institutos de Salud Especializados de tercer nivel de atención, categoría III-2, siendo el máximo nivel otorgado por el Ministerio de Salud en Perú [9],[10]. El Hospital Emergencias Grau es también de tercer nivel, pero de categoría III-1, puesto que no tiene subespecialidades [11]. Estas instituciones se escogieron por conveniencia, anticipando que se ubican en lugares céntricos y son hospitales docentes que tienen convenios con todas las universidades, lo que permite la rotación en sus instalaciones de estudiantes de medicina y médicos residentes.
La población estuvo conformada por los estudiantes del último año de medicina de los tres hospitales mencionados. Se incluyeron a los estudiantes del proceso internado médico del Seguro Social de Salud 2014, de ambos sexos y con rotaciones en los servicios de medicina interna, gineco-obstetricia, pediatría y cirugía. Se excluyeron a los estudiantes rotantes pertenecientes a otros hospitales y los que estaban con licencia. No se realizaron procedimientos específicos para muestreo.
Los participantes del estudio fueron ubicados durante sus rotaciones clínicas, con el permiso del jefe de servicio correspondiente para que pudieran llenar el instrumento en el tiempo necesario. Del mismo modo, se explicó a los participantes que el llenado de los datos era voluntario y confidencial, que serían utilizados con fines académicos y que podrían retirarse en cualquier momento del proceso. El instrumento no consignó secciones que permitieran la identificación del participante.
La recolección y registro de accidentes biológicos se realizó mediante la aplicación de un cuestionario sobre exposición a sangre y fluidos corporales. La encuesta se elaboró sobre la base de dos formatos. El primero se sustentó en el sistema Exposure Prevention Information Network (EPINet), para el registro de accidentes con agujas u objetos punzocortantes [12]. El segundo se basó en el formato de los Centers for Disease Control and Prevention (CDC) de exposición a sangre y fluidos corporales [13]. Se construyó un cuestionario seleccionando 19 preguntas que fueron traducidas al español. Se obviaron preguntas sobre situación laboral o contractual y preguntas abiertas, debido a que no correspondían con las características de la población.
Se interrogó acerca de la ocurrencia de accidentes biológicos, definidos como todo proceso repentino con probabilidad de adquirir una infección transmisible debido a la exposición con fluidos biológicos [14] como sangre, tejido u otro fluido corporal potencialmente infeccioso a través de una herida percutánea (aguja o corte con objeto afilado), contacto de membrana mucosa o piel no intacta [15]. Si la respuesta era afirmativa, se indagó sobre la frecuencia de accidentes presentados desde el inicio del internado hasta el momento de la encuesta, las características del último accidente presentado, medios de protección que utiliza y número de dosis contra la hepatitis B. Si la respuesta era negativa, pasaba a responder sólo las dos últimas preguntas sobre medidas de protección y dosis contra hepatitis B.
Los datos categóricos se presentados como frecuencias absolutas y porcentuales. Los datos numéricos se muestran como mediana y rango intercuartílico. Se utilizó para la base de datos Microsoft Excel 2013 y para el análisis estadístico el programa SPSS versión 20.
Resultados
La población fue de 105 estudiantes, de los cuales se excluyeron a tres que estaban con licencia y hubo una tasa de pérdida de dos, encuestándose en total a 100 estudiantes.
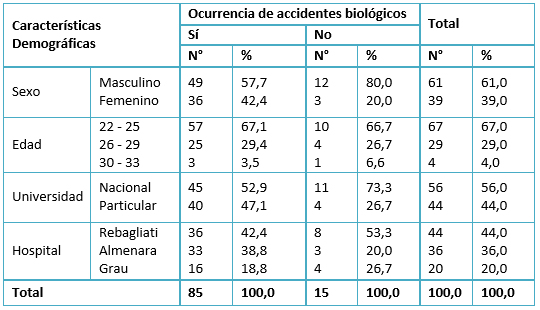
La ocurrencia de accidentes biológicos según características demográficas se presenta en la Tabla 1. Se encontró predominio del sexo masculino (61%). El 85% de los estudiantes presentó algún accidente biológico durante su año de internado.
 Tamaño completo
Tamaño completo Durante el año de internado de los estudiantes encuestados se presentaron en total 297 accidentes biológicos, entre mucocutáneos 44,8% (133) y percutáneos 55,2% (164). El número de accidentes biológicos durante el año de internado tuvo como mediana 2 y rango intercuartílico 3.
En cuanto a la descripción de las características en el último accidente presentado, encontramos que el tipo de exposición más frecuente también fue el percutáneo con 71,8% (61). El líquido biológico más frecuentemente involucrado fue sangre con 72,9% (62), seguido por líquido amniótico/vaginal visiblemente ensangrentado en 18,8% (16).
 Tamaño completo
Tamaño completo 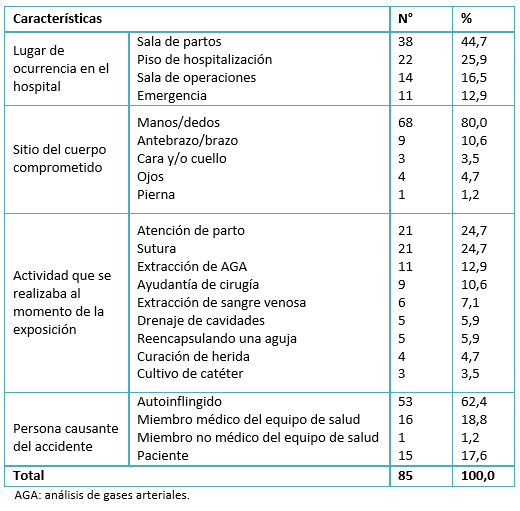 Tamaño completo
Tamaño completo El 98,8% (84) de los pacientes fuente eran identificables. Un 18,8% (16) de los estudiantes desconocían si el paciente identificable era de alto riesgo. Tres de los accidentes presentados ocurrieron con pacientes de alto riesgo, sin embargo sólo uno de los estudiantes accidentados recibió profilaxis antiviral
 Tamaño completo
Tamaño completo El 75,3% (64) de los estudiantes que sufrieron exposición en el último accidente no lo reportaron. El motivo que señalaron como más frecuente fue que el paciente era sin riesgo 73,4% (47), seguido por la falta de tiempo 54,7% (35).
Al interrogárseles sobre las barreras de protección que realmente utilizan para minimizar el riesgo de ocurrencia de accidentes biológicos, respondieron que lo que más utilizan son los guantes (95%), seguido por el mandil (67%) y mascarilla (50%). Los menos utilizados son los lentes de protección (14%) y el gorro (22%).
El 87% de los estudiantes encuestados refirieron tener las tres dosis de vacuna contra la hepatitis B y el 13% tenían sólo dos dosis.
Discusión
El 85% de los estudiantes del último año de medicina presentó algún accidente biológico (Tabla 1). Ramos y colaboradores también encontraron una alta frecuencia, el 96% de los estudiantes encuestados sufrieron por lo menos un accidente durante su año de internado en Lima en el año 2000 [4]. No obstante, otros estudios indican que la frecuencia puede ser menor como el de Flores y colaboradores, donde el 73% de los estudiantes del último año sufrieron accidentes punzocortantes [16]. Inga y colaboradores en su estudio en alumnos de medicina de una universidad pública en Lima, revelaron que el 32% de los que sufrieron algún accidente biológico correspondía a los estudiantes del último año, teniendo 75 veces más probabilidad de sufrir un accidente que los de primer año [1]. La mayor frecuencia de accidentes biológicos en los estudiantes del último año de medicina, se puede explicar debido a las actividades y procedimientos que realizan en forma progresiva, según niveles académicos, y a la gran demanda de pacientes que acuden para atención a los hospitales de estudio.
El tipo de exposición más frecuente del último accidente biológico presentado fue el percutáneo (72%). Según las recomendaciones de Centers for Disease Control and Prevention y el New York State Department of Health, clasifican como riesgo alto de adquirir una infección aquel donde existe cortadura o pinchazo [17]. Este resultado es inferior a lo observado por Ramos y colaboradores, donde el 87% de los accidentes fueron de alto riesgo [4].
El líquido biológico involucrado más frecuentemente en el último accidente fue sangre, encontrándose dentro del rango que señalan diversos estudios [1],[2]. El líquido amniótico/vaginal visiblemente ensangrentado fue el segundo (16%). Herrera y colaboradores reportan al líquido amniótico en un porcentaje menor (5,8%), sin especificar si está ensangrentado o no [2]. Este mayor porcentaje puede explicarse por lo encontrado como el lugar más frecuente de ocurrencia del accidente, que fue la sala de partos.
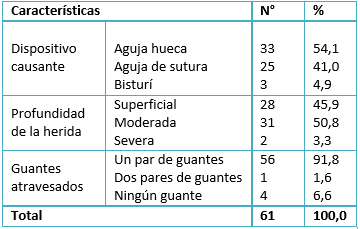
Dentro de las características de la exposición percutánea en el último accidente presentado (Tabla 2), encontramos que el dispositivo causante de la lesión más frecuente fue la aguja hueca, similar a lo observado por otros estudios [1],[7],[18], la cual representa un mayor riesgo de contacto para enfermedades infecciosas.
En el 92% de los accidentes percutáneos el dispositivo causante de la lesión atravesó un par de guantes, indicando que la mayoría de los estudiantes utilizaba dicha barrera de protección. Esto debido a que en los hospitales de estudio, por su mayor capacidad financiera a diferencia de los hospitales públicos, los guantes son la barrera de protección más proporcionada y encontrada fácilmente en cualquier ambiente de trabajo. La bibliografía refiere que el uso de dos pares de guantes ha demostrado reducir significativamente las perforaciones en los guantes internos y aún más el riesgo de contaminación [19]. Por ello, es una práctica que se aconseja de manera rutinaria [5]. Sin embargo, encontramos que sólo un estudiante utilizó doble guante. En consecuencia, se observa en nuestro medio que esta práctica no es difundida. Esto se debe a que las condiciones de trabajo en el sector salud de Perú no son adecuadas, habiendo falta de recursos económicos en el nosocomio que no permite abastecer a todo el personal con los equipos de protección mínimos necesarios.
El lugar de ocurrencia más frecuente fue la sala de partos, seguido por el piso de hospitalización y la sala de operaciones (Tabla 3). La bibliografía médica informa que el riesgo de exposición es mayor en áreas donde se realiza mayor cantidad de procedimientos invasivos y de mayor contacto con pacientes. Además, las prácticas de mayor riesgo son las de especialidades quirúrgicas y de gineco obstetricia [1],[5],[20].
En el presente estudio la atención de parto y la sutura fueron los procedimientos más frecuentemente realizados. Esto es similar a lo encontrado por Tapias y colaboradores, en donde el procedimiento más frecuente fue atención del parto, seguido de ayudantía quirúrgica [5]. Ello se puede explicar porque los estudiantes del último año de medicina en nuestro país tienen la posibilidad de realizar una gran variedad de procedimientos invasivos bajo supervisión, como la atención de partos y apoyo en cirugías de diversa complejidad, como lo señalaron también Tapias y colaboradores [5]. Además la mayoría atiende su primer parto en el internado, tratando en lo posible de atender en su integridad la mayor cantidad de partos, realizando también sus primeras episiorrafias.
La cuarta parte de los accidentes sucedieron en el piso de hospitalización. Esto se correlaciona con la extracción de análisis de gases arteriales, siendo la tercera actividad frecuentemente realizada al momento del accidente. Allí se produce una exposición de alto riesgo, al encontrarse el dispositivo con aguja hipodérmica directamente en contacto con la arteria del paciente fuente [14].
Cerca de las dos terceras partes de los internos considera que el accidente fue autoinflingido, lo cual concuerda con lo encontrado en otros estudios [1],[5],[7],[20].
Tres accidentes ocurrieron con pacientes de alto riesgo, definidos como pacientes con historia o factores de riesgo de infección por virus de inmunodeficiencia humana, virus de la hepatitis B y/o virus de la hepatitis C [14]. Pero sólo uno de los estudiantes accidentados recibió profilaxis antiviral. Tapias y colaboradores informaron que cinco de los accidentes presentados en los estudiantes fueron con pacientes de alto riesgo, recibiendo sólo dos de ellos profilaxis [5]. Esto puede ser explicado quizás por la poca cultura del reporte, la desinformación y lo mal planteado que se encuentra el sistema de manejo de riesgos, pues no existen o son muy escasos los protocolos a seguir tras un accidente biológico en las áreas de trabajo.
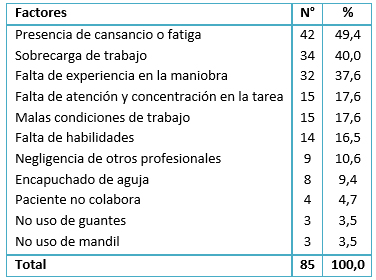
La presencia de cansancio o fatiga es el factor más importante como causante del accidente. Esto difiere de lo reportado por Tapias y colaboradores, quienes encontraron que 39% de los estudiantes respondieron que se debió a la falta de destreza, malas condiciones del lugar de trabajo en 23% y fatiga en 18% [5]. Esto podría deberse a que los estudiantes del último año de medicina en nuestro medio, más que actividades pre profesionales, desarrollan tareas que van más allá de lo rigurosamente académico, como también lo señalaron Galán y colaboradores [20]. Entre estas tareas se cuentan guardias seguidas, escasez de áreas de descanso y falta de descanso postguardia. La bibliografía indica que las largas horas de trabajo y la falta de sueño entre los médicos en formación resultan en fatiga, que se asocia con un aumento de tres veces en el riesgo de lesiones por pinchazo de aguja [21]. Además los lugares del hospital en donde más se presentaron los accidentes, son ambientes donde principalmente se realizan los turnos de guardia.
El reporte del accidente presentado es muy importante, puesto que permite a la persona recibir consejería sobre los riesgos de la exposición y la prevención secundaria de la infección [5]. No se debe confiar sólo en los datos que contiene la historia clínica del paciente fuente acerca del riesgo de infección para los virus de inmunodeficiencia humana, de la hepatitis B y/o virus de hepatitis C. Por consiguiente, todos los accidentes deberían reportarse para realizarse las pruebas pertinentes. A pesar de ello, encontramos que las tres cuartas partes de los accidentes no se reportaron, argumentándose que se trataba de un paciente sin riesgo. Similar a lo encontrado por Tapias y colaboradores, en que más de la mitad de los estudiantes no reportaron el accidente, dando como razón que la exposición era sin riesgo [5].
Un aspecto substancial es la inmunización activa, la cual constituye la medida más eficaz para la prevención de la infección ocupacional de la hepatitis B, estando recomendada en los estudiantes de medicina antes de iniciar las prácticas propias de su carrera [1]. En nuestro estudio el 87% de los estudiantes encuestados informaron haber recibido las tres dosis recomendadas, muy superior a lo encontrado por otros estudios [1],[4],[7]. Esta mayor cobertura se debería a que, en su mayoría, dichas vacunas son gratuitas y prerrequisitos para las matrículas en la universidad. Sin embargo, hay un 13% que no están completamente protegidos. Esto es preocupante por el estrecho contacto que tienen con los pacientes, la elevada frecuencia de accidentes de alto riesgo presentados y porque en Perú existen áreas con alta endemicidad del virus.
Debe mencionarse que este trabajo presenta limitaciones, como la heterogeneidad de la población estudiada y la pertenencia a hospitales privados (Seguro Social de Salud). Se sugiere realizar más estudios en los que se pueda comparar la frecuencia y características de los accidentes biológicos de los internos de medicina que pertenecen a universidades públicas y privadas. Del mismo modo, el presente estudio no es representativo de lo que ocurre en todo el país, debido a que no se ha tenido dicha consideración en su diseño. Por este motivo sería recomendable la realización de un estudio a nivel nacional, para evaluar las diferencias que se presentan en provincias.
Conclusiones
La frecuencia de accidentes biológicos presentados es alta. El escaso reporte y uso inadecuado de barreras de protección son eventos que elevan el riesgo de los estudiantes de medicina.
Los hospitales y las universidades deben fomentar y reforzar constantemente desde los primeros años de estudio, la importancia de la aplicación de las medidas de precaución universal, la inmunización en pregrado contra la hepatitis B, la cultura del reporte y los protocolos post exposición.
Notas
Aspectos éticos
En cuanto a la aprobación del comité de ética tenemos el inconveniente de que en los hospitales sedes en los cuales se realizó el estudio en diciembre del 2014, no contaban con un comité de ética consolidado; sin embargo se procedió a solicitar la autorización a los jefes de servicio de los departamentos de Medicina Interna, Cirugía, Gineco-obstetricia y Pediatría de los tres hospitales para la aplicación del cuestionario. A los estudiantes se les ubicó en los servicios donde realizaban su última rotación, ellos fueron invitados a participar en el estudio indicándoseles que el cuestionario era anónimo, voluntario y se solicitó su consentimiento informado verbal. El presente estudio no implicó ningún riesgo para los participantes, la información recogida no tuvo ninguna incidencia en la evaluación del internado médico, tampoco se realizaron preguntas de tipo personal.
Declaración de conflictos de intereses
Los autores han completado el formulario de declaración de conflictos intereses del ICMJE traducido al castellano por Medwave, y declaran no haber recibido financiamiento para la realización del reporte; no tener relaciones financieras con organizaciones que podrían tener intereses en el artículo publicado, en los últimos tres años; y no tener otras relaciones o actividades que podrían influir sobre el artículo publicado. Los formularios pueden ser solicitados contactando al autor responsable o a la dirección editorial de la Revista.
Financiamiento
El presente estudio fue autofinanciado, así mismo no existe otros conflictos de interés.

