Resúmenes Epistemonikos
← vista completa
Publicado el 15 de marzo de 2016 | http://doi.org/10.5867/medwave.2016.6383
¿Tratamiento conservador o quirúrgico para fracturas toracolumbares tipo burst sin déficit neurológico?
Conservative versus operative treatment for thoracolumbar burst fractures without neurologic deficit
Carolina Avilés , Sebastián Flores, Marcelo Molina
Resumen
Las fracturas toracolumbares tipo burst representan hasta el 17% de las fracturas de columna.Se ha planteado tanto el tratamiento conservador como el quirúrgico para este tipo de fracturas, observando buenos resultados funcionales con ambos, pero con un mayor costo y riesgo de producir efectos adversos con la cirugía. Utilizando la base de datos Epistemonikos, la cual es mantenida mediante búsquedas en 30 bases de datos, identificamos seis revisiones sistemáticas que en conjunto incluyen cuatro estudios aleatorizados. Realizamos un metanálisis y tablas de resumen de los resultados utilizando el método GRADE. Concluimos que el tratamiento quirúrgico podría disminuir el riesgo de deterioro neurológico pero con un mayor riesgo de complicaciones generales. Concluimos que no está claro si existen diferencias en dolor, funcionalidad, calidad de vida, necesidad de reintervención o progresión radiográfica de la cifosis entre el tratamiento conservador y el quirúrgico
Problema
Las fracturas toracolumbares tipo burst representan hasta el 17% de las fracturas de columna [1]. Las fracturas tipo burst se producen por cargas en compresión axial, resultando en falla de las columnas anterior y media de la comuna vertebral. Se estima que la incidencia de déficit neurológico producto de fracturas toracolumbares tipo burst es entre un 50 y 60 % [1],[2]. Si bien muchas lesiones de la médula espinal a este nivel no producen parálisis de las extremidades inferiores, pueden dejar un segmento espinal inestable debido a la disrupción de elementos óseos y ligamentosos, que podrían causar lesión neurológica tardía [1]. Existen opiniones divididas respecto al tratamiento ideal de las fracturas toracolumbares tipo burst sin déficit neurológico. Tanto el tratamiento conservador como el quirúrgico son ampliamente utilizados en la práctica clínica. Estudios previos han mostrado que el tratamiento conservador con movilización temprana logra buenos resultados funcionales, incluso en fracturas con compromiso de la columna posterior. El tratamiento quirúrgico también ha mostrado resultados radiográficos favorables con resultados funcionales similares al tratamiento ortopédico, pero a un mayor costo y con el riesgo de exponer a los pacientes a efectos adversos y complicaciones propias de una cirugía.
Métodos
Utilizamos la base de datos Epistemonikos, la cual es mantenida mediante búsquedas en 30 bases de datos, para identificar revisiones sistemáticas y sus estudios primarios incluidos. Con esta información generamos un resumen estructurado, siguiendo un formato preestablecido, que incluye mensajes clave, un resumen del conjunto de evidencia (presentado como matriz de evidencia en Epistemonikos), metanálisis del total de los estudios, tablas de resumen de resultados con el método GRADE, y tabla de otras consideraciones para la toma de decisión.
|
Mensajes clave
- El tratamiento quirúrgico de las fracturas toracolumbares tipo burst podría disminuir el riesgo de deterioro neurológico, pero a su vez, podría aumentar el riesgo de complicaciones generales.
- No está claro si existen diferencias en dolor, funcionalidad, calidad de vida, necesidad de reintervención o progresión radiográfica de la cifosis porque la certeza de la evidencia es muy baja.
|
Acerca del conjunto de evidencia para esta pregunta
|
Cuál es la evidencia.
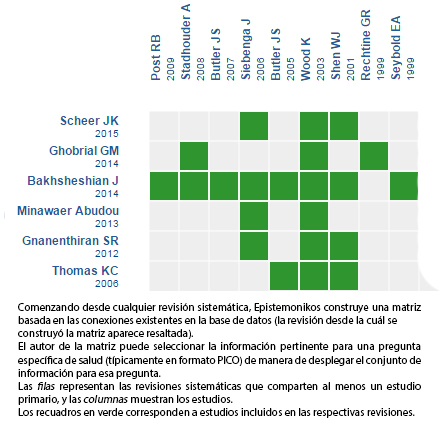
Véase matriz de evidencia en Epistemonikos más abajo.
|
Encontramos seis revisiones sistemáticas [3],[4],[5],[6],[7],[8], que incluyen cuatro estudios controlados aleatorizados [9],[10],[11],[12]. |
|
Qué tipo de pacientes incluyeron los estudios
|
Todos los estudios incluyeron pacientes adultos (edad de 18 a 65 años) con fractura toracolumbar tipo burst no patológica sin déficit neurológico [9],[10],[11],[12]. Un estudio incluyó a pacientes con TAC concordante con fractura con retropulsión del cuerpo vertebral en el canal raquídeo [11]. Un estudio incluyó a pacientes con TAC con fracturas tipo burst con pedículos y facetas articulares intactas [10]. Un estudio incluyó a pacientes con TAC compatible con canal espinal residual > 50% de lo normal [9] y un estudio no discriminó por tipo de compromiso del canal [12].
|
|
Qué tipo de intervenciones incluyeron los estudios
|
Todos los estudios compararon manejo conservador y quirúrgico [9],[10],[11],[12]. Como tratamiento conservador, dos estudios usaron órtesis [9],[10], uno utilizó órtesis o yeso [11] y uno corsé [12]. Como tratamiento quirúrgico, dos estudios usaron fijación con instrumentación [10],[11], un estudio utilizó estabilización posterior con injerto transpedicular o fusión posterolateral [12] y un estudio no lo específicó [9].
|
|
Qué tipo de desenlaces midieron
|
Se midió dolor según escala visual análoga (EVA). Se evalúo funcionalidad y calidad de vida con el Oswestry back pain questionnaire, Roland Morris Disability Questionnaire (RMDQ), Greenough Low Back Outcome Score (GLBOS) y con el SF 36 (Short form-36). Se evalúo la progresión radiográfica de la cifosis, la necesidad de reintervención, el deterioro neurológico y las complicaciones del tratamiento. Otros desenlaces medidos fueron tiempo de retorno al trabajo, progresión de la estenosis del canal espinal, costos del tratamiento y duración de la hospitalización.
|
[90
Resumen de los resultados
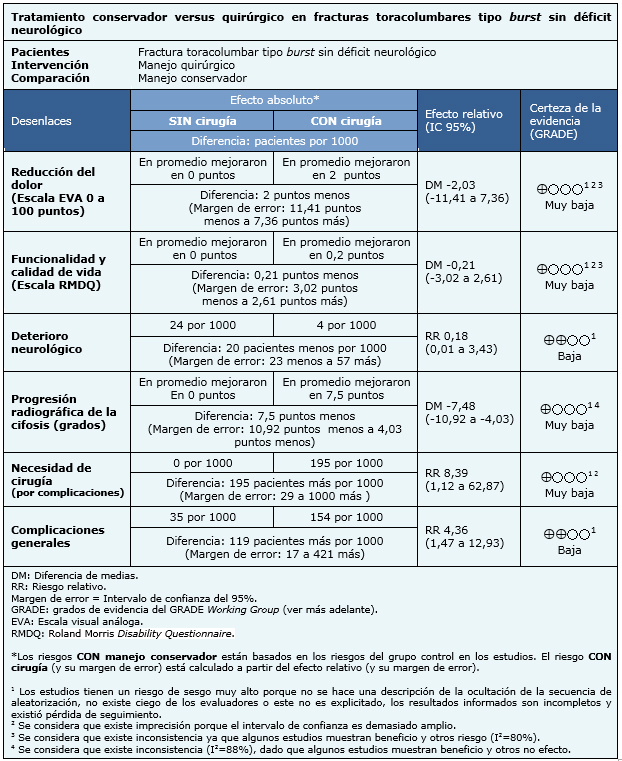
La información sobre el tratamiento conservador versus quirúrgico en fracturas toracolumbares tipo burst sin déficit neurológico está basada en cuatro estudios aleatorizados que incluyen 201 pacientes. Tres estudios evaluaron dolor según escala visual análoga (EVA) [10],[11],[12]. Dos estudios evaluaron funcionalidad y calidad de vida según Roland Morris Disability Questionnaire [9],[10],[11],[12]. Todos los estudios reportaron progresión radiográfica de la cifosis (grados) y deterioro neurológico [9],[10],[11],[12]. Finalmente tres estudios evaluaron necesidad de reintervención y complicaciones generales [10],[11],[12].
- El tratamiento quirúrgico de las fracturas toracolumbares tipo burst podría disminuir el riesgo de deterioro neurológico en comparación con el tratamiento conservador. La certeza de la evidencia es baja.
- El tratamiento quirúrgico de las fracturas toracolumbares tipo burst podría asociarse a mayores complicaciones generales en comparación con el tratamiento conservador. La certeza de la evidencia es baja.
- No está claro si existen diferencias en cuanto a reducción del dolor entre el tratamiento quirúrgico o el conservador de las fracturas toracolumbares tipo burst porque la certeza de la evidencia es muy baja.
- No está claro si existen diferencias en funcionalidad o calidad de vida entre el tratamiento quirúrgico o el conservador de las fracturas toracolumbares tipo burst porque la certeza de la evidencia es muy baja.
- No está claro si existen diferencias en la necesidad de reintervención entre el tratamiento quirúrgico o el conservador de las fracturas toracolumbares tipo burst porque la certeza de la evidencia es muy baja.
- No está claro si existen diferencias en la progresión radiológica de la cifosis entre el tratamiento quirúrgico o el conservador de las fracturas toracolumbares tipo burst porque la certeza de la evidencia es muy baja.

Otras consideraciones para la toma de decisión
|
A quién se aplica y a quién no se aplica esta evidencia
|
- Los estudios incluidos evaluaron a pacientes adultos con fractura toracolumbar tipo burst traumática sin déficit neurológico. Se excluyen por tanto, pacientes con fractura vertebrales en hueso patológico osteoporótico o tumoral (metástasis o primario) o con déficit neurológico al ingreso. No hubo restricción de pacientes según comorbilidad o uso de fármacos.
|
Sobre los desenlaces incluidos en este resumen
|
- Se incluyeron desenlaces considerados críticos para la toma de decisión a juicio de los autores de este resumen. Estos coinciden con aquellos presentados en las principales revisiones sistemáticas identificadas.
|
Balance riesgo/beneficio y certeza de la evidencia
|
- La evidencia existente muestra un posible beneficio del tratamiento quirúrgico con respecto al deterioro neurológico, pero con mayor riesgo de complicaciones generales.
- La principal ventaja del tratamiento conservador es evitar las complicaciones perioperatorias, incluyendo: infección, lesión neurológica iatrogénica, pseudoartrosis, falla de la instrumentación y complicaciones relacionadas con la anestesia.
- No existe una opción que sea claramente preferible, por lo que es fundamental realizar la toma de decisión compartida con el paciente para evaluar los riesgos y beneficios del tratamiento conservador versus el quirúrgico.
|
| Qué piensan los pacientes y sus tratantes |
- Es posible que muchos de los pacientes y tratantes pongan mayor valor en la prevención del deterioro neurológico y se inclinen por el tratamiento quirúrgico a pesar de la baja certeza de la evidencia.
- Pacientes aversos al riesgo, o con mayor riesgo quirúrgico por patologías de base o por otras complicaciones producto del trauma podrían inclinarse por el manejo conservador.
|
Consideraciones de recursos
|
- Debido al alto grado de incertidumbre sobre los beneficios y riesgos es difícil realizar un adecuado balance. Considerando que ambas alternativas tienen superioridad sobre la otra en cuanto a algún desenlace crítico para la toma de decisión, se necesitaría una evaluación más formal del costo-beneficio, además de una mejor base de evidencia, para poder establecer qué opción es superior.
|
|
Diferencias entre este resumen y otras fuentes
|
- Las conclusiones de este resumen concuerdan parcialmente con las revisiones sistemáticas más recientes, que incluyen el total de los estudios identificados.
- Las conclusiones de este resumen están en acuerdo parcial con las recomendaciones de la principal guía clínica [13]. Se revisó la guía de la American Academy of Orthopaedic Surgeons (AAOS), la cual sugiere que el tratamiento conservador debe ser considerado como método inicial de elección, incluso en casos límites donde la ausencia de lesión neurológica o inestabilidad no queda completamente clara, basándose en que las ventajas de la cirugía no se encuentran bien definidas. Es importante considerar que esta guía, del año 2004, incluye una proporción baja de la evidencia identificada en este resumen, en parte porque no estaba disponible al momento de su realización.
|
| ¿Puede que cambie esta información en el futuro? |
- La probabilidad que futura evidencia cambie las conclusiones de este resumen es moderada, debido a la baja certeza de la evidencia.
- No existen estudios en curso o nuevos respecto a esta materia.
|
Notas
Si con posterioridad a la publicación de este resumen se publican nuevas revisiones sistemáticas sobre este tema, en la parte superior de la matriz se mostrará un aviso de “nueva evidencia”. Si bien el proyecto contempla la actualización periódica de estos resúmenes, los usuarios están invitados a comentar en Medwave o contactar a los autores mediante correo electrónico si creen que hay evidencia que motive una actualización más rápida.
Luego de crear una cuenta en Epistemonikos, al guardar las matrices recibirá notificaciones automáticas cada vez que exista nueva evidencia que potencialmente responda a esta pregunta. El detalle de los métodos para elaborar este resumen están descritos aquí: http://dx.doi.org/10.5867/medwave.2014.06.5997.
La Fundación Epistemonikos es una organización que busca acercar la información a quienes toman decisiones en salud, mediante el uso de tecnologías. Su principal desarrollo es la base de datos Epistemonikos (www.epistemonikos.org).
Los resúmenes de evidencia siguen un riguroso proceso de revisión por pares interno.
Declaración de conflictos de intereses
Los autores declaran no tener conflictos de intereses con la materia de este artículo.

Esta obra de Medwave está bajo una licencia Creative Commons Atribución-NoComercial 3.0 Unported. Esta licencia permite el uso, distribución y reproducción del artículo en cualquier medio, siempre y cuando se otorgue el crédito correspondiente al autor del artículo y al medio en que se publica, en este caso, Medwave.




