Reporte de caso
← vista completaPublicado el 24 de abril de 2021 | http://doi.org/10.5867/medwave.2021.03.8176
Cetoacidosis diabética severa precipitada por COVID-19 en pacientes pediátricos: reporte de dos casos
Severe diabetic ketoacidosis precipitated by COVID-19 in pediatric patients: Two case reports
Resumen
Introducción La relación entre la enfermedad por el coronavirus de 2019 (COVID-19) secundaria a SARS-CoV-2 y la diabetes mellitus es bidireccional. Por un lado, la diabetes mellitus se asocia con un mayor riesgo de COVID-19 grave. Por otro lado, en pacientes con COVID-19 se han observado diabetes mellitus de nueva aparición con presentaciones de cetoacidosis diabética y complicaciones metabólicas graves de dicha presentación.
Casos clínicos En este informe, describimos a dos pacientes pediátricos con diabetes mellitus que acudieron a nuestro hospital con cetoacidosis diabética, de debut inicial. Describimos la evolución y el manejo clínico y terapéutico durante la pandemia de COVID-19.
Conclusión La infección por COVID-19 puede precipitar complicaciones como cetoacidosis diabética severa.
Ideas clave
- En el caso de los niños afectados por COVID-19, si bien suelen tener curso asintomático y con menor letalidad, se han descrito presentaciones extrapulmonares diferentes a la etapa de adulto, lo que representa un reto para sus tratantes.
- La diabetes mellitus suele debutar con cetoacidosis. Esta enfermedad se ha asociado a más complicaciones en adultos infectados por el nuevo coronavirus, aunque esto no ha sido demostrado en población pediátrica.
- Pacientes pediátricos con o sin historia de diabetes pueden presentar cetoacidosis severa y COVID-19 tal como los casos incluidos en este reporte.
- Esta asociación debe ser reconocida por pediatras que manejen dichos pacientes para prevenir cetoacidosis. Si los pacientes presentan cetoacidosis debe considerarse cuidados críticos para el manejo de dichos pacientes.
Introducción
Desde que fue clasificada como pandemia, la infección por COVID-19 por el nuevo coronavirus SARS-CoV-2 se ha comportado como una enfermedad que afecta predominantemente el aparato respiratorio, con una mayor letalidad en el grupo de adultos (hombres mayormente) en la sexta década de la vida[1].
El acondicionamiento de todos los sistemas de salud de los países ha tenido que priorizar sus recursos humanos y económicos en su contención. En consecuencia, otras enfermedades crónicas se han visto exacerbadas debido a un mal control[2].
En el caso de los niños, la infección por COVID-19 se ha comportado en su mayoría con un curso asintomático y con menor letalidad. Sin embargo, se han descrito presentaciones extrapulmonares diferentes a la etapa de adulto, representando un reto para quienes asisten a estos enfermos[3]. Las series de casos y los estudios transversales han permitido identificar una mayor proporción de complicaciones en aquellos niños con comorbilidades, que incluso condicionan que debuten algunas enfermedades.
La diabetes mellitus suele debutar con cetoacidosis en 43% de los casos, y en 59% se ha identificado coexistencia de enfermedades infecciosas[4],[5]. Esta patología y sus complicaciones han sido asociadas a una mayor probabilidad de complicaciones en los adultos infectados por el nuevo coronavirus. Sin embargo, esto aún no ha sido demostrado en población pediátrica. El propósito de este artículo es informar de la posible exacerbación de diabetes mellitus durante la pandemia de COVID-19.
Método
Bajo la metodología de las guías CARE (CAse REports)[6] se presentan dos casos de pacientes menores de 18 años con diagnóstico de infección por SARS-CoV-2 (detectado por prueba de reacción en cadena de la polimerasa para dicho virus) y cetoacidosis diabética (acidemia con pH menor de 7,31, glucosa mayor de 350 miligramos por decilitro, cetonas en orina), de un hospital de tercer nivel de atención.
Caso 1
Hombre de 11 años, con obesidad según índice de masa corporal mayor a 95% por gráficos de la Organización Mundial de la Salud.
Antecedentes heredofamiliares positivos para diabetes mellitus tipo 2 en padre y abuelo paterno. Fue contacto de un familiar cercano confirmado (padre) de SARS-CoV-2.
Cuadro clínico
El paciente refirió sintomatología respiratoria inicialmente y luego presentó poliuria, polidipsia, polifagia y pérdida de peso de 10 kilogramos durante quince días previos al ingreso. Al ingreso la prueba de anticuerpos para COVID 19 (inmunoglobulinas G y M) fue positiva y se documentó la infección por SARS-CoV-2 por prueba molecular positiva de hisopado nasofaríngeo. El paciente presentó dificultad respiratoria y alteraciones en el estado de conciencia, recibiendo terapia con oxígeno, seguido de evento de asistolia que requirió maniobras de reanimación y soporte ventilatorio. Los exámenes de laboratorio basales fueron: glucosa sérica de 600 miligramos por decilitro, gasometría con acidemia metabólica descompensada, concentración de bicarbonato menor de 10 milimol por litro, cetonuria. Los marcadores inflamatorios fueron: proteína C reactiva cuantitativa superior a 200 miligramos por litro, leucocitosis, anemia y trombocitopenia, hipoalbuminemia, dímero-d superior a 20 nanogramos por litro (Tablas 1 y 3).
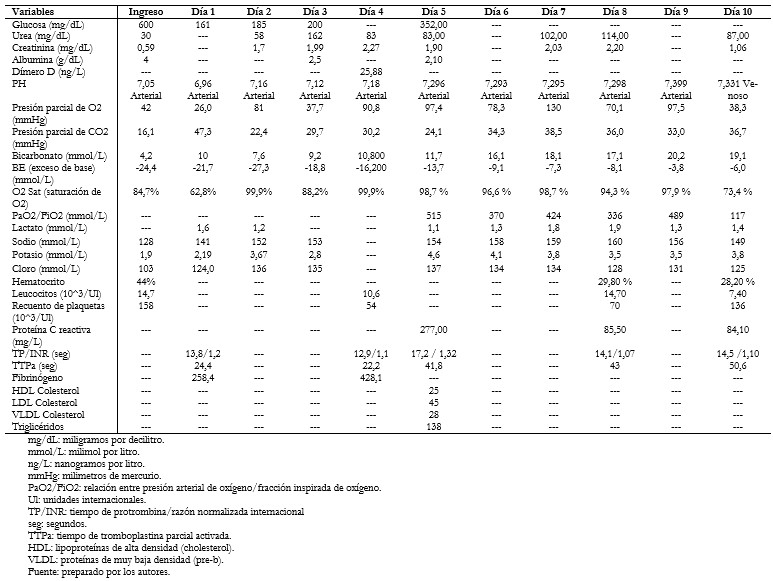 Tamaño completo
Tamaño completo El manejo inicial se basó en rehidratación parenteral de las pérdidas e infusión con insulina rápida de 0,05 a 0,1 unidades por kilo por hora durante 7 días. Luego de mejoría clínica y del estado ácido básico se indicó insulina humana de acción intermedia y rápida a escala móvil según niveles de glicemia.
La condición respiratoria evaluada por radiografía de tórax demostró alteraciones alveolos intersticiales sugestivas de neumonía tipo COVID-19, de grado leve (Figura 1).
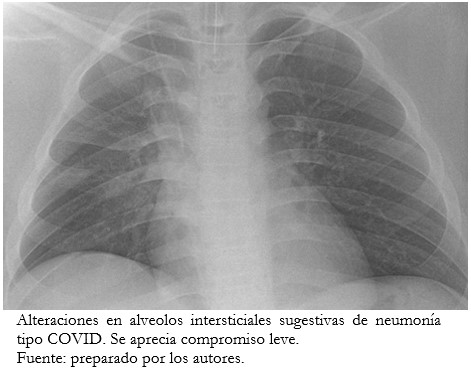 Tamaño completo
Tamaño completo Durante la evolución se presentó encefalopatía secundaria a daño hipóxico agudo leve y edema cerebral, manteniéndose bajo sedación y analgesia con propofol en infusión, más fentanilo en infusión. Para el estado hemodinámico se trató con noradrenalina en rango 0,05 a 0,2 microgramos por kilo por minuto durante seis días. Presentó retención urémica y oligoanuria que evolucionó favorablemente. Luego de seis días de ventilación mecánica, se inició destete de sedoanalgesia y de ventilación mecánica. No se documentó déficit neurológico. A los ocho días se procedió con protocolo de extubación COVID-19, y se progresó con mascarilla Venturi a fracción inspirada de oxígeno de 0,6%. Se indicó cobertura antibiótica empírica para infección nosocomial y para bacterias atípicas con ceftriaxona a 100 miligramos por kilo al día y clindamicina a 30 miligramos por kilo al día, por 7 días. Se decidió agregar enoxaparina a dosis anticoagulante 1 miligramo por kilo por dosis.
El paciente mejoró progresivamente y pudo egresarse al domicilio con tratamiento basado en insulina humana de acción intermedia e insulina rápida a escala móvil, según serología de glicemias seriadas.
Caso 2
Mujer de 8 años, con antecedente positivo desde los 5 años de diabetes mellitus insulinodependiente, controlada. La paciente fue contacto (vecina) de un caso confirmado de COVID-19. Manifestó cuadro clínico compatible con sintomatología urinaria (disuria, piuria, fiebre) y se documentó la infección por SARS-CoV-2 por prueba molecular hisopado nasofaríngeo.
En su evolución, la paciente presentó durante 18 horas vómitos, disnea, respiración de Kussmaul e hipoactividad. Por este motivo fue atendida en el servicio de urgencias, en el cual se corroboró el diagnóstico de cetoacidosis diabética (Tablas 2 y 3) y se inició tratamiento con reanimación hídrica, infusión insulina rápida 0,05 a 0,1 unidades por kilo cada hora y cobertura empírica de antimicrobianos. La radiografía de tórax no demostró imágenes compatibles con patrón reticulonodular (Figura 2).
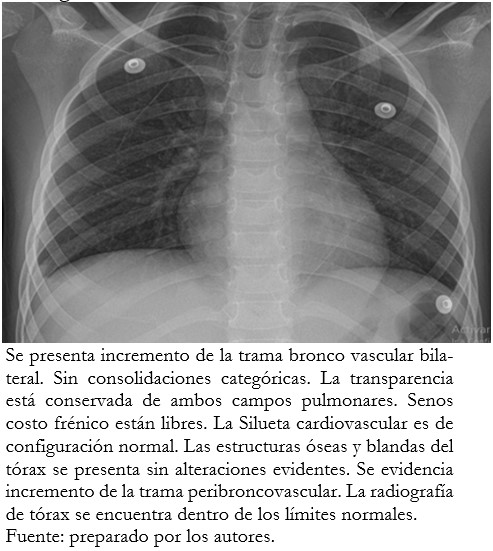 Tamaño completo
Tamaño completo Durante su evolución fue hospitalizada en una unidad de terapia intensiva, donde se brindó la terapia de hidratación y el control antimicrobiano empírico (amikacina) para un cuadro probable de infección de vías urinarias. Durante la evolución se documentó la expresión de anticuerpos inmunoglobulinas G y M para virus de SARS-CoV-2. La evolución fue favorable y fue egresada con insulina glargina e insulina rápida a escala móvil según controles glicemia sérica.
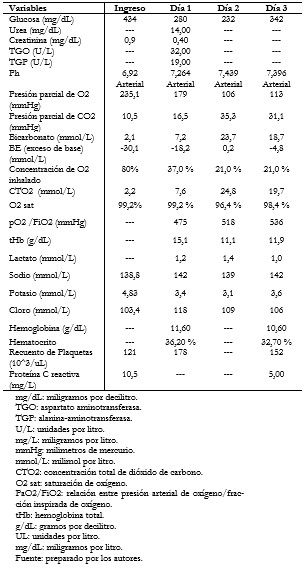 Tamaño completo
Tamaño completo 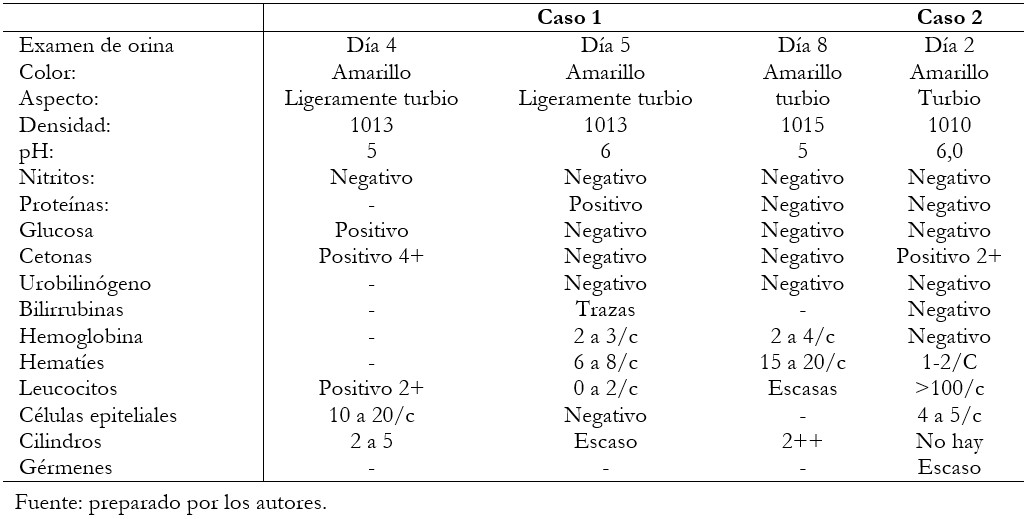 Tamaño completo
Tamaño completo Discusión
En los dos casos presentados se demostró una coexistencia de cetoacidosis diabética y la infección por el nuevo coronavirus.
El primer caso corresponde a un paciente con la comorbilidad de obesidad que debutó con la complicación de cetoacidosis diabética coexistente con las manifestaciones pulmonares de la infección por COVID-19. El segundo caso es una paciente pediátrica con diagnóstico preexistente de diabetes mellitus, que desarrolló cetoacidosis diabética e infección por COVID-19 sin manifestaciones pulmonares.
Estos dos casos recalcan la importancia de continuar con control adecuado de condiciones metabólicas, las que podrían empeorar debido a una infección por el SARS-CoV-2. Es importante reconocer este factor en los médicos responsables de la salud de pacientes con condiciones crónicas, como obesidad y diabetes mellitus, ya que son poblaciones en riesgo de peores morbilidades. Esto fue descrito por Kamrath y colaboradores en el estudio realizado en Alemania, donde describieron un incremento significativo de casos de cetoacidosis diabética severa durante la pandemia[7]. La presentación con cetoacidosis diabética podría ser letal si no se compensa y trata a tiempo. El primer caso presentó edema cerebral y paro cardiorrespiratorio. Ambos pacientes requirieron manejo en cuidados intensivos con estancia hospitalaria prolongada. Estos dos casos sin previos controles rutinarios ni seguimiento metabólico, fueron afectados por la pandemia antes de ser diagnosticados de cetoacidosis diabética. Es por este motivo, que surge el interés de correlacionar la descompensación y precipitación en un cuadro grave como la cetoacidosis diabética severa por la infección por COVID-19, y la necesidad del manejo en terapia intensiva pediátrica. Estos casos sugieren que los niños con trastorno metabólico sin seguimiento endocrinológico, son parte de las poblaciones más vulnerables a infección por COVID-19 y podrían desarrollar una descompensación severa, lo cual incrementa la mortalidad y la estancia hospitalaria.
En cuanto a la relación de diabetes mellitus y COVID-19, Samir y colaboradores describieron en 86 niños con diabetes mellitus e infección por COVID-19 que desarrollaron un cuadro leve, requiriendo cinco de ellos hospitalización en unidad de terapia intensiva. Todos los casos estudiados mantuvieron un control terapéutico de los niveles de glucosa durante la infección[8].
Por su parte, en un estudio italiano a modo de cuestionario en los centros incluidos, reportaron un número menor de casos nuevos de diabetes mellitus en pediatría, pero un mayor número de casos con presentación de cetoacidosis severa[9]. Un estudio similar en Estados Unidos basado en un registro de calidad de casos nuevos de diabetes mellitus, no encontró diferencia en cetoacidosis diabética en casos con o sin COVID-19. Sin embargo, los autores discuten que el número de casos de cetoacidosis es mayor que otros años en el mismo registro[10]. Un estudio de base de datos en Australia describió una mayor frecuencia de cetoacidosis diabética severa durante la pandemia[11].
Una pregunta que estos estudios plantean es si este incremento de frecuencia de cetoacidosis es parte de la fisiopatología del virus o si está relacionado con los cambios sociales impuestos para controlar la pandemia, como menor acceso a controles de salud o postergar las visitas a las emergencias aumentado la severidad de presentación.
Juyi Li, estudió a 658 pacientes adultos hospitalizados con COVID-19 confirmado, 42(6,4%) de ellos presentaron cetoacidosis diabética al ingreso como primera manifestación, los mismos que presentaron una mayor estancia intrahospitalaria y mortalidad[12].
Se precisa realizar estudios de causalidad para determinar si hay una afectación a nivel celular pancreática que acelere la lesión en los pacientes que debutan con diabetes mellitus[13]. Los reportes de pacientes con COVID-19 con síndrome inflamatorio multisistémico en niños presentan también pancreatitis[14]. Los estudios de amilasa y lipasa no fueron obtenidos en nuestros pacientes, ya que la evolución fue favorable.
Un importante aspecto de salud pública es evitar hospitalización por condiciones prevenibles y tratables. El aumento de la seroprevalencia para SARS-CoV-2 y la reducción de la oferta de servicios de salud durante la pandemia, pone de relevancia analizar y reorientar el flujo de pacientes en el ámbito intrahospitalario, con el objetivo de optimizar los recursos con los que contamos. Es importante que esta información sea conocida por médicos que atienden pacientes pediátricos en situación de emergencia para tener las precauciones adecuadas. Los pacientes con COVID-19 pueden presentar cetoacidosis y esto debe ser considerado en el manejo.
Conclusiones
Estos casos muestran que COVID-19 puede precipitar cetoacidosis severa. Estos pacientes pueden presentar mayores complicaciones que otras formas leves de presentación.

