Estudio cualitativo
← vista completaPublicado el 12 de diciembre de 2016 | http://doi.org/10.5867/medwave.2016.11.6798
Aspectos cualitativos del proceso del Programa de Tamiz Auditivo Neonatal en México evaluados desde la perspectiva parental
Qualitative aspects of the process of Neonatal Hearing Screening Program in Mexico evaluated from the parental perspective
Resumen
INTRODUCCIÓN El Programa de Tamiz Auditivo Neonatal Universal se inició en México en 2010. Sus resultados, publicados en 2013 por el Consejo Nacional para el Desarrollo y la Inclusión de las Personas con Discapacidad, informan baja cobertura. Actualmente hay escasez de información sobre sus actividades. Este estudio describe el proceso del programa desde la perspectiva epistemológica de mujeres cuyos hijos participaron en el mismo, evaluándolo bajo el sustento del modelo constructivista-respondente en busca de aspectos que puedan ayudar a explicar sus resultados.
MÉTODOS Estudio de tipo mixto, con enfoque en el paradigma constructivista respondente. En él participaron 14 mujeres, elegidas por juicio y su número hasta la saturación teórica. A ellas, previa firma de consentimiento informado, respetando la confidencialidad y anonimato; se les aplicaron entrevistas semi estructuradas. Estas fueron audio grabadas y transcritas tal como se expresaron. Las investigadoras analizaron y codificaron categorías por separado; juntas resumieron categorías y subcategorías. La validez y confiabilidad se obtuvieron a través de la credibilidad, transferibilidad y triangulación.
RESULTADOS De los discursos se obtuvieron el perfil general de las entrevistadas, evolución de sus hijos en el proceso del programa y cuatro categorías con 15 subcategorías relacionadas con la reconstrucción del proceso: conocimientos, necesidades, sentimientos y actitudes. Estas categorías se evaluaron como favorable (una), sin acuerdo (seis) y desfavorables (ocho). Estas últimas, son propias de nuestro contexto.
CONCLUSIONES La perspectiva epistemológica de las entrevistadas, mostró aspectos que podrían ayudar a explicar la baja cobertura del programa. Retomarlo desde las políticas públicas puede mejorarlo. Con el establecimiento del programa, los niños con sordera son diagnosticados e intervenidos a menor edad que antes del programa.
Introducción
La creación de programas de tamiz auditivo neonatal universal se inició en países desarrollados entre 1964 y 1996. En Latinoamérica esto sucedió en 1993 [1] y en México en 2010, como una acción de políticas públicas dentro del Plan de Desarrollo 2007-2012. Estas políticas se desarrollaron en conjunto con el “Seguro para una nueva generación”, como apoyo económico para los nacidos a partir de 2006 [2].
Actualmente, hay 18 hospitales del gobierno de la Ciudad de México aplicando el Tamiz Auditivo Neonatal. Estos son siete hospitales generales: La Villa, Iztapalapa, Ticomán, Enrique Cabrera, Milpa Alta, Gregorio Salas y Xoco; siete hospitales materno-infantiles: Inguarán, Tláhuac, Magdalena Contreras, Topilejo, Cuajimalpa, Nicolás M. Cedillo y Cuautepec; el hospital de especialidades Belisario Domínguez; el hospital materno-pediátrico Xochimilco y los hospitales pediátricos de Peralvillo y Coyoacán; además de cinco unidades para confirmar el diagnóstico y ocho para tratamiento quirúrgico.
En los estados de la República Mexicana se incluyeron en el programa casi 500 hospitales materno-infantiles de la Secretaría de Salud y 49 unidades médicas para diagnóstico auditivo. Sus actividades fueron reportadas en el boletín del Consejo Nacional para el Desarrollo y la Inclusión de las Personas con Discapacidad. La evaluación del programa se hizo en 2013, publicando sus resultados con un enfoque positivista y confrontando objetivos contra indicadores (porcentaje de niños tamizados, diagnosticados, tratados). Estos resultados muestran baja cobertura e inconsistencia en la información [3],[4]. Actualmente, sólo hay reportes de estas actividades a través de notas periodísticas y algunos artículos publicados [5],[6],[7].
La evaluación de programas y sistemas comenzó en Estados Unidos hace 50 años, en las áreas de capacitación laboral y educativa. Posteriormente, se desarrolló en programas de salud (adicciones, planificación familiar, salud reproductiva y recientemente salud pública) [8]. En Latinoamérica, su incorporación ha sido lenta. En México se inició en 1917, intensificándose en la década de los sesenta y sistematizándose en 1997 con los programas de educación, salud y alimentación [9].
En general, la evaluación consiste en hacer un juicio sobre un objeto, situación o proceso. Sin embargo, deberá ser sistemática con procedimientos que garanticen la validez y fiabilidad por medio de una investigación evaluativa, cuyos métodos y técnicas sean los mismos que se utilizan en investigación social [10].
La evaluación ha sido impulsada por estudiosos del tema, y no precisamente teóricos, quienes en los años sesenta impulsaron múltiples iniciativas para reconceptualizar el término y proponer nuevos modelos evaluativos. Así, crearon cinco generaciones de modelos con objetivos que han cambiado su modo de evaluar. Se inició con la medición y continuó con la descripción, emisión de juicio y participación negociada de los involucrados, confrontándose en una guerra de paradigmas [11]. En este contexto, se entiende como paradigma un sistema básico de creencias, basado en supuestos ontológicos, epistemológicos y metodológicos, que representan la visión del mundo o sus partes. Estos supuestos definen para el investigador lo que está haciendo, así como lo que hay dentro y fuera de los límites de una investigación legítima [12].
El modelo evaluativo constructivista respondente, propuesto en 1984 por E. Guba e I. Lincoln, pertenece a la cuarta generación de estos modelos. Él da inicio al enfoque cualitativo de la evaluación. Pertenece a un paradigma cuya ontología presenta la realidad por medio de construcciones mentales múltiples, basadas en la experiencia social y naturaleza local que pueden compartirse entre diferentes individuos y culturas. Su epistemología es transaccional y subjetivista (vinculación entre investigador y objeto investigado). Los hallazgos se construyen al avanzar la investigación y su metodología se caracteriza por ser holística. Es decir, es un estudio de la realidad desde una mirada global e inductiva. Las categorías, patrones e interpretaciones se elaboran a partir de la información obtenida de los participantes, mas no a partir de teorías o hipótesis previas. Es ideográfica, pues en ella se orienta, comprende e interpretan los fenómenos sociales con técnicas hermenéuticas y dialécticas.
Sus construcciones sociales e individuales son variables producidas y refinadas por medio de la interacción entre investigador y quien las aporta, interpretando, comparando y contrastando en intercambio dialéctico. Este intercambio construye el etic del investigador a partir de las construcciones emic de los participantes [13], aplicadas en la presente investigación.
Young, A. y Tattersall, H. consideran que la perspectiva parental tiene un valor epistemológico haciendo mención sobre la posición de este valor. Además, comentan sobre los pocos estudios relacionados con la investigación evaluativa de los programas de tamiz auditivo neonatal sustentados en modelos evaluativos [14]. Esto porque la mayoría de las publicaciones al respecto, se han dirigido a obtener de los padres el grado de satisfacción o problemas específicos del tamiz auditivo neonatal por medio de cuestionarios, encuestas telefónicas y entrevistas. En su mayoría han sido por medio de un enfoque cuantitativo [15],[16],[17],[18] y los menos con un enfoque cualitativo [19],[20],[21],[22]. Sin embargo, los estudios no se han centrado en el proceso global del programa Tamiz Auditivo Neonatal (tamiz, diagnóstico, intervención, implante coclear).
El presente estudio se realizó con la finalidad de evaluar cualitativamente este proceso desde la perspectiva parental, buscando aspectos que pudieran ayudar a explicar sus resultados a través del modelo constructivista respondente. Asimismo, se hizo un análisis cuantitativo de las características de las participantes y la evolución cronológica de sus hijos durante su participación en algunas o las cuatro etapas del Programa de Tamiz Auditivo Neonatal.
Métodos
Diseño
Se trata de un estudio de tipo mixto, donde el enfoque cualitativo se basa en el modelo evaluativo constructivista respondente de Guba y Lincoln. El aspecto cuantitativo se sustenta en la descripción de variables demográficas de las participantes y cronológicas de sus hijos, durante el proceso del programa Tamiz Auditivo Neonatal.
Las participantes se definieron por conveniencia [23], elaborando un perfil de informantes de acuerdo con los siguientes criterios: mujeres cuyos hijos nacieron a partir de 2010 en alguno de los hospitales materno infantiles incluidos dentro del Programa de Tamiz Auditivo Neonatal, o que fueron llevados para su tamizaje participando en una o más etapas del programa. El número de entrevistadas se determinó de acuerdo con el criterio de saturación teórica [24].
El investigador principal presenta una experiencia en el tema de 12 años aproximadamente, con conocimientos teóricos sobre los programas de tamiz auditivo y práctica del mismo, pero no dentro del actual programa.
La relación con las entrevistadas fue con respeto y ética, guiando las entrevistas con una lista de preguntas relacionadas con las etapas del programa, dando libertad para el discurso y permitiendo la expresión de sus emociones.
Debido a que el proceso del programa se lleva a cabo en diferentes unidades médicas (tamizaje, diagnóstico, tratamiento), fue necesario trasladarse hacia algunas de ellas dentro de la Ciudad de México, previa autorización del personal responsable de las áreas de audiología y de la práctica del tamiz auditivo de dos hospitales materno-infantiles, un hospital general y un instituto de tercer nivel de atención de la Secretaría de Salud.
Se acudió a las salas de espera donde asisten madres con sus hijos para el tamiz, a confirmar el diagnóstico y/o a las áreas de terapia de lenguaje. A las 14 participantes se les solicitó la firma del consentimiento informado. Se les realizó una entrevista semi estructurada a través de una guía de preguntas dadas sin orden específico, evitando las que aportaron su respuesta dentro del discurso. La encuesta duró entre 40 y 50 minutos, y se aplicó entre agosto de 2014 y marzo de 2015. Estas entrevistas se grabaron en audio y se transcribieron, tal y como fueron expresadas (emic). Las entrevistadas presenciaron la lectura de la transcripción para confirmar o rechazar su dicho. Esto se realizó sólo en quienes llevaban a terapia de lenguaje a sus hijos, las otras ya no regresan al hospital. Luego, las entrevistas fueron reducidas a etic, sin perder su esencia.
Cada una de las investigadoras por separado utilizó el análisis de contenido latente para identificar, codificar y categorizar patrones primarios relacionados con el proceso del programa. Se utilizaron las letras del abecedario en español, sustituyendo los nombres de las entrevistadas para garantizar su confidencialidad, anonimato y privacidad. Las categorías y subcategorías se ordenaron de acuerdo al modelo respondente. Éstas fueron “problemas”: no hubo acuerdo entre las entrevistadas sobre algunos aspectos del proceso; “preocupaciones”: se evaluaron como desfavorables dichos aspectos; y “reivindicaciones”: se les consideró favorables.
El rigor científico se obtuvo a través de los criterios de credibilidad (construcción de las participantes y reconstrucción del investigador principal, acorde a lo que piensan y sienten ellas); transferibilidad, analizando el ajuste de los resultados con otro contexto (el proceso es semejante en todos los hospitales incluidos en el programa); y triangulación, confrontando las diferencias de acuerdo y desacuerdo de los discursos, y corroborando los datos en las historias clínicas de los niños y en la bitácora de resultados diarios del tamizaje.
Resultados
Se hizo uso de la estadística descriptiva para analizar y presentar el perfil demográfico de las 14 entrevistadas participantes, cuyos datos mostraron: edad entre 19 y 38 años con un promedio de 26; 10 casadas (72%), 13 dedicadas al hogar (93%), con un nivel de estudios de preparatoria para seis (42%), seis con problemas en el embarazo (42%) y en 12 el nacimiento de sus hijos fue por cesárea, de las que nueve (65%) fueron no programadas. Los hospitales donde fueron atendidas están ubicados: seis en el Estado de México, cuatro en tres Estados de la República Mexicana y cuatro de la Ciudad de México (Tabla 1).
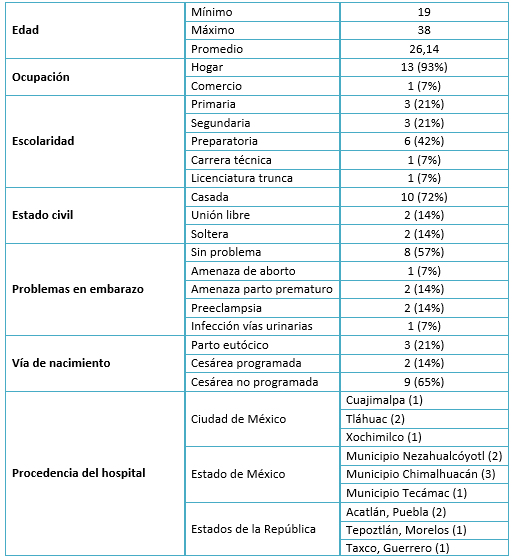 Tamaño completo
Tamaño completo Asimismo, los datos relevantes de sus hijos fueron: la edad al momento de este estudio fue entre un mes y cuatro años, con un promedio de 1,8 años; en cuanto al sexo, ocho (57%) fueron masculinos y seis (43%) femeninos; y dos (14%) presentaron antecedentes familiares de sordera. La edad al momento del tamiz fue entre cuatro y 180 días de nacidos, con un promedio de 43 días. A siete (50%) se les realizó entre dos y tres veces el tamiz auditivo; la edad promedio del diagnóstico fue de 7,57 meses.
En cuanto al diagnóstico, cinco (36%) presentaron hipoacusia bilateral profunda, dos (14%) hipoacusia unilateral profunda, cuatro (28%) con probable hipoacusia (siguen en estudio) y tres con audición normal bilateral. La edad promedio de inicio de uso de auxiliares auditivos fue a los 18 meses y de terapia de lenguaje a los 13,4 meses. Dos niños fueron tratados con implante coclear a los dos años y 6 meses. Las edades no se ajustan a los objetivos de los programas de tamiz auditivo internacional (Tabla 2).
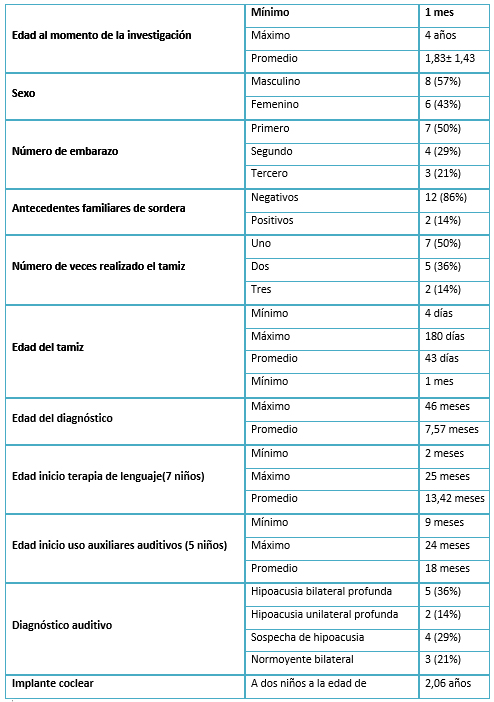 Tamaño completo
Tamaño completo El análisis cualitativo de las construcciones hechas desde la perspectiva parental sobre el proceso del programa Tamiz Auditivo Neonatal e Intervención Temprana, bajo los criterios del modelo evaluativo constructivista respondente, mostró cuatro categorías: conocimientos, necesidades, sentimientos y actitudes con tres, siete, tres y dos subcategorías respectivamente. De estas últimas, siete correspondieron a la etapa del tamiz auditivo, una a la de diagnóstico, cuatro relacionadas con la etapa de tratamiento y tres referidas al programa en general. Del total, ocho fueron organizadas como desfavorables (preocupaciones), de las que cinco correspondieron a la etapa del tamiz y dos al tratamiento. Estas últimas se relacionaron con nuestro contexto en México (Tabla 3).
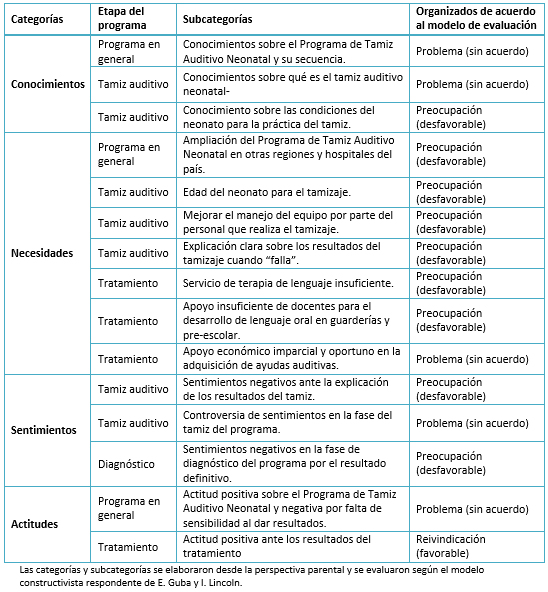 Tamaño completo
Tamaño completo La descripción de categorías y subcategorías se describe a continuación, acompañada de sus testimonios. La categoría I “conocimientos” agrupó tres subcategorías. La primera se vinculó a los conocimientos obtenidos a través de la información entregada a las entrevistadas, sobre lo que es el Programa de Tamiz Auditivo Neonatal y su secuencia. Los resultados mostraron desacuerdo, pues algunas dijeron haber recibido información completa con trípticos, carteles y pláticas en algunos hospitales de la Ciudad de México y el Estado de México; en cambio otras no fueron informadas, lo que ocasionó incluso que a sus hijos no les practicaran el tamiz.
[…] “En el hospital donde nació mi hijo, realizan el tamiz auditivo, hay carteles y ofrecen trípticos, para dar información, y reciben a niños de otros hospitales” […] D
[…] “Me enteré por mi hermano, pues su niño y mi hijo nacieron en el mismo hospital. A su hijo le hicieron la prueba del tamiz auditivo y a mi hijo no” […] A
La segunda subcategoría, sin acuerdo también, se relacionó con el conocimiento sobre lo que es el tamiz auditivo. La información se les dio en las salas del puerperio a algunas de ellas, a otras sólo se les indicó que habrían de realizarle el tamiz a sus hijos.
[…] “Mientras estaba en recuperación me dijeron que tenían que hacerle el tamiz metabólico y el tamiz auditivo a mi bebé, pero no me explicaron en qué consistían” […] M
[…] “Cuando pregunté para qué era ese estudio, me dijo la enfermera para verificar si el bebé escuchaba correctamente, que no era peligroso” […] G
La tercera incluyó la falta de conocimientos sobre las condiciones en que debe presentarse el neonato para el tamiz auditivo. Esta se considera desfavorable, pues a ninguna se le dio información, sólo la indicación de regresar al hospital para el tamiz. Sus discursos ejemplifican las condiciones en que se realizó el estudio.
[…] “El consultorio es pequeño, el ruido es normal, había 3 o 4 enfermeras platicando mientras hacen el estudio. Durante el tamiz los bebés se inquietan porque les ponen unos como taponcitos, y no creo que les duela, dura entre 10 y 15 minutos si se dejan. Te dicen como cargar al niño, le hacen primero de un oído, luego lo volteas del otro oído. Si llora, te dicen que lo tranquilices, te sacan por un momento y luego te vuelven a llamar”[…] E
La categoría II “necesidades” representa condiciones desfavorables en el proceso del programa. Se identificaron siete subcategorías, de las que seis estuvieron ligadas: una con el programa, tres con la práctica del tamiz y tres con el tratamiento.
La primera subcategoría se refiere a la necesidad del programa de tamiz auditivo en otras localidades y hospitales del país. Ello, porque cuando los niños nacen en unidades médicas no incluidas en el programa, algunos son referidos a hospitales con tamiz y otros no, debido al desconocimiento del personal de salud sobre donde se realiza éste.
[…] “En el hospital donde nació mi hijo no hacen el tamiz auditivo. Me dijeron que si tenía oportunidad de hacérselo que buscara a donde llevarlo, ya que era importante para él” […] F
[…] “En Puebla, las clínicas particulares no hacen tamiz auditivo, tienes que ir al hospital general” […] C
[…] “En el hospital donde nació mi hijo no hay tamiz auditivo. Debería estar en todos los hospitales, para prevenir cualquier problema en los oídos de los pequeños” […] G
La subcategoría concerniente con la práctica del tamiz auditivo fue la necesidad de ampliar la edad para el tamizaje, pues la indicación que recibieron fue que se realice entre el cuarto y quinto día de nacidos. Algunas entrevistadas comentaron que habían estado hospitalizadas por diversas causas de salud y que al salir, ya no se los hicieron.
[…] “Se lo realizaron a los 5 días después de que ella nació, no antes de salir del hospital porque tenía que ser 4 o 5 días después del nacimiento así nos lo explicaron” […] N
[…] “Como mi hijo estaba en el alojamiento conjunto dijeron que subirían a hacérselo, pero no subieron y cuando salí del hospital él tenía 15 días de nacido y ya no se lo realizaron, pues debe ser entre el 4 o 5 día de nacidos”[…] K
Otra subcategoría fue la necesidad de que hubiera un mejor manejo de los equipos, al realizar el tamizaje por parte del personal.
[…] “No le pudieron hacer el estudio en tres ocasiones, el doctor decía que se movía mucho y tenía miedo de lastimarla” […] C
[…] “Lo intentaron varias veces con diferentes ‘chuponcitos’ y no respondía, me dijeron que probablemente estaba sucio su oído o algo así y que regresara otro día” […] J
En la tercera subcategoría, sobre la necesidad de recibir una explicación clara sobre los resultados de tamiz cuando “falla”, la explicación produjo confusión y desconfianza en algunas madres, abandonando la secuencia del programa en busca de quien les dé un resultado confiable.
[…] “El tamiz está ‘ruidoso’ me dijeron hasta 3 veces. Nunca me explicaron por qué salía ruidoso.” […] H
[…] “No le pudieron hacer el tamiz en tres ocasiones y nos fuimos como a dos horas de ahí, con una especialista que le revisara sus oídos bien, con certeza” […] C
Las subcategorías referentes con el tratamiento fueron la necesidad de ampliar el servicio de terapia de lenguaje y como aumentarlo en frecuencia y duración.
[…] “Para ingresar a terapia la pusieron en lista de espera porque son bastantes los niños que acuden ahí, así que esperamos a tener lugar. La terapia de lenguaje es necesaria, debiera darse con más frecuencia y durante más tiempo pues tardamos más en ir y venir que el tiempo de terapias” […] C
La necesidad de apoyo para el desarrollo del lenguaje en las guarderías y centros pre-escolares por parte del personal docente es otra subcategoría, pues se requiere como complemento de la terapia de lenguaje.
[…] “En la escuela no la apoyan pues dejan que se comunique con señas. La finalidad es que hable. Ya decía algunas palabras en la casa y ahora nuevamente con señas” […] H
La última subcategoría, relacionada con el tratamiento protésico, las madres mencionaron la necesidad de que haya apoyo económico para todos los niños en la adquisición de auxiliares auditivos e implante coclear. Ello, pues mientras a unas les fueron cubiertos todos los gastos, otras refieren dificultades para adquirirlos por su alto costo, aun participando en programas de donación.
[…] “No me cobraron ni el implante coclear, el Seguro Popular nos está cubriendo todo” […] A
[...] “Me indicaron un auxiliar auditivo, pero no he podido comprarlo. En el programa de donación dijeron que donan dos aparatos y mi hija solo necesita uno. He tenido mala suerte para la donación” […] D
La categoría III fue los “sentimientos” como resultado de las emociones vividas, con tres subcategorías involucradas con su sentir ante los resultados del tamizaje y diagnóstico. La primera de ellas, vinculada a la explicación del resultado del tamizaje, generó sentimientos negativos como angustia, ansiedad y desesperación.
[…] “Me sentí muy angustiada. Eso de que mi hija no escuchara, eso de que fuera sorda, me produjo mucho dolor porque los sordos sufren mucho. No pueden hablar porque no oyen y no pueden hacer una vida normal” […] B
La segunda subcategoría produjo sentimientos positivos en algunas entrevistadas, cuando se les presentaron las ventajas del tamizaje (confianza y seguridad), y después sentimientos negativos ante la explicación de sus resultados.
[…] “Sentí confianza. Este estudio te quita un peso de encima. No duele, es rápido y te da resultados inmediatos” […] J
[…] “Dijeron probablemente el aparatito que tenemos está fallando. ‘Estos aparatitos no son tan confiables’, me dijo la enfermera. Si hubiera otro lugar más confiable la mandaríamos a hacerlo” […] E
La tercera subcategoría concerniente al impacto del resultado del diagnóstico que es definitivo, produjo sentimientos negativos como culpa, dolor, negación y desesperanza.
[…] “Cuando confirmaron que mi hija no oía, me sentí mal porque pensaba que por mi culpa mi niña no escucha. Es algo que tengo a diario presente” […] H
[...] “En ese momento se nos vino el mundo encima porque nosotros teníamos la esperanza de que, a lo mejor, fuera nada más poco o nada más de un lado” […] C
La categoría IV fueron las “actitudes” con dos subcategorías, la primera referente al proceso del programa en general (sin acuerdo). Algunas entrevistadas lo consideraron bueno al experimentar las ventajas de un diagnóstico temprano. Otras, en cambio, lo tomaron con sus reservas pues consideraron que el personal operativo es insensible al dar los resultados.
[…] “El tamiz es bueno porque nos ayuda a darnos cuenta si nuestros niños están bien. Físicamente se ven bien, a veces viene malformado el oído pero no te das cuenta inmediatamente si hay algo malo al interior. Este tipo de programas son necesarios, pues ayudan a las mamás y a sus hijos” […] N
[…] “Es necesario que el personal del programa de tamiz auditivo tenga más de atención y sensibilidad al dar los resultados, porque te dicen ‘tu hija es sorda’. Así de duro. Son crueles, deberían comprender los momentos que estamos pasando. Hay mamás que van solas y al darles los resultados requieren un poco de sensibilidad y apoyo de los médicos en quienes confiamos” […] H
La segunda subcategoría, vinculada con los resultados del tratamiento en la fase final del proceso del programa, se evaluó como favorable ante los resultados en el desarrollo del lenguaje y en los cambios de conducta de los niños.
[…] “Desde el momento en que le pusieron los aparatos ella empezó a balbucear mucho. Antes sólo gritaba, pero sin balbucear ni intentar decir palabras, pero ahora los auxiliares auditivos si le ayudan bastante” […] C
[…] “Con el uso de los auxiliares auditivos no notamos cambios, lo veíamos casi igual. Cuando se implantó a los 3 años 4 meses, poco a poco se fue viendo el avance… pensamos se quedaría como mis tías que son sordomudas, pero ya logramos que nos oyera, lo que falta es que hable más” […] A
Discusión
Pocos estudios han incluido la experiencia de los padres (beneficiarios indirectos de un programa) en una evaluación que describa críticamente los programas y la práctica del tamizaje auditivo [25]. Afortunadamente, la visión de los padres ha sido considerada como un aporte epistemológico. También se reconoce que son pocos los estudios evaluativos sustentados en un modelo de enfoque cualitativo [14].
Tomando en cuenta los resultados obtenidos en la presente investigación, desarrollada dentro de los criterios ontológicos, epistemológicos y metodológicos del modelo evaluativo constructivista respondente; se obtuvo un enfoque global del proceso del programa de Tamiz Auditivo Neonatal e Intervención Temprana que corresponde a su carácter holístico. Metodológicamente las categorías, patrones e interpretaciones se construyeron a partir de los discursos de las entrevistas, derivados y refinados hermenéutica y dialécticamente entre el investigador responsable y las participantes. Los hallazgos fueron creados en el proceso de interacción entre el evaluador y el objeto evaluado, de acuerdo al criterio epistemológico del modelo evaluativo.
De los resultados del programa Tamiz Auditivo Neonatal e Intervención Temprana de 2012, se sabe que la cobertura fue de 65%, cuando se había planeado alcanzar el 80% [4]. Ahora, desde la perspectiva parental, se identificaron siete subcategorías relacionadas con la fase de tamiz auditivo. Dos de ellas están relacionadas con el conocimiento parcial que tienen las madres sobre lo que es el tamiz auditivo, el que consideran erróneamente un estudio diagnóstico, así como el desconocimiento de las condiciones que debe tener el neonato para el tamiz.
Tres subcategorías de esta fase fueron evaluadas como necesidades: la edad del neonato limitada para el tamizaje (sólo lo aplican en la primera semana de nacidos), los problemas relacionadas con el manejo del equipo del tamiz, así como la explicación no clara de los resultados. Esto generó sentimientos controvertidos pues mientras unas participantes tuvieron buenos resultados, otras se encontraron confundidas, provocando incluso que abandonaran la secuencia del programa retrasando el diagnóstico y tratamiento. Estas categorías han sido identificadas como hallazgos en otros estudios sobre resultados del tamizaje auditivo, como son los conocimientos [26],[27], las condiciones del neonato para el tamiz [17], el manejo del equipo para el tamizaje y la falta de una explicación clara sobre sus resultados cuando este falla [16].
En la etapa de diagnóstico sólo se identificaron los sentimientos negativos que siempre acompañan estos casos, pero que requieren mayor apoyo por parte del personal de salud [28],[29]. La etapa del tratamiento está relacionada con las necesidades sobre la adquisición de ayudas auditivas y la baja cobertura del servicio de terapia de lenguaje. Ello es compatible con la baja infraestructura de estos servicios en nuestro país, como lo es la falta de expansión del programa a todo el sector salud. La opinión general del programa fue contradictoria, dependiendo de los resultados que se tienen actualmente con el tratamiento y cómo fue la atención del personal médico durante el proceso. Al final se reconoce como favorable [30].
Los resultados desfavorables en las subcategorías de la fase del tamiz pueden estar incidiendo en la baja cobertura del programa. El desconocimiento, las fallas en la práctica, la confusión que producen los resultados así como la edad limitada para su práctica, retrasan el proceso hacia el diagnóstico temprano. Asimismo, las dificultades para iniciar el tratamiento protésico (pobre acceso económico para ayudas auditivas, retraso en las donaciones), y de terapia de lenguaje (baja infraestructura del servicio en el país), retrasan el proceso en esta etapa. Esto conlleva a que los niños pierdan la oportunidad de recibir un implante coclear por rebasar la edad para este tratamiento.
El perfil de las entrevistadas nos habla de la diversidad territorial de la práctica del tamiz y su contexto nacional. Mientras que el análisis cronológico de la edad de los niños, nos indica que han mejorado relativamente su edad para el diagnóstico e inicio del tratamiento, aún cuando no se han alcanzado los estándares internacionales de los programas de tamiz auditivo universal [31],[32] pues antes que iniciara éste, los niños eran llevados a su primera evaluación entre los 3 y 4 años [33].
La detección de discapacidad auditiva en el Distrito Federal en 2006, a nivel de marginación media, era a la edad de 2,8 y el diagnóstico a los 6,6 años. Mientras, en el nivel de marginación alta la detección se realizaba a los 5,4 y el diagnostico a los 10,4 años lo que habla del pobre acceso a los servicios especializados [34]. Retomar estos resultados en una propuesta de políticas públicas permitirá la mejora del programa Tamiz Auditivo Neonatal e Intervención Temprana. Esto significa difusión, información para las mujeres embarazadas, personal de salud y público en general; así como capacitación continua del personal que lo practica, apoyo a los padres en todas las etapas del programa, monitoreo de los casos, información continua de las actividades del mismo y búsqueda de alternativas de apoyo para el tratamiento protésico, terapéutico y quirúrgico. Sobre todo, implica retomar un programa que beneficia a los niños con discapacidad auditiva y a sus familias.
Conclusiones
La evaluación cualitativa de la perspectiva parental, sustentada en el modelo constructivista respondente, mostró una incidencia mayor de subcategorías desfavorables en la etapa de tamizaje y tratamiento. Estas pueden ser propuestas a través de las políticas públicas para mejora del programa y beneficio de los neonatos con pérdida auditiva y sus familias.
Los niños con deficiencia auditiva provenientes del Programa de Tamiz Auditivo, están reduciendo su edad de asistencia a diagnóstico e inicio de tratamiento, comparados con la edad a la que acudían antes del programa.
Notas
Aspectos éticos
Debido a que la presente investigación se realizó por medio de entrevistas y estas son consideradas como sin riesgo de acuerdo a la Ley general de salud en materia de Investigación para la salud en México, capítulo I, “Aspectos éticos de investigación en seres humanos”, artículo 17, se obtuvo la firma de un consentimiento informado por parte de las entrevistadas. Este requisito es exigido por el personal responsable de las áreas de tamiz, diagnóstico y tratamiento de las unidades médicas donde se realizó la investigación, dispensable por la comisión de ética de acuerdo al artículo 23 de la Ley mencionada, por ser una investigación sin riesgo. Asimismo y considerando los artículos 13 y 16 de esta Ley se utilizaron como seudónimos las letras del abecedario en español para identificar a las participantes garantizando con ello su confidencialidad.
Conflicto de Intereses
Las autoras han completado el formulario de declaración de conflictos intereses del ICMJE traducido al castellano por Medwave, y declaran no haber recibido financiamiento para la realización del reporte; no tener relaciones financieras con organizaciones que podrían tener intereses en el artículo publicado, en los últimos tres años; y no tener otras relaciones o actividades que podrían influir sobre el artículo publicado. Los formularios pueden ser solicitados contactando al autor responsable o a la dirección editorial de la Revista.
Financiamiento
Los autores declaran que no hubo fuentes de financiación externas.

