Estudios originales
← vista completaPublicado el 8 de abril de 2016 | http://doi.org/10.5867/medwave.2016.03.6422
Sepsis neonatal y neurodesarrollo en recién nacidos de muy bajo peso en Matanzas, Cuba 2006-2010: cohorte prospectiva
Neonatal sepsis and neurodevelopment in very low birth weight infants in Matanzas, Cuba 2006-2010: a prospective cohort study
Resumen
INTRODUCCIÓN La sepsis neonatal se ha asociado a peor resultado del neurodesarrollo en recién nacidos de muy bajo peso. En Cuba se desconoce el impacto de la sepsis neonatal en el neurodesarrollo de los recién nacidos de muy bajo peso, egresados de sus unidades de cuidados intensivos neonatales.
OBJETIVO Determinar el impacto de la sepsis neonatal como factor de riesgo de alteraciones del neurodesarrollo en una población de recién nacidos cubanos de muy bajo peso.
MÉTODOS Se realizó un estudio de cohorte con 89 neonatos con peso al nacer <1 500 gramos, atendidos durante el periodo 2006-2010 en el Hospital Gineco-obstétrico Docente Provincial de Matanzas, a los cuales se les realizó un seguimiento longitudinal por consulta externa hasta los dos años de edad corregida. El total de pacientes seguidos se dividió en dos grupos, según hubieran presentado (n=19) o no (n=70) sepsis neonatal. A partir del cálculo del riesgo relativo e intervalos de confianza al 95% (IC 95%), se determinó la fuerza de asociación de la sepsis neonatal con la presencia de alteraciones del neurodesarrollo. Mediante un estudio multivariado con regresión logística, se pudo comparar ésta con otras variables neonatales como factores de riesgo.
RESULTADOS Los recién nacidos de muy bajo peso con sepsis neonatal tuvieron un riesgo incrementado de presentar alteraciones del neurodesarrollo (47,4 versus 17,1%; riesgo relativo 2,7 IC 95% 1,3-5,5; p=0,005). Este riesgo fue significativo con independencia de otras variables (sexo masculino, asistencia respiratoria mecánica, displasia broncopulmonar e hiperbilirrubinemia >15 mg/dl) (odds ratio 4,0; IC 95%: 1,1-14,3; p=0,03).
CONCLUSIONES La sepsis neonatal debe considerarse como una causa importante, dentro de los múltiples eventos causales, de daño cerebral en el recién nacido pretérmino.
Introducción
El nacimiento pretérmino es un fenómeno que ha alcanzado dimensiones sociales, condicionadas por el incremento de la sobrevida de los recién nacidos de muy bajo peso o <1500 gramos y de bajo peso extremo (<1000 gramos). En el año 2010 por ejemplo, se estima que a nivel mundial nacieron 15 millones de niños antes de las 37 semanas de gestación, de los cuales 13 millones sobrevivieron. De estos, 2,7% tuvieron un daño moderado o severo del neurodesarrollo [1].
Hoy en día la sobrevida en los recién nacidos menores de 1500 gramos es superior o igual al 90%, y los déficits motores se presentan aun entre el cinco y 10% de los mismos. Otras discapacidades se presentan entre 25 y 50% de los casos, e incluyen trastornos cognitivos y de conducta [2]. La incidencia de la parálisis cerebral es mucho mayor en los niños extremadamente prematuros, con 17 o 19%, según sean menores de 26 semanas de gestación o de bajo peso extremo [3],[4].
Algunos de los factores de riesgo de mayor importancia para la ocurrencia de alteraciones del neurodesarrollo en niños pretérmino de muy bajo peso y, especialmente de bajo peso extremo, incluyen sexo masculino, no administración de esteroides antenatales, presencia de leucomalacia periventricular, hemorragia intraventricular, convulsiones neonatales, retinopatía de la prematuridad, displasia broncopulmonar, ventilación mecánica prolongada, ductus arterioso persistente, uso de esteroides posnatales, malnutrición, nutrición parenteral prolongada, enterocolitis necrotizante y/o perforación intestinal [5],[6],[7].
En diversos estudios se ha encontrado asociación entre la presencia de infección materna, especialmente corioamnionitis, histológica o clínica, y la presencia de daño a la sustancia blanca o parálisis cerebral, tanto en niños pretérmino como a término [8],[9].
Pero el resultado neurológico adverso en recién nacidos pretérmino no solo se ha asociado a la presencia de infecciones maternas intrauterinas o corioamnionitis, sino también a la sepsis neonatal per se. Los primeros dos estudios realizados en poblaciones de recién nacidos pretérmino extremos, en los cuales se encuentra una fuerte asociación entre la presencia de infección neonatal y peor resultado neurológico en estos niños, fueron publicados hace apenas pocos años [10],[11].
Las infecciones bacterianas continúan siendo causa importante de morbilidad y mortalidad en el período neonatal. Cerca del 1,5% de los recién nacidos de muy bajo peso presentan sepsis de aparición temprana y hasta cerca del 21% presentan sepsis de aparición tardía, con una mortalidad que varía entre 10 y 30%, aunque las incidencias varían según años y regiones [12].
La mayoría de los estudios que han evaluado la asociación de la sepsis neonatal con la ocurrencia de secuelas del neurodesarrollo en recién nacidos de muy bajo peso, han sido llevados a cabo en países desarrollados [12],[13]. De los estudios publicados en Cuba acerca de la asociación de los factores que tienen lugar durante el período neonatal con los resultados del neurodesarrollo en recién nacidos de muy bajo peso [14],[15],[16], ninguno se ha centrado en el estudio del papel de la sepsis neonatal como factor de riesgo en la ocurrencia de trastornos del neurodesarrollo. Ello, a pesar de que la incidencia de sepsis neonatal en este grupo de neonatos es elevada, según lo reportan estudios realizados en este país [17],[18].
De lo anteriormente expresado, se infiere que se desconoce el impacto que pueda tener la sepsis neonatal en la ocurrencia de trastornos del neurodesarrollo en los recién nacidos de muy bajo peso egresados de las unidades de cuidados intensivos neonatales en Cuba, país subdesarrollado que ha logrado bajas tasas de mortalidad infantil.
El Hospital Gineco-obstétrico Docente Provincial de Matanzas Dr. Julio Alfonso Medina, se encuentra ubicado en la ciudad cabecera de la provincia del mismo nombre. Constituye el centro de referencia en esta provincia para la atención a los recién nacidos con peso al nacer <1500 gramos. En él radica una consulta provincial de seguimiento del neurodesarrollo, donde los recién nacidos con riesgo de secuelas neurológicas son evaluados durante los primeros años de vida con una metodología descrita en otros trabajos [19].
A partir de la hipótesis de que la sepsis neonatal parece constituir un factor de riesgo asociado a peor evolución del neurodesarrollo en recién nacidos de muy bajo peso, se realizó este estudio cuyo objetivo principal fue determinar el impacto de la sepsis neonatal como factor de riesgo en la ocurrencia de alteraciones del neurodesarrollo en recién nacidos de muy bajo peso egresados vivos de un centro de tercer nivel de atención perinatal en Cuba.
Métodos
Se realizó un estudio observacional prospectivo con 89 neonatos con peso al nacer <1500 gramos, nacidos durante el periodo 2006-2010 en la Provincia de Matanzas y egresados vivos del Servicio de Neonatología del Hospital Gineco-obstétrico Docente Provincial de Matanzas Dr. Julio Alfonso Medina. Estos recién nacidos tenían una edad gestacional al nacer menor de 37 semanas (según fecha de la última menstruación o en su defecto, por ultrasonografía realizada al inicio del embarazo o puntaje de Ballard modificado), y cumplieron su seguimiento en la consulta de neurodesarrollo de dicho centro hasta los 24 meses de edad corregida (edad en meses a partir del momento en que se cumplieran las 40 semanas de edad gestacional).
Fueron excluidos del estudio los neonatos con malformaciones mayores o síndromes genéticos reconocidos al momento del nacimiento, así como las muertes neonatales y posneonatales.
La muestra de estudio estuvo constituida por 89 recién nacidos de muy bajo peso. La misma se conformó a partir de un total de 134 recién nacidos vivos con peso al nacer <1500 gramos, nacidos en la provincia de Matanzas en el período de años 2006-2010. De ellos, 99 nacieron en el Hospital Gineco-obstétrico Docente Provincial de Matanzas Dr. Julio Alfonso Medina. El resto fue trasladado durante el período neonatal a dicho centro, provenientes de otros hospitales de la provincia. De los 134 nacidos vivos con peso <1500 gramos, hubo 26 que resultaron en defunciones neonatales; por lo que el total de egresados vivos fue de 108. Cuatro de ellos se excluyeron del estudio por presentar malformaciones, síndromes genéticos y muertes posneonatales, y 104 entraron en el programa de seguimiento. De estos últimos, hubo 89 que completaron su seguimiento hasta los dos años de edad corregida, que son los que constituyen la muestra de estudio.
Grupos de estudio
Con los 89 pacientes que reunieron los criterios para entrar en el estudio se conformaron dos grupos: un grupo con sepsis (expuestos), integrado por los pacientes que hubieran presentado sepsis clínica durante el período neonatal (en total 19), y un segundo grupo denominado grupo sin sepsis (no expuestos), conformado por los pacientes que no hubieran presentado sepsis durante el periodo neonatal (en total 70).
Para el diagnóstico de sepsis neonatal se tuvo en cuenta los criterios de Haque KN [20], los cuales incluyen variables clínicas, hemodinámicas, de perfusión tisular e inflamatorias, con la excepción de que en estas últimas no se consideraron los valores de proteína C reactiva, procalcitonina, ni interleukinas 6 u 8, por no realizarse de manera habitual en el centro donde se realizó el estudio. Cuando hubo crecimiento de gérmenes en los hemocultivos realizados, se consideró sepsis probada. Cuando estos no se realizaron o resultaron negativos, se consideró sepsis no probada. En el estudio se incluyeron tanto los pacientes con sepsis neonatal probada como no probada.
Además de las variables inflamatorias contenidas en los criterios de Haque KN (leucocitosis>34 000x109/l, leucopenia<5000x109/l, neutrófilos inmaduros>10%, relación inmaduros/neutrófilos totales>0,2 y trombocitopenia <100 000x109/l), hubo otros parámetros hematológicos contenidos en los criterios de Rodwell et al. [21] que se tuvieron en cuenta en este estudio al incluir los pacientes en el grupo con sepsis. Estos fueron la presencia de leucocitosis (≥25 000x109/l al nacimiento, o ≥30 000x109/l entre las 12 y 24 horas de vida, o ≥21 000x109/l más allá de las 48 horas de vida), neutrofilia o neutropenia, índice de neutrófilos aumentado, relación inmaduros/segmentados ≥0,3 y presencia de neutrófilos con granulaciones tóxicas o vacuolización.
Dentro del grupo con sepsis neonatal no solo se incluyeron los pacientes con sepsis neonatal no localizada, sino también aquellos neonatos que presentaron una infección localizada a la cual se agregaban dos o más signos de respuesta inflamatoria sistémica, de los establecidos por consenso internacional como criterios de síndrome de respuesta inflamatoria sistémica en el neonato. Estos signos son la presencia de alteraciones en la frecuencia cardíaca (>180 o <100 latidos por minuto), alteraciones de la frecuencia respiratoria (>50 respiraciones por minuto en el neonato durante la primera semana de vida o >40 por minuto de ocho a 30 días de nacido), alteraciones de la temperatura (<36 o >38,5 °C), alteraciones en el recuento total de leucocitos (>34 000 en la primera semana de vida o >19 500 o <5000 entre los ocho y 30 días de nacido), y la presencia de células en banda (>10% del conteo total de leucocitos) [22].
Etapas de la investigación
Esta investigación constó de tres etapas:
- 1° etapa: se realizó un estudio de cohorte, con el objetivo de determinar la asociación de la sepsis neonatal con las alteraciones del neurodesarrollo.
- 2° etapa: mediante un análisis de regresión logística, se determinó si la sepsis neonatal se asociaba a la ocurrencia de alteraciones del neurodesarrollo al considerar otras variables que potencialmente podían constituir factores de riesgo de alteraciones del neurodesarrollo. Estas variables fueron seleccionadas previamente, a partir de un análisis bivariado de riesgo.
- 3° etapa: se analizó si existía asociación entre el momento de aparición de la sepsis y la presentación de alteraciones del neurodesarrollo, así como si existía una asociación de “dosis-respuesta” entre los niveles de exposición a episodios de sepsis neonatal y la ocurrencia de alteraciones del neurodesarrollo.
Variables estudiadas
Se consideró como alteración del neurodesarrollo cualquier desviación del neurodesarrollo normal durante los primeros 24 meses de edad corregida, demostrable por examen neurológico, test de Bayley II [23] o pruebas neurofisiológicas.
En la clasificación de la evolución del neurodesarrollo durante los dos primeros años de edad corregida se emplearon, además, otras categorías:
- Alteraciones mayores. Presencia de una o más de las siguientes alteraciones: parálisis cerebral moderada-severa, índice de desarrollo psicomotor o índice de desarrollo mental <70, sordera bilateral o ceguera bilateral, epilepsia, hidrocefalia o microcefalia.
- Alteraciones menores. Presencia de una o más de las siguientes alteraciones: hipotonía muscular leve o transitoria, insuficiencia motora ligera con tono aumentado, alteraciones reflejas ligeras o transitorias, retardo transitorio o leve del desarrollo psicomotor (índice de desarrollo psicomotor 70-84), retardo mental ligero (índice de desarrollo mental 70-84), retardo ligero del lenguaje, hiperactividad, alteración neurosensorial ligera o unilateral.
- Normal. Cuando no se presentó ninguna de las alteraciones anteriores.
Se consideró parálisis cerebral la presencia de un trastorno permanente o crónico de la función motora, de origen en el cerebro o cerebelo, de aparición temprana en la vida, no debido a enfermedad progresiva reconocida y con un límite mínimo de dos años de edad postnatal al momento de la evaluación [24]. La discapacidad visual severa y bilateral se definió como la imposibilidad para la visión útil en ambos ojos. En tanto, la ceguera ligera o unilateral se determinó como la disminución de la agudeza visual en uno o ambos ojos, pero que no imposibilitara totalmente la función de la visión. Se consideró sordera bilateral severa cuando existía imposibilidad para la audición en ambos oídos y el paciente requería de amplificación para poder oír, e hipoacusia unilateral ligera, cuando había imposibilidad para la audición en un solo oído, o la disminución de la capacidad auditiva no requería de equipo de amplificación para lograr la función auditiva.
Las variables independientes incluidas en el análisis bivariado de riesgo fueron sexo masculino (versus femenino), peso al nacer (gramos), edad gestacional (según fecha de la última menstruación, o en su defecto por ultrasonido obstétrico, o examen físico neonatal por método de Ballard modificado), bajo peso para la edad gestacional (peso para la edad gestacional al nacer por debajo del décimo percentil según las curvas de Dueñas E et al. [25]), Apgar bajo al minuto y a los cinco minutos de nacido (puntuación 0-6), tipo de parto (transpelviano versus cesárea), enfermedad de membrana hialina, displasia broncopulmonar (considerada presente cuando, al menos, a los 28 días de nacido el paciente requería aún terapia con oxígeno) [26], hiperbilirrubinemia no fisiológica (presencia de valores de bilirrubina sérica ≥15 mg/dl), uso de esteroides antenatales (uno o más ciclos de tratamiento completo), uso de surfactante exógeno (uno o más dosis de tratamiento) y empleo de asistencia respiratoria mecánica (ya fuera ventilación mecánica convencional o de alta frecuencia).
Las sepsis neonatales fueron clasificadas, de acuerdo al comienzo de sus síntomas y signos, en precoces (aparición en las primeras 72 horas de nacido), tardías (aparición más allá de las 72 horas de nacido) y precoces con reinfección tardía (cuando una sepsis apareció en las primeras 72 horas de vida y luego se produjo otra sepsis, pasado ese lapso).
En el análisis final, correspondiente al nivel de exposición a la sepsis y su asociación con la presentación de alteraciones del neurodesarrollo, la variable episodios de sepsis neonatal se dividió en tres categorías: sin sepsis, un episodio de sepsis y más de un episodio de sepsis (con independencia del momento de aparición de la misma).
Seguimiento
A todos los recién nacidos de muy bajo peso se les realizó un examen neurológico al término (al cumplir 38 a 42 semanas de edad gestacional corregida), mediante los métodos de Amiel Tison et al., Prechtl y Fenichel, [14],[19]. En ese momento fueron clasificados en una de las siguientes categorías:
- Normales: examen neurológico sin alteraciones.
- Sospechosos: presencia de hipotonía de eje, alteración de los reflejos primarios y osteotendinosos, así como de su capacidad adaptativa.
- Patológicos: presencia de hipotonía global (de eje y miembros) o hipertonía de eje y/o de miembros, disminución o aumento marcado de los reflejos integrados y osteotendinosos, y pobre capacidad adaptativa.
Todos los pacientes fueron examinados durante el primer año de edad corregida con controles al primero, segundo, tercero, sexto, noveno y duodécimo mes, y durante el segundo año con frecuencia trimestral. A cada uno se le realizó la valoración neurológica por el método de Amiel-Tison [14],[19] durante el primer año. Durante el segundo año se aplicó examen neurológico clásico.
La valoración del desarrollo psicomotor y mental se efectuó mediante la escala de Bayley II [23], la cual se aplicó al final del primero y del segundo año de edad corregida. El seguimiento clínico se completó con la realización de ultrasonografía cerebral transfontanelar al mes, al final del tercero y del sexto mes de edad corregida; así como de potenciales evocados auditivos y de tallo cerebral.
Recogida de la información
Los datos referentes a la evolución del paciente durante el período perinatal, fueron obtenidos de las historias clínicas maternas y neonatales. Esta información y la obtenida durante el seguimiento del neurodesarrollo fueron recogidas en un modelo de elaboración propia donde se resumió la información necesaria de cada paciente.
Procesamiento estadístico
Con toda la información anterior se conformó una base de datos para lo cual se empleó el paquete estadístico SPSS versión 17.0, con el que se realizaron los cálculos estadísticos necesarios.
Para lograr el objetivo de la primera etapa de este trabajo, se empleó como medida fundamental el riesgo relativo (RR) y sus intervalos de confianza al 95% (IC 95%). De forma similar, se halló la asociación entre la sepsis neonatal y la presencia de alteraciones específicas del neurodesarrollo.
En la segunda etapa del estudio, para seleccionar las variables candidatas a ser incluidas posteriormente en el modelo de regresión logística, se emplearon como medidas de resumen de las variables cuantitativas continuas la media y la desviación estándar. Para las variables cualitativas se usaron las frecuencias absolutas y relativas. En el análisis bivariado se empleó, para variables cualitativas nominales, la prueba chi cuadrado o el test exacto de Fisher, este último cuando las frecuencias esperadas fueron menores de cinco o si resultaban igual a cero. Cuando se trataba de variables cuantitativas, se empleó la prueba de t para la comparación de medias entre dos poblaciones. En todos los casos se consideró significativo todo valor de p<0,05.
Posteriormente se realizó un análisis de regresión logística en el que, mediante la técnica del ómnibus, se calcularon los odds ratio (OR) y sus intervalos de confianza al 95%. Se consideró como significativo todo valor de p<0,05.
Previo al análisis de regresión logística se realizó un análisis de colinealidad entre las covariables independientes candidatas a ser incluidas en el mismo, para el que se utilizó el coeficiente de correlación de Pearson. Las covariables incluidas en el análisis de regresión logística se seleccionaron sobre la base de que no existiera alta correlación entre las mismas. De esta forma, cuando el coeficiente de Pearson arrojó que existía una alta correlación (>0,5) entre dos o más de las posibles covariables independientes, solo se seleccionó una, teniendo en cuenta la de mayor importancia de acuerdo a la literatura revisada y a los objetivos del estudio. Fue así que se seleccionó la variable asistencia respiratoria mecánica y se excluyó del análisis la enfermedad de membrana hialina y el empleo de surfactante, por tener cada una de estas dos últimas una alta correlación con la primera.
De esta manera, en el modelo de regresión logística se incluyeron las cuatro covariables resultantes de la selección anterior: sepsis neonatal, asistencia respiratoria mecánica, hiperbilirrubinemia no fisiológica y displasia broncopulmonar; además de incluir el sexo masculino. Como variable dependiente, se incluyó en el modelo la presencia de alteraciones del neurodesarrollo.
Para determinar la asociación entre el momento de aparición de la sepsis y la presentación de alteraciones del neurodesarrollo, se incluyeron en el modelo las categorías sepsis neonatal precoz, sepsis neonatal tardía y sepsis neonatal precoz con reinfección tardía, las cuales fueron tratadas como variables internas o “dummy”.
Finalmente, para determinar la posible asociación de dosis-respuesta de los episodios de sepsis neonatal con la ocurrencia de alteraciones del neurodesarrollo, se hallaron los riesgos relativos e intervalos de confianza al 95%.
Aspectos éticos
La inserción de los pacientes en el seguimiento se realizó bajo el consentimiento informado de los padres o tutores, quienes tuvieron la libertad de abandonar el mismo en el momento en que lo desearan. La investigación contó con la aprobación del consejo científico y el comité de ética en las investigaciones del centro donde se ejecutó.
Resultados
En la Tabla 1 se presentan las características generales de los 89 recién nacidos de muy bajo peso incluidos en este estudio, en los que hubo un predominio del sexo femenino. El peso promedio al nacer fue de 1278 gramos (mínimo 700 y máximo 1490 gramos) y la edad gestacional promedio fue de 31,4 semanas (mínima 26 y máxima 36 semanas). Los neonatos con peso <1000 gramos constituyeron alrededor del 8%. La mayoría de los recién nacidos presentaron una puntuación de Apgar normal y alrededor del 40% recibió alguna modalidad de asistencia respiratoria mecánica. La sepsis neonatal se presentó en 21,3% de los neonatos estudiados.
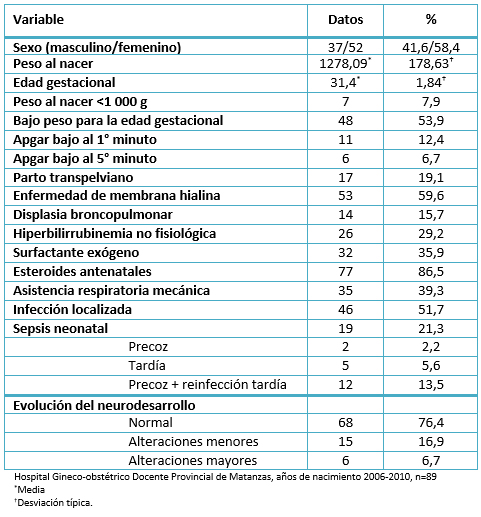
Tabla 1: Características generales de los recién nacidos de muy bajo peso incluidos en el estudio.
Al analizar la asociación de la sepsis neonatal con la ocurrencia de alteraciones del neurodesarrollo en los primeros dos años de edad corregida, se obtuvo que los recién nacidos de muy bajo peso que presentaron sepsis neonatal tuvieron un riesgo mayor de presentar alteraciones del neurodesarrollo que los que no presentaron sepsis (47,4 versus 17,1%; RR 2,7 IC 95%: 1,3-5,5; p=0,005).
En la Tabla 2 se muestran con mayor detalle los resultados del neurodesarrollo en los recién nacidos estudiados, según hubieran presentado o no sepsis durante el período neonatal. De acuerdo a este análisis, la sepsis neonatal se asoció a un mayor riesgo de alteraciones mayores del neurodesarrollo, aunque esta asociación no fue significativa. En tanto que la asociación de la sepsis neonatal con un riesgo incrementado de alteraciones menores del neurodesarrollo, sí resultó significativa.
En la misma Tabla 2 se muestran la frecuencia y el riesgo de presentación de las alteraciones específicas del neurodesarrollo en los pacientes estudiados. Los pacientes con sepsis neonatal presentaron un incremento en el riesgo de parálisis cerebral, de retardo en el desarrollo psicomotor moderado/severo (índice de desarrollo psicomotor <70) y de retardo en el desarrollo mental (índice de desarrollo mental <70), pero estas asociaciones no resultaron estadísticamente significativas. De las alteraciones menores, es de destacar que la sepsis neonatal se asoció significativamente a un mayor riesgo de hipotonía leve o transitoria y de retardo leve o transitorio en el desarrollo psicomotor, mientras que no se asoció significativamente a la presencia de discapacidad visual ligera o unilateral.
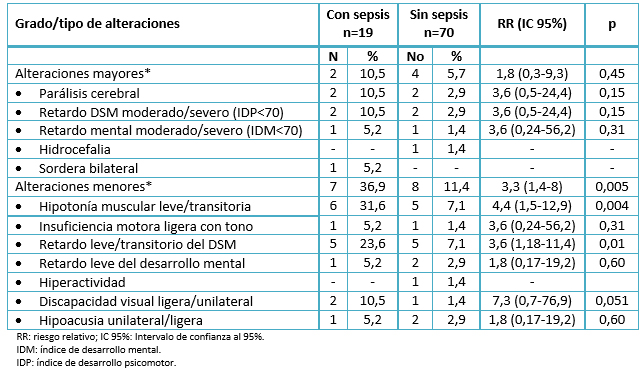 *Un mismo paciente pudo presentar más de una alteración.
*Un mismo paciente pudo presentar más de una alteración.
Tabla 2: Alteraciones del neurodesarrollo durante los primeros dos años de edad corregida encontradas en los recién nacidos estudiados (N=89).
En la Tabla 3 aparecen los resultados del análisis bivariado de riesgo, en el que se determinó la asociación de una serie de variables con la presencia de sepsis neonatal. De las variables analizadas, solamente tuvieron una asociación estadísticamente significativa con la presencia de sepsis neonatal la presencia de enfermedad de membrana hialina, displasia broncopulmonar, hiperbilirrubinemia no fisiológica, el uso de surfactante exógeno y el empleo de asistencia respiratoria mecánica.
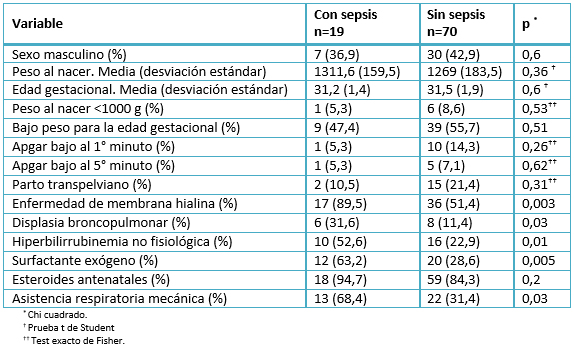
Tabla 3: Asociación de las variables estudiadas con la presencia de sepsis neonatal, según análisis bivariado (n=89).
En la Tabla 4 se muestran los resultados del modelo de regresión logística realizado con vista a determinar la fuerza de asociación independiente de las covariables incluidas en el mismo con respecto a la presencia de alteraciones del neurodesarrollo. Según este análisis, la única variable que resultó significativa fue la sepsis neonatal, la cual se asoció a un incremento de cuatro veces en el riesgo de alteraciones del neurodesarrollo. La asistencia respiratoria mecánica en el período neonatal y la displasia broncopulmonar se asociaron a un incremento en el riesgo de alteraciones del neurodesarrollo, al igual que el sexo masculino, pero estas asociaciones no fueron significativas.
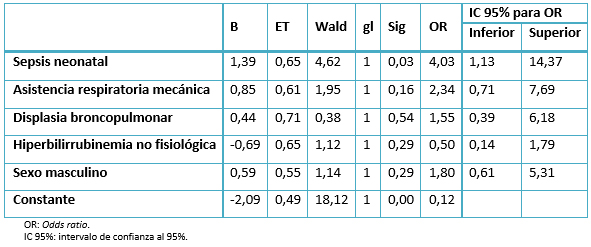
Tabla 4: Asociación de la sepsis neonatal con la presencia de alteraciones del neurodesarrollo según análisis de regresión logística (n=89; casos=21, controles=68).
Al realizar el análisis de riesgo anterior, pero esta vez incluyendo en el mismo en vez de la covariable sepsis neonatal el tipo de sepsis neonatal de acuerdo a su momento de aparición, se obtuvo que la sepsis neonatal precoz con reinfección tardía se asoció a un incremento significativo en el riesgo de alteraciones del neurodesarrollo (odds ratio 4,5 IC 95%: 1,02-20,3), mientras que la sepsis neonatal tardía se asoció a un incremento en el riesgo, pero no significativo (odds ratio 7,5 IC 95%: 0,82-69,5). La sepsis neonatal precoz, cuando se presentó sola, no se asoció a alteraciones del neurodesarrollo.
Finalmente, se analizó la asociación del número de exposiciones a episodios de sepsis con la ocurrencia de alteraciones del neurodesarrollo. El resultado fue que a medida que aumentó el número de exposiciones, se produjo un incremento en el riesgo de alteraciones del neurodesarrollo, lo que fue significativo cuando hubo más de una exposición a episodios de sepsis, tal como se muestra en la Figura 1.
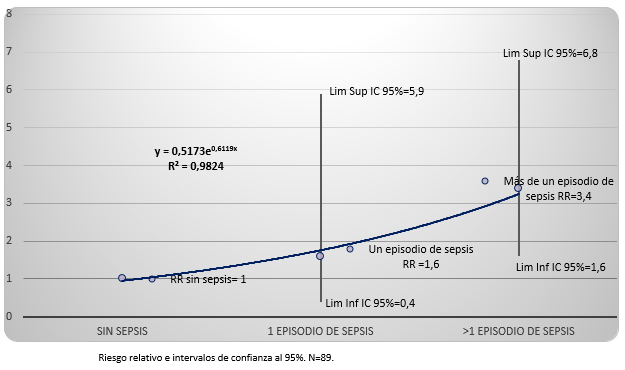
Figura 1.: Riesgo de alteraciones del neurodesarrollo según número de episodios de sepsis neonatal.
Discusión
Características de la población estudiada
Del total de recién nacidos de muy bajo peso incluidos en este estudio, 23,6% presentó alteraciones durante su neurodesarrollo en los primeros dos años de edad corregida, resultado muy similar al encontrado por Moll et al. en Alemania [27], pero que difiere de los obtenidos en otros estudios. En dos de ellos [5],[28], el porcentaje de alteraciones del neurodesarrollo fue inferior al encontrado aquí, con 10,1 y 17%, respectivamente; mientras que en el otro [16], fue superior con 38% de secuelas.
El porcentaje de alteraciones mayores en el actual estudio se encuentra en el rango reportado en otros trabajos realizados en Cuba (entre 5,2 y 11,1%) [14],[15],[16]; no obstante, es inferior al encontrado por otros autores foráneos (entre 19 y 25%) [29],[30].
Si se comparan algunas de las características de la población incluida en este trabajo (Tabla 1) con la de un estudio multicéntrico realizado en España [5], es de destacar que en el actual estudio el porcentaje de recién nacidos con peso <1000 gramos fue menor, al igual que la frecuencia de puntuaciones de Apgar <7 al quinto minuto de nacido y la de empleo de surfactante exógeno; mientras que las frecuencias de uso de esteroides antenatales y de displasia broncopulmonar fueron mayores. Con relación a otros estudios realizados en Gran Bretaña y Suiza, en el actual la frecuencia de presentación de infecciones fue mayor [31],[32].
Incidencia de sepsis neonatal en recién nacidos de muy bajo peso
La incidencia global de sepsis neonatal en países desarrollados se encuentra entre uno y 12 por cada 1000 nacidos vivos, aunque en los países subdesarrollados llega a ser tan alta como entre 20 y 30% de todos los nacidos vivos. El riesgo de secuelas del neurodesarrollo es mayor en los recién nacidos con sepsis, pero si se trata de recién nacidos de muy bajo peso este riesgo es mayor [33].
La tasa de incidencia peso específica de sepsis neonatal en recién nacidos vivos con peso <1500 gramos durante el período estudiado en el hospital donde se llevó a cabo esta investigación, era de 33% (datos obtenidos del Departamento de Registros Médicos y del Registro de Morbilidad del Servicio de Neonatología del Hospital Gineco-obstétrico Docente Provincial de Matanzas Dr. Julio Alfonso Medina). Si se compara esta cifra con respecto a la incidencia reportada de sepsis neonatal en los recién nacidos de muy bajo peso en estudios realizados en países desarrollados [32],[34],[35], donde la sepsis neonatal se encuentra entre 9,8 y 31,7% de todos los recién nacidos con peso <1500 gramos, es obvio que la incidencia en este centro resulta algo más elevada.
La incidencia de sepsis neonatal en este trabajo se refiere tanto a las sepsis no probadas como probadas. Ello pudo influir en que en el mismo la sepsis de aparición temprana tuviera una mayor incidencia que la de aparición tardía, contrario a lo que refieren la mayoría de los trabajos. Un estudio realizado en Australia muestra cómo, al considerar las sepsis no probadas o clínicas, la frecuencia de la sepsis de aparición temprana es mayor que la tardía (32 versus 26,6%); en tanto que cuando se consideran solamente las sepsis probadas, sucede lo contrario (1,3 versus 17,4%) [35].
Sepsis neonatal y alteraciones del neurodesarrollo
La asociación de la sepsis neonatal con mayor riesgo de alteraciones del neurodesarrollo, ha sido encontrada en múltiples estudios en recién nacidos de muy bajo peso o con edad gestacional <34 semanas, con peso <1000 gramos o edad gestacional <28 semanas [12],[31],[33],[36],[37],[38]. La mayoría de tales estudios han sido llevados a cabo en países de altos o medianos ingresos. El riesgo de alteraciones del neurodesarrollo a los dos años de edad corregida en recién nacidos de muy bajo peso y de bajo peso extremo con sepsis neonatal, es alrededor de dos a tres veces mayor que en los neonatos de igual grupo de peso sin sepsis neonatal (odds ratio 2,09; IC 95%:1,65-2,65) [12],[13]. En el actual estudio, el riesgo relativo de presentar alteraciones del neurodesarrollo en los primeros dos años de edad corregida en los recién nacidos de muy bajo peso con sepsis neonatal, comparado con los que no tuvieron sepsis, estuvo en el rango de lo reportado por tales autores [12],[13],[33].
La sepsis con o sin meningitis se asocia a un incremento de dos a 10 veces en el riesgo de parálisis cerebral [12],[33],[39], lo cual ha sido demostrado también en estudios realizados en Cuba [40],[41].
El resultado neurológico adverso asociado a la sepsis en sobrevivientes neonatales nacidos con muy bajo peso, se ha constatado no solo en relación a la ocurrencia de parálisis cerebral y otros trastornos neuromotores, sino también en relación a la ocurrencia de trastornos del desarrollo intelectual (retraso mental o daño cognitivo) [12],[37], aunque los resultados en cuanto a este último grupo de trastornos son controvertidos [9],[36],[38].
En el estudio del National Institute of Child Health and Human Development Neonatal Research Network, de Estados Unidos, los recién nacidos de muy bajo peso con infecciones tuvieron un mayor riesgo de tener microcefalia, parálisis cerebral, índice de desarrollo psicomotor e índice de desarrollo mental <70 y daño visual [11]. Estos hallazgos han sido corroborados en un metanálisis reciente [33], que muestra que los recién nacidos de muy bajo peso y con edad gestacional <34 semanas que presentan sepsis neonatal tienen un mayor riesgo de parálisis cerebral (RR 2; IC 95%: 1,7-2,3), daño cognitivo (RR 1,6; IC 95%: 1,4-1,8), retardo en el desarrollo psicomotor (RR 1,9; IC 95%: 1,5-2,3), daño visual (RR 2,2; IC 95%: 1,6-3,2) y daño auditivo (RR 3,2; IC 95%: 2,3-4,4).
En otro metanálisis se ha encontrado una disminución equivalente a 3,75 y 5,55 puntos en los índices de desarrollo mental y de desarrollo psicomotor respectivamente, en recién nacidos de muy bajo peso o pretérmino con infecciones perinatales, al ser comparados con niños de este mismo grupo de peso y edad gestacional, pero que no tuvieron infecciones de este tipo [9]. Las infecciones neonatales (sepsis, enterocolitis necrotizante y meningitis), analizadas en conjunto, agregan un riesgo adicional al que se produce en niños de bajo peso extremo con tres morbilidades como la displasia broncopulmonar, el daño cerebral y la retinopatía de la prematuridad, con respecto a sus resultados adversos (muerte o secuelas neurológicas) en los primeros 18 meses de edad corregida [10].
En el presente estudio, el mayor riesgo de alteraciones del neurodesarrollo en pacientes con sepsis neonatal resultó estadísticamente significativo solamente para las alteraciones del neurodesarrollo en su conjunto y para las alteraciones menores, pero no para las alteraciones mayores. Este resultado podría explicarse por la baja potencia del estudio cuando se analizaron fenómenos de baja frecuencia, si se tiene en cuenta que la muestra es pequeña, comparada con la de otros estudios colaborativos multicéntricos o metanálisis [5],[9],[13],[29],[33].
Otra explicación probable para este hallazgo pudiera estar relacionada con la etiopatogenia del daño cerebral en el recién nacido pretérmino. Desde hace algunos años se ha planteado la hipótesis de múltiples hits en la ocurrencia de daño cerebral, especialmente en los neonatos pretérmino [3]. La sepsis neonatal actúa como uno de los últimos eslabones en la cadena de eventos causales de alteraciones del neurodesarrollo. Por esta razón su efecto, en el caso de las alteraciones mayores, podría verse como el de un factor agravante a partir de un daño pre-establecido antenatalmente. Esos factores antenatales no han sido analizados en este estudio, pero se ha demostrado que tienen una contribución mayor en la ocurrencia de parálisis cerebral y otras alteraciones mayores del neurodesarrollo [42],[43]. Sin embargo, en el caso de las alteraciones menores, el efecto de la sepsis neonatal pudiera ser considerado como más cercano dentro de la cadena de eventos que pueden dar lugar a estas alteraciones, lo cual pudiera implicar que la asociación fuera más fácil de demostrar estadísticamente.
De cualquier manera, los resultados de este estudio demuestran que la sepsis per se constituye un factor de riesgo perinatal en la ocurrencia de alteraciones del neurodesarrollo en recién nacidos de muy bajo peso, lo cual corrobora los resultados de otros estudios [12],[13],[33],[36],[37],[38]. Los episodios de sepsis en los recién nacidos pretérmino se asocian a leucomalacia periventricular, la que resulta en alteraciones neurológicas entre los 12 y 14 meses de edad en cerca del 90% de estos niños [39].
Tipo de sepsis y alteraciones del neurodesarrollo
En el actual estudio la sepsis de aparición precoz con reinfección tardía se asoció a un riesgo incrementado de alteraciones del neurodesarrollo, lo cual coincide con los resultados de Mitha et al. en un estudio realizado en Francia [44]. Se ha encontrado también asociación significativa de la sepsis de aparición tardía con un incremento en el riesgo de secuelas neurológicas [12],[38],[44], lo cual pudo ser constatado en este estudio, aunque no en forma significativa. No obstante la asociación del tipo de sepsis, de acuerdo a su momento de aparición, con la presencia de alteraciones del neurodesarrollo en recién nacidos de muy bajo peso resulta aún controvertida [5].
La asociación entre la infección por determinados agentes etiológicos y la ocurrencia de secuelas del neurodesarrollo ha sido estudiada también. Esta asociación ha sido significativa para la sepsis de aparición tardía por bacterias gram positivas [38], así como para las infecciones sistémicas por hongos [45].
Pero en este estudio tal asociación no fue evaluada. Aunque sí se estudió la asociación entre el número de exposiciones a episodios de sepsis y los resultados del neurodesarrollo en recién nacidos de muy bajo peso (Figura 1), encontrándose una relación dosis-dependiente entre la aparición de secuelas neurológicas y la exposición creciente a episodios de sepsis, independientemente del momento de aparición de la sepsis. Este es un hallazgo importante, que concuerda con el de Glass et al., en que la exposición a múltiples episodios de infección probada incrementa el riesgo de daño progresivo a la sustancia blanca [46].
La principal fortaleza de este trabajo es que aporta evidencias epidemiológicas, sobre la base del tiempo, para demostrar la probable relación causal entre la sepsis neonatal y las alteraciones del neurodesarrollo en recién nacidos de muy bajo peso. Además, este aporte tiene lugar en el contexto de un país subdesarrollado. Pero se necesita acumular más evidencia experimental a partir de intervenciones en salud pública, para demostrar esta relación, ya que la muestra en el actual estudio fue pequeña. Ello constituye una limitación a la hora de extrapolar sus resultados, particularmente en los eventos con muy baja frecuencia de presentación.
Conclusiones
La fuerza de asociación de la sepsis neonatal con los resultados adversos del neurodesarrollo en recién nacidos de muy bajo peso, fue similar en este estudio en relación a otros realizados en países de mayor desarrollo económico. La sepsis neonatal debe considerarse como una causa importante, dentro de los múltiples eventos causales de daño cerebral en el recién nacido pretérmino.
Es posible que se pueda disminuir la incidencia de secuelas del neurodesarrollo en recién nacidos de muy bajo peso con la implementación de medidas de intervención más efectivas dirigidas a la prevención de la sepsis neonatal.
Notas
Aspectos éticos
La inserción de los pacientes en el seguimiento se realizó bajo el consentimiento informado de los padres o tutores, quienes tuvieron la libertad de abandonar el mismo en el momento en que lo desearan. La investigación contó con la aprobación del Consejo científico y el Comité de ética en las investigaciones del centro donde se ejecutó.
Declaración de conflictos de intereses
Los autores han completado el formulario de declaración de conflictos intereses del ICMJE traducido al castellano por Medwave, y declaran no haber recibido financiamiento para la realización del reporte; no tener relaciones financieras con organizaciones que podrían tener intereses en el artículo publicado, en los últimos tres años; y no tener otras relaciones o actividades que podrían influir sobre el artículo publicado. Los formularios pueden ser solicitados contactando al autor responsable o a la dirección editorial de la Revista.
Financiamiento
Los autores declaran que no hubo fuentes de financiación externas.

