Estudios originales
← vista completaPublicado el 17 de noviembre de 2020 | http://doi.org/10.5867/medwave.2020.10.8066
Pronóstico de pacientes hospitalizados por COVID-19 en un centro terciario en Chile: estudio de cohorte
Prognosis of patients with COVID-19 admitted to a tertiary center in Chile: A cohort study
Resumen
Introducción Desde el comienzo de la pandemia de COVID-19, se han desarrollado diversas investigaciones sobre el pronóstico de pacientes con SARS-CoV-2 asociado a factores como edad, condiciones biodemográficas, comorbilidades, factores sociales, parámetros clínicos, hematológicos, marcadores inflamatorios, de coagulación, bioquímicos y gasométricos, entre otros. Hasta ahora, existen escasos estudios que hayan abordado el tema en América Latina, por lo que es de interés conocer el comportamiento de la enfermedad en la región.
Objetivo Evaluar el curso del COVID-19 en pacientes ingresados en un centro terciario en Chile y analizar factores predictores, medidos en el período cercano a la admisión, que se asocien al pronóstico vital y al uso de ventilación mecánica invasiva.
Métodos Estudio de cohorte retrospectivo realizado en Clínica Indisa de Santiago, Chile. Participaron todos los pacientes de 15 años o más hospitalizados entre el 11 de marzo y el 25 de julio de 2020. Se analizó la letalidad hospitalaria, la complejidad de los casos y se aplicaron modelos de regresión logística para identificar predictores de las variables de resultado definidas.
Resultados La muestra estuvo constituida por 785 sujetos. La edad media fue 59 años, 59% fueron hombres y 61,3% tenía comorbilidades. El 45% requirió cuidados intensivos y 24% ventilación mecánica invasiva. La letalidad hospitalaria global fue de 18,7%. En pacientes de unidad de cuidados intensivos fue 32,1% y en quienes recibieron ventilación mecánica invasiva 59,4%. Los factores de riesgo independientes de morir incluyeron la edad (Odds ratio 1,09; intervalo de confianza 95%: 1,07 a 1,12), diabetes (1,68; 1,06 a 2,67), enfermedad pulmonar crónica (2,80; 1,48 a 5,28) y mayores niveles de proteína C reactiva, creatinina y ferritina. No se demostró asociación con el sexo, pertenencia al seguro público de salud, antecedente de cardiopatía, obesidad, ni dímero D. Similares factores fueron predictores de ventilación mecánica invasiva.
Conclusiones El pronóstico y factores predictores en esta cohorte de pacientes hospitalizados en Chile por COVID-19 fueron comparables en su mayoría a los reportados en estudios similares de países de mayores ingresos. El sexo masculino no fue un factor de mal pronóstico en este grupo de pacientes.
Ideas clave
- Existe escasa literatura que aborde la letalidad y factores pronósticos del COVID-19 en el contexto latinoamericano. No se han publicado investigaciones similares en Chile.
- El estudio analiza estos aspectos en una cohorte retrospectiva de 785 pacientes hospitalizados en un centro terciario en Chile, con énfasis en la identificación de factores predictores de muerte y necesidad de ventilación mecánica medidos en el momento de admisión.
- Los resultados son similares a los reportados en países desarrollados, pero representan preferentemente a pacientes que se atienden en el sector privado de salud, por lo que no necesariamente son extrapolables a la población general.
- Además, el carácter retrospectivo del estudio limita la calidad de los datos y la posibilidad de haber estudiado más a fondo algunas comorbilidades.
Introducción
Desde las primeras cohortes estudiadas en China[1],[2], la investigación sobre el pronóstico del COVID-19 y los factores que la afectan se fue extendiendo a otros países afectados por la pandemia[3],[4],[5]. Los resultados de estas cohortes comenzaron a ser consolidados en revisiones sistemáticas, inicialmente con un enfoque amplio[6],[7], y pronto orientadas a factores específicos[8],[9]. A partir de allí se han propuesto nuevos índices pronósticos[10] y modelos predictivos[11],[12]. Algunos se han aventurado en complejas investigaciones que implican el análisis de decenas de componentes metabólicos e inmunológicos que podrían tener correlación con la severidad de la enfermedad[13]. Pese a todo, el panorama sobre la importancia y aplicabilidad clínica de estas variables dista de ser concluyente. Además, existe una amplia heterogeneidad en la literatura en cuanto a los métodos de análisis, criterios de medición, y en la significación y magnitud de las asociaciones encontradas. A esto se agrega la dudosa calidad de algunas de las revisiones publicadas[14],[15].
Por su parte, el médico que enfrenta a un paciente con COVID-19 espera disponer de información simple y confiable sobre los factores que pueden servir de alerta temprana, para anticipar el curso de la enfermedad, por ejemplo, respecto de la necesidad de ventilación mecánica invasiva. Lo mismo aplica a los factores que sirven para controlar la evolución de los casos graves y monitorear las complicaciones que vaya presentando el paciente, para adoptar en forma oportuna medidas acordes.
Entre los múltiples factores estudiados, sobre los cuales existe alguna evidencia de asociación con el pronóstico de los pacientes, se incluyen condiciones biodemográficas, comorbilidades, factores sociales, parámetros clínicos, hematológicos, marcadores inflamatorios, de coagulación, bioquímicos y gasométricos, entre otros. De los mencionados, el que claramente resulta más consistente y con asociaciones de mayor magnitud es la edad.
Si bien la evidencia acumulada es posiblemente generalizable, hasta ahora existen escasos estudios que hayan abordado el tema en América Latina[16],[17],[18], por lo que es de interés conocer el comportamiento de la enfermedad en la región. El presente estudio tiene por objetivo evaluar el curso del COVID-19 en pacientes ingresados en un centro terciario en Chile y analizar factores biodemográficos, sociales, clínicos y de laboratorio, medidos en el periodo cercano o durante la admisión, que se asocien al pronóstico vital y a la intensidad de los cuidados recibidos por los pacientes, particularmente el uso de ventilación mecánica invasiva. Por sus características, el estudio no pretende establecer un modelo con fines predictivos.
Método
El estudio corresponde a una cohorte retrospectiva. Fue realizado en Clínica Indisa, centro privado de 400 camas, ubicado en la Región Metropolitana de Santiago, que recibe principalmente pacientes de ingresos medios. Con motivo de la pandemia, la clínica desarrolló un proceso de reconversión de camas, pasando de 32 camas de unidades de cuidados intensivos de adulto en abril, a 102 en junio.
Participaron en la cohorte todos los pacientes hospitalizados desde el comienzo de la pandemia por COVID-19 en Chile (cuyo primer caso fue admitido el 11 de marzo), hasta el 25 de julio de 2020. Se utilizó como fuente de información la base de datos de pacientes COVID-19 elaborada por la clínica para el análisis y seguimiento de los casos, que se alimenta de distintas fuentes. Los datos biodemográficos, seguro de salud, resultados de laboratorio, nivel de atención (consultas médicas, urgencia u hospitalización), así como los días de estancia en servicios básicos, unidad de tratamientos y unidad de cuidados intensivos, y la condición al egreso se obtuvieron del sistema informático central. Los casos se identificaron a partir de los resultados de los test de reacción en cadena de la polimerasa con transcriptasa inversa de laboratorio, de los reportes del equipo de vigilancia y control de infecciones y del registro de derivaciones provenientes de centros externos. Los antecedentes clínicos, uso de ventilación mecánica invasiva y otros, se extrajeron directamente de las fichas clínicas electrónicas de cada paciente. Por último, también se validó la información revisando las notificaciones del sistema nacional Epivigila del Ministerio de Salud. La base fue anonimizada en dos etapas y posteriormente exportada al programa estadístico para su análisis.
Criterios de inclusión: pacientes de 15 años o más, admitidos en la clínica que al alta hubieran sido confirmados como COVID-19 mediante una retrotranscripción de reacción en cadena de la polimerasa positiva obtenida por muestras de hisopos nasales y faríngeos; o bien, un cuadro clínico y una tomografía axial computarizada compatible con neumonía viral por SARS-CoV-2, en un paciente con retrotranscripción de reacción en cadena de la polimerasa negativa, indeterminada o no disponible. Como tomografía axial computarizada compatible se consideró a los informes calificados como “apariencia típica” de acuerdo a los criterios de la Sociedad Chilena de Radiología[19].
Criterios de exclusión: mujeres embarazadas y pacientes con retrotranscripción de reacción en cadena de la polimerasa positiva como hallazgo (asintomáticos), hospitalizados por otras causas; pacientes que permanecían hospitalizados al cierre del seguimiento el 25 de julio.
Variables de resultado y predictores
La variable de resultado principal fue la muerte del paciente durante la hospitalización; como variable secundaria se evaluó la indicación de ventilación mecánica invasiva. Las variables independientes se seleccionaron a priori a partir de los estudios de cohorte publicados con mayores tamaños muestrales, entre aquellas que hubieran mostrado asociación independiente con la letalidad hospitalaria por COVID-19 en más de un estudio, y que pudieran ser predictores precoces de mal pronóstico. De esta forma se incluyó la edad, el sexo, el antecedente de enfermedad pulmonar crónica, de cardiopatía, de diabetes mellitus y de obesidad, junto con los niveles de proteína C reactiva, dímero D, creatinina y ferritina. También se incluyó el tipo de seguro de salud, público o privado. No se incluyó la hipertensión, que no ha demostrado asociación significativa con la mortalidad en la mayoría de las cohortes, ni el recuento de plaquetas, cuya utilidad estaría en los cambios detectados en mediciones seriadas[20],[21],[22] y no en los valores al momento de la admisión. La ferritina, que posee un rango muy amplio, fue expresada en microgramos por litros (originalmente en nanogramos por mililitro) para facilitar la interpretación de los coeficientes.
Las variables cuantitativas (edad, proteína C reactiva, dímero D, creatinina y ferritina) fueron analizadas inicialmente como tales, sin agrupar. Los datos sobre las comorbilidades están basados en la constancia del diagnóstico en la ficha clínica. La función renal fue analizada a través de la creatinina sérica más reciente. Los exámenes de laboratorio fueron realizados en la admisión, o dentro de las 48 horas previas o posteriores al ingreso. Si existían exámenes en ambos períodos, se seleccionó aquel más próximo a la admisión, dando preferencia al tomado con anterioridad al ingreso. Se analizó, además, posibles interacciones entre la diabetes y la ferritina[23], entre la diabetes y la creatinina, y entre el sexo y las distintas comorbilidades.
Análisis estadístico
Las estadísticas descriptivas incluyeron análisis de frecuencias (porcentajes) para variables categóricas y mediana, y rango intercuartil para variables continuas. Las comparaciones bivariadas se realizaron mediante la prueba U de Mann-Whitney para variables continuas, y mediante el test de Chi-cuadrado para variables categóricas. Se evaluaron los datos perdidos y se aplicó un procedimiento de imputación múltiple totalmente condicional con cinco imputaciones. Se utilizaron modelos de regresión logística binaria para analizar la asociación de las variables independientes y las variables de resultado.
El análisis se realizó mediante un procedimiento manual, considerando la bondad de ajuste y parsimonia del modelo, usando como referencia el criterio de información de Akaike. Se realizó un análisis de residuos y del cumplimiento de supuestos. Se compararon además las curvas de sobrevida de los pacientes mayores y menores de 65 años, evaluándose su asociación mediante el Log Rank test. Se consideró estadísticamente significativo un valor de p menor que 0,05. Los análisis fueron realizados con el software IBM SPSS V.21. De acuerdo a la fórmula propuesta por Peduzzi para regresiones logísticas[24], el tamaño muestral necesario para una menor probabilidad de ocurrencia del evento de 0,20 y 12 covariables, corresponde aproximadamente a 600 casos, por lo que se consideró que la muestra disponible tenía poder suficiente para satisfacer los objetivos del estudio.
El estudio se realizó cumpliendo los criterios de la Declaración de Helsinski. El protocolo del estudio fue aprobado por el Comité de Bioética Institucional de la Universidad Andrés Bello (UNAB), el cual se encuentra acreditado por el Ministerio de Salud de Chile. Para garantizar la confidencialidad de la información se aplicó a la base de datos un proceso de anonimización de dos pasos.
Resultados
En el período del estudio fueron atendidos un total de 2231 pacientes con sospecha o diagnóstico confirmado de COVID-19, de los cuales 826 fueron tratados en consultas ambulatorias, 419 en urgencia y 986 fueron hospitalizados. De estos últimos, al 25 de julio habían egresado 877 y permanecían internados 109. Se excluyeron 15 pacientes menores de 15 años, 52 embarazadas y 25 pacientes que no cumplieron los criterios diagnósticos definidos para el estudio, quedando constituida la muestra por 785 sujetos.
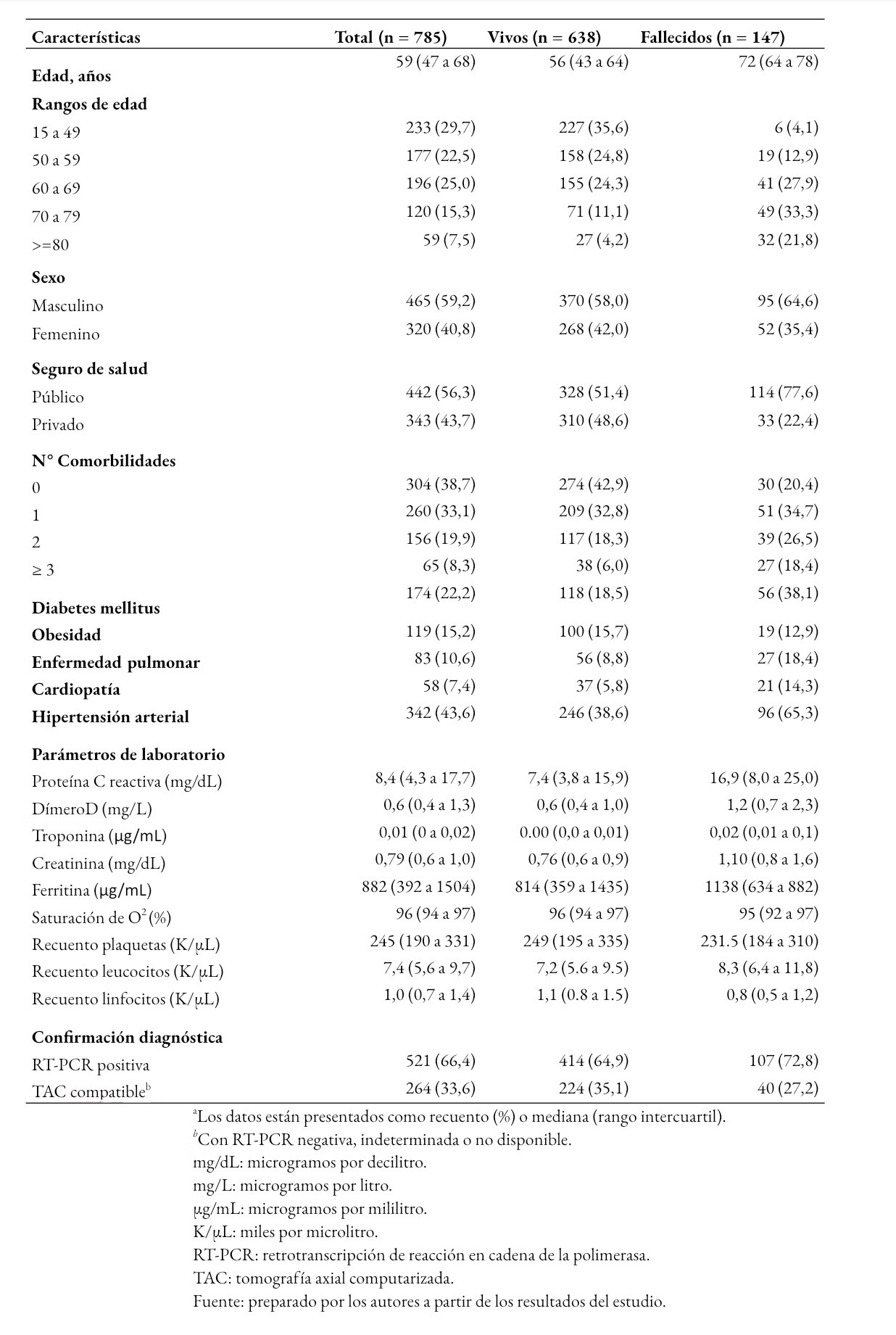
La Tabla 1 muestra las principales características biodemográficas, comorbilidades, biomarcadores y el método diagnóstico de los integrantes de la cohorte, según estado vital al egreso.
 Tamaño completo
Tamaño completo De las variables consideradas para el análisis, se detectaron datos perdidos en proteína C reactiva (n = 27; 3,4%), dímero D (n = 28; 3,6%), creatinina (n = 20; 2,5%) y ferritina (n = 37; 4,7%), que combinados produjeron un 11,1% de casos incompletos, los que fueron recuperados mediante el procedimiento de imputación.
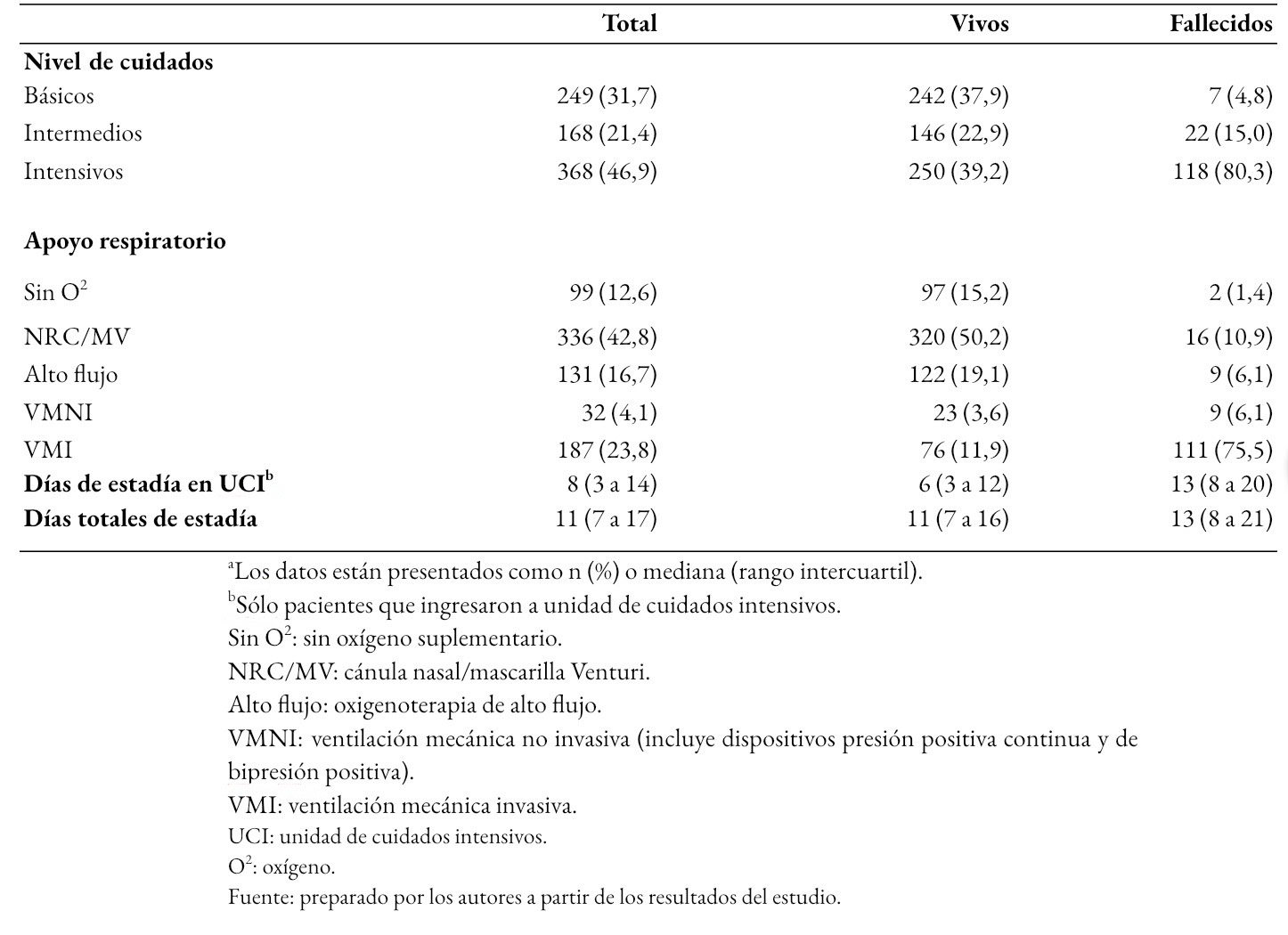
El nivel de cuidados y soporte de ventilatorio requeridos, así como la duración de la estancia se detallan en la Tabla 2. Aproximadamente, un 55% de los pacientes fue tratado en camas convencionales o de dependencia media, manejado sin oxígeno suplementario o con aporte de oxígeno por naricera o mascarilla Venturi. El restante 45% requirió dispositivos de alto flujo, ventilación mecánica no invasiva o invasiva. No se utilizó oxigenación por membrana extracorpórea en ningún paciente.
 Tamaño completo
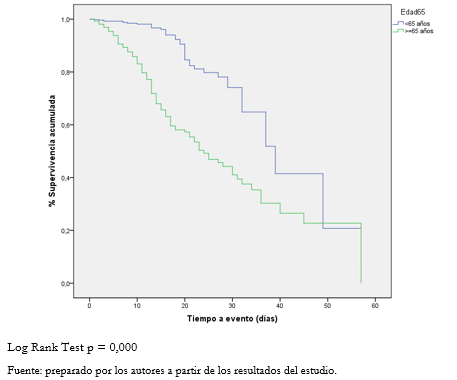
Tamaño completo La Figura 1 muestra la sobrevida acumulada de los integrantes de la cohorte, para aquellos pacientes de 65 años o más y los menores de 65.
 Tamaño completo
Tamaño completo Factores pronósticos de letalidad hospitalaria
La letalidad hospitalaria global de la cohorte fue de 18,7%. En pacientes que ingresaron a unidad de cuidados intensivos fue de 32,1%, y en quienes recibieron ventilación mecánica invasiva alcanzó 59,4%. La edad mostró una fuerte asociación con la mortalidad. En el grupo de 15 a 49 años la letalidad fue 2,6%, aumentando a 10,7% entre los de 50 a 59 años; 20,9% entre los de 60 a 69; 40,8% en el grupo de 70 a 79, y 54,2% en los de 80 años o más.
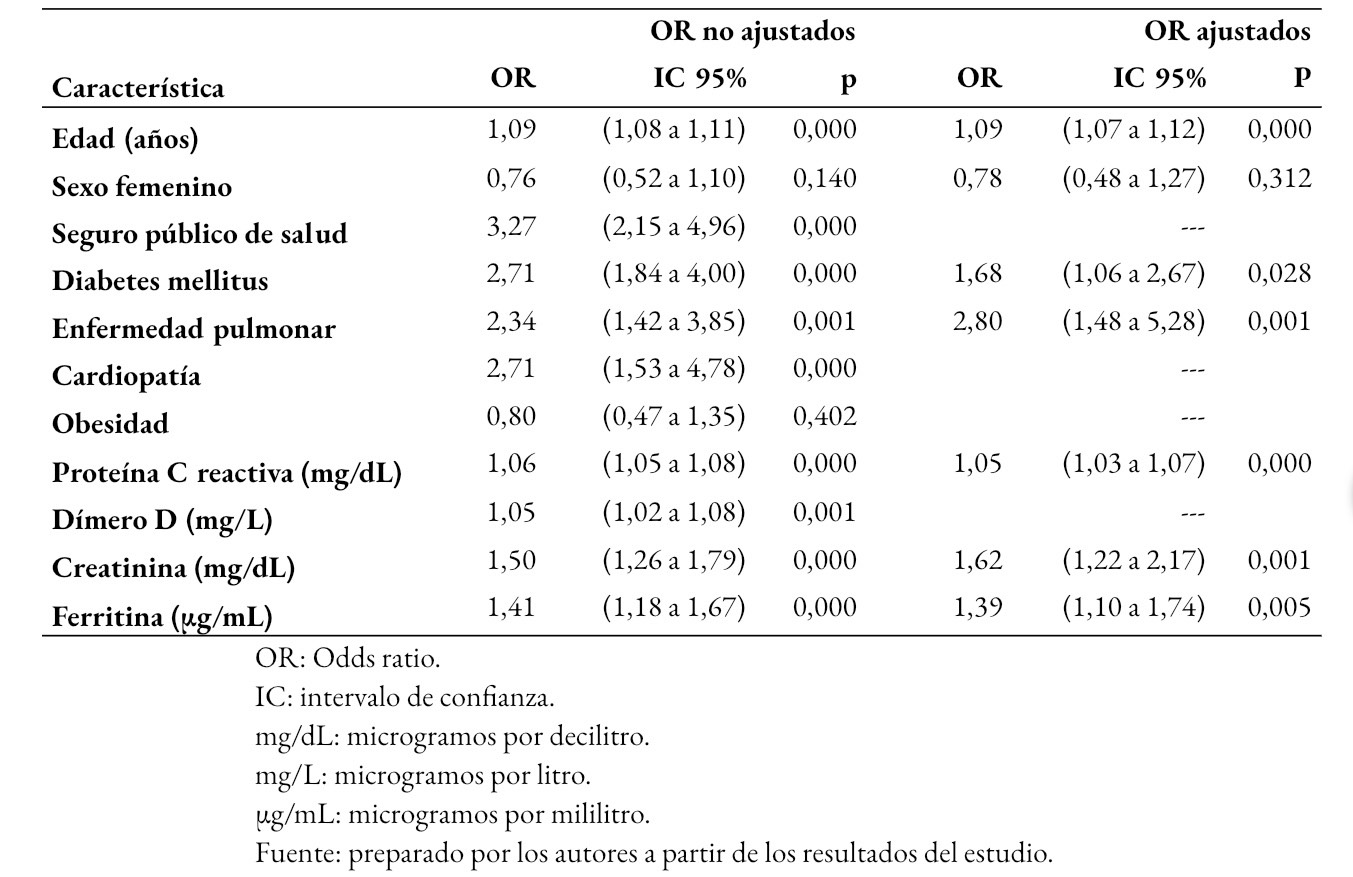
La Tabla 3 muestra los resultados del análisis bivariado inicial y los Odds ratio ajustados obtenidos con el modelo de regresión, que mostró una asociación significativa entre la letalidad y la edad, el antecedente de diabetes mellitus, de enfermedad pulmonar crónica, y valores elevados de proteína C reactiva, creatinina y ferritina. No se confirmaron como predictores independientes el sexo, el tipo de seguro de salud, el antecedente de cardiopatía u obesidad, ni los valores de dímero D. Se encontró además una interacción significativa entre la creatinina y la diabetes, de forma que la presencia o no de diabetes tiene menor efecto relativo cuando ya existe daño renal. No se identificaron otras interacciones significativas. Los supuestos del modelo se cumplieron satisfactoriamente. La especificidad del modelo fue de 95%, la sensibilidad de 42% y la exactitud global de 85%.
 Tamaño completo
Tamaño completo Uso de ventilación mecánica invasiva
El 23,8% de los pacientes recibió ventilación mecánica invasiva. Los análisis bivariados mostraron respecto del uso de ventilación mecánica invasiva un patrón similar al de la letalidad. La Tabla 4 muestra los resultados finales obtenidos con el modelo de regresión. En este caso se optó por categorizar la edad en decenios a partir de los 50 años, por la presencia de un brusco descenso en el uso de ventilación mecánica invasiva a partir de los 80 años, que afectaba el supuesto de linealidad.
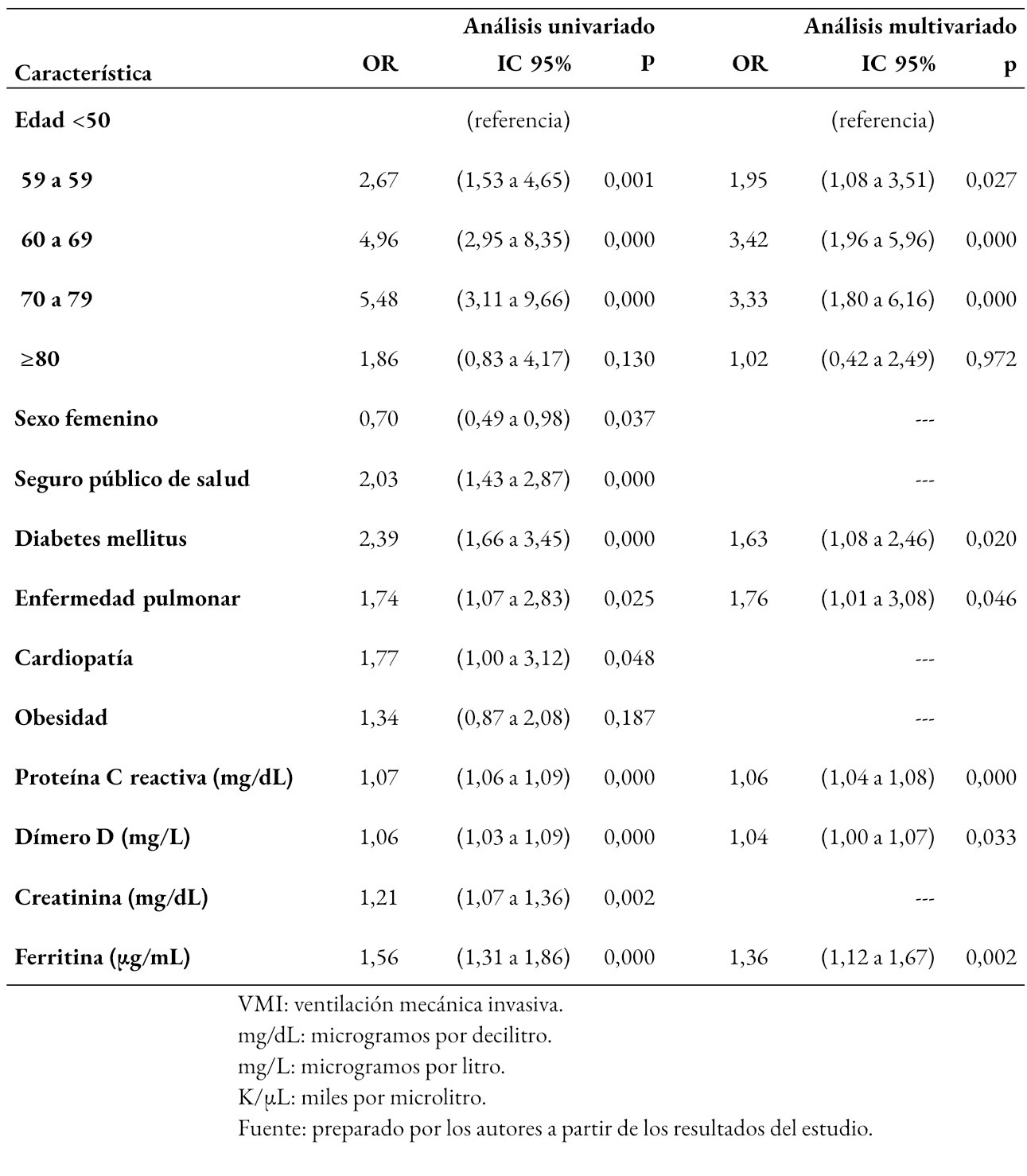 Tamaño completo
Tamaño completo Discusión
Principales hallazgos
La enfermedad afectó mayoritariamente a hombres, situación que se ha dado en todo el mundo. Del total de casos atendidos, alrededor de 45% recibió indicación de internación. Aproximadamente la mitad de los pacientes hospitalizados requirió ingreso a unidad de cuidados intensivos y alrededor de 1 de cada 4 fue conectado a ventilación mecánica invasiva. Estos resultados fueron similares a los reportados por diversos autores. Las diferencias con algunos estudios pudieran explicarse por la inclusión en ellos de pacientes que aún permanecían hospitalizados al cierre del seguimiento (a diferencia de nuestra cohorte que sólo incluyó casos egresados), distintos criterios para calificar los servicios de cuidados críticos y distinta proporción de comorbilidades en las poblaciones estudiadas.
Similar situación ocurre con la letalidad. Al respecto se puede afirmar que los resultados en nuestra cohorte se encuentran dentro del rango comúnmente observado, que oscila aproximadamente entre 20% de letalidad hospitalaria global, hasta guarismos del orden del 60% en los grupos de pacientes más graves. Otras cifras relativamente constantes que se reprodujeron en nuestra cohorte fueron una mediana de edad en torno a los 60 años, y los días de hospitalización en unidad de cuidados intensivos, sobre los que se reportan medianas entre 8 y 12 días en la mayoría de los estudios[3],[4],[5],[18].
El análisis multivariable mostró que la edad, el antecedente de diabetes y de enfermedad pulmonar crónica son factores predictores de muerte en estos pacientes. Lo mismo ocurre con la elevación de la proteína C reactiva, la creatinina y la ferritina, presentes al momento de la admisión, confirmando hallazgos previos[6],[8],[9],[23],[25]. Los mismos factores, con excepción de la creatininemia, pueden orientar al clínico para anticipar le necesidad de ventilación mecánica invasiva en el paciente con posterioridad a su ingreso, cuestión que adquiere relevancia en contextos donde la disponibilidad de ventiladores haya sido superada por la demanda. Lamentablemente la sensibilidad de los modelos es baja, lo que implica un riesgo importante de no detectar pacientes que van a requerir ventilación mecánica invasiva después del ingreso (falsos negativos). Por esto, es deseable diseñar y validar modelos con alto valor predictivo, aunque ello muchas veces se enfrenta con la dificultad para poder aplicarlos en la práctica diaria.
El estudio intentó distinguir las variables que pueden ser importantes al ingreso, de aquellas cuyo rol principal se da durante el seguimiento hospitalario. Ejemplo de ello fue la decisión de excluir el recuento de plaquetas. Si bien se ha observado asociación entre COVID-19 grave y menores recuentos de plaquetas, la disminución en general es leve y la mayoría de los pacientes exhibe valores al ingreso dentro de rango normal o sobre 100 mil por microlitro. En nuestra cohorte, sólo 11 casos (1,2%) presentaron valores inferiores o iguales a 100 mil por microlitro.
El descenso en el riesgo de ventilación mecánica invasiva en pacientes de edades muy avanzadas refleja la dificultad para adoptar decisiones terapéuticas agresivas en este grupo. En los pacientes fallecidos, alrededor de 30% tenía al momento de morir una autorización firmada por familiares, de limitación del esfuerzo terapéutico. Este subgrupo tenía alrededor de 80 años en promedio. La mención de los clínicos al esfuerzo “proporcional” del tratamiento en algunos de estos casos, apunta en el mismo sentido.
A diferencia de lo observado en diversas series, no encontramos que el sexo masculino fuera un factor de riesgo independiente de muerte en pacientes COVID-19. Si bien esta situación podría explicarse por variables de confusión relevantes no controladas en nuestro estudio, no se han descrito a nuestro entender factores patogénicos intrínsecamente ligados al sexo que expliquen el eventual mayor riesgo en hombres. Con respecto a la condición social de los pacientes, los datos iniciales sugerían que esta podía ser un factor predictor de mortalidad, pero en definitiva la diferencia observada fue explicada por variables de confusión (edad, comorbilidades) cuyo efecto fue corregido por el ajuste.
Como se indicó en la sección métodos, los autores optaron por tratar las variables continuas en su forma original, sin categorizarlas. Los argumentos en favor de limitar en lo posible la categorización artificial de variables continuas en los modelos de regresión han sido expuestos reiteradamente en la literatura[26],[27]. En las cohortes publicadas encontramos con frecuencia el uso de puntos de corte aplicados sin un criterio explícito o una justificación clara. En favor de esos autores, la interpretación de los datos se simplifica y en ocasiones facilita las comparaciones entre estudios. No obstante, agrega incertidumbre sobre los estimadores. Los autores sugieren usar los resultados respecto de estas variables como una referencia general que complemente el criterio clínico.
La limitación principal del estudio fue su carácter retrospectivo, que limita la calidad de los datos, la posibilidad de haber estudiado más a fondo algunas comorbilidades (por ejemplo, la obesidad), y expone a errores de clasificación. Aun así, es dudoso que la inclusión de una variedad mayor de predictores hubiera modificado sustancialmente los resultados, porque se incluyó aquellos con mayor evidencia previa y se evitó sobresaturar los modelos multivariantes. Otra limitación es que el estudio se haya realizado en una clínica de carácter privado, y tampoco se haya podido validar los modelos en otros grupos de pacientes, lo que restringe la posibilidad de generalizar los resultados, por ejemplo, a un espectro socioeconómico más amplio de la población, que incluya a grupos más precarios. Entre las fortalezas puede destacarse la baja proporción de datos perdidos. La condición inicial de los casos pudo influir en la pérdida de datos observada en algunos marcadores, por la menor disposición del médico a medirlos en pacientes menos graves, no obstante, no se encontraron diferencias importantes entre los casos con datos perdidos y completos, ni entre los coeficientes de los modelos con y sin imputación.
Conclusión
A diferencia de lo observado en diversas series, no encontramos que el sexo masculino fuera un factor de riesgo independiente de muerte en pacientes COVID-19. El pronóstico y factores predictores en esta cohorte de pacientes hospitalizados por COVID-19 fueron comparables, en su mayoría, a los reportados en estudios similares de países de mayores ingresos.
En términos generales, Chile enfrentó la pandemia por COVID-19 cuando esta ya se había extendido en otros continentes, permitiendo al país adoptar medidas anticipadas para dar cobertura a la atención de los casos más graves, incluyendo la integración público privada. Ello contribuyó a que la atención hospitalaria ofreciera resultados comparables a los de países de mayores ingresos.
En situaciones similares, sería recomendable la instauración temprana de registros nacionales prospectivos, que permitan estudiar cohortes representativas del conjunto del país, y un análisis más a fondo del efecto de los determinantes sociales en la salud de la población.

