Reporte de caso
← vista completaPublicado el 25 de noviembre de 2025 | http://doi.org/10.5867/medwave.2025.10.3082
Miotomía de Heller laparoscópica con fundoplicatura en acalasia esofágica tipo II: reporte de un caso clínico
Laparoscopic Heller myotomy with fundoplication in type II esophageal achalasia: A case report
Main messages
- Esophageal achalasia is a rare motility disorder, often diagnosed late, which negatively impacts patients’ quality of life.
- This case report illustrates the successful use of laparoscopic Heller myotomy with fundoplication in a patient with type II achalasia, resulting in marked symptom relief.
- Residual symptoms such as mild dysphagia and esophageal spasm may persist and require ongoing pharmacological and dietary management.
- This case report illustrates the successful use of laparoscopic Heller myotomy with fundoplication in a patient with type II achalasia, resulting in marked symptom relief.
Introduction
Peristalsis is the primary mechanism by which the food bolus moves through the digestive tract. Disturbances in the neuromuscular coordination of the esophageal body and the lower esophageal sphincter can result in motility disorders such as achalasia, distal esophageal spasm, and gastro-esophageal reflux disease, significantly impairing patients' quality of life. Achalasia, a rare esophageal motor disorder, is characterized by the absence of peristalsis and incomplete relaxation of the lower esophageal sphincter. Its global incidence ranges from 0.03 to 1.63 cases per 100 000 individuals per year, with a prevalence of approximately 10 cases per 100 000 worldwide [1].
This rare primary disorder shows no racial or gender predilection and most commonly affects individuals between 30 and 60 years of age. Its etiology is often idiopathic, with a possible genetic component supporting neurodegenerative hypotheses. Secondary causes include Chagas disease [2]. Dysphagia is the most prominent symptom, reported in 90% of patients and affecting both solids and liquids. Other common manifestations include regurgitation (75%), postprandial vomiting, retrosternal chest pain (50%), and heartburn (40%) [3]. The diagnostic evaluation of achalasia includes esophageal manometry, dynamic esophagography, and upper endoscopy. High-resolution esophageal manometry is considered the gold standard. Radiological studies, such as barium esophagography, are sensitive in 95% of cases, revealing findings such as aperistalsis and the characteristic “bird’s beak” sign, caused by esophageal dilatation and incomplete lower esophageal sphincter opening [4].
Treatment for esophageal achalasia is palliative, focusing on symptom relief and restoration of esophageal function. Laparoscopic Heller myotomy, a widely used surgical approach, reduces lower esophageal sphincter pressure and provides effective, long-lasting relief [5]. This case report aims to illustrate the effectiveness of a palliative surgical intervention in a patient with type II esophageal achalasia, highlighting substantial improvements in both clinical outcomes and quality of life.
Case presentation
This is the case of a 37-year-old female patient living in a rural area of the province of Azuay, Ecuador. The patient has completed higher education and holds three jobs, which involves prolonged exposure to physical and mental stress and irregular eating schedules. She lives with her two young children and is their primary caregiver, a situation that creates a moderately stressful psychosocial environment. Her personal history includes arterial hypertension for the past five years and she denies using tobacco, alcohol, or other substances. The patient presented with a five-year history of dysphagia, initially limited to solid foods, which progressively worsened to include liquids in the last three years. These symptoms were accompanied by sudden onset of oppressive precordial pain, rated 9 to 10 on the visual analogue scale (VAS), which radiated to the neck, jaw and teeth, along with odynophagia. She saw her doctor and an initial endoscopy revealed esophagitis, gastroesophageal reflux and gastritis. Two years ago, her symptoms intensified, prompting further diagnostic investigations:
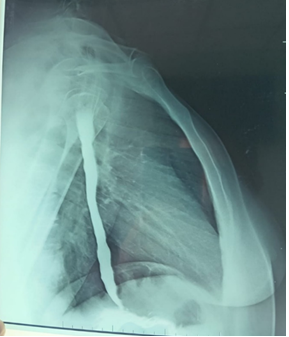
Esophagogastroduodenal series showed a dilated esophagus with a well-defined bird’s beak appearance at the esophagogastric junction (Figure 1).
Esophageal achalasia.
Esophageal manometry revealed altered peristalsis in the esophageal body, 100% of swallows with pan-esophageal pressurisation, normotensive lower esophageal sphincter with a resting pressure of 25.7 mmHg, incomplete relaxation (Integrated Relaxation Pressure = 15.1 mmHg), and altered esophagogastric junction contractility. No hiatal hernia was detected, and the gastro-esophageal junction was classified as type III A.
Based on the Chicago Classification Version 4.0, the diagnostic impression was Type II achalasia, consistent with the patient’s clinical presentation.
The patient underwent palliative surgical treatment consisting of a laparoscopic Heller myotomy combined with fundoplication as an anti-reflux technique (Figures 2 and 3).
Intraoperative image during laparoscopic Heller myotomy.
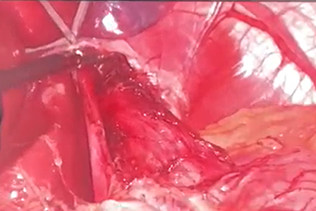
Intraoperative laparoscopic image corresponding to the final phase of Dor-type fundoplication.
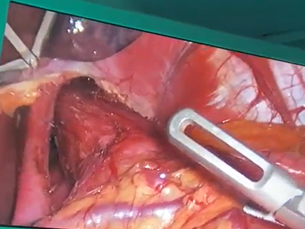
The patient was discharged 72 hours after surgery with instructions to follow a strict liquid diet, divided into 20 small portions per day, until her follow-up appointment. Seven days later, she reported difficulty eating and was advised to continue the liquid diet for an additional 45 days. A gradual transition to a soft diet followed, consisting of approximately 15 small meals per day for a further 30 days, while avoiding hard foods, lean meats, citrus fruits, spicy foods, hot dishes, and alcohol. Twelve months after surgery, the patient transitioned to a general diet, continuing to avoid foods known to trigger esophageal spasm or irritation, such as citrus fruits, spicy or acidic foods, and alcohol (Figure 4).
Postoperative findings in esophageal achalasia.
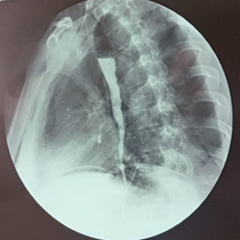
Discussion
In this case, the patient was successfully treated with laparoscopic Heller myotomy with Dor-type fundoplication, achieving a favorable clinical outcome with no significant recurrence of symptoms 12 months after surgery. This result is consistent with the literature, which establishes that laparoscopic Heller myotomy is highly effective in the treatment of type II achalasia, where clinical success is greater than 90%, this being the variant with the best surgical prognosis within the Chicago 4.0 classification [6].
When compared with alternative techniques such as per-oral endoscopic myotomy (POEM), several multicenter studies have shown that, although both techniques are effective, POEM is associated with a significantly higher incidence of gastroesophageal reflux (up to 57%) due to the absence of protective fundoplication [7]. In this case, the choice of the same technique allowed for adequate control of reflux, highlighting the importance of individualizing the therapeutic approach according to the subtype and clinical context.
In terms of long-term follow-up, it has been observed that the favorable results of laparoscopic Heller myotomy can be maintained for more than 5 years, especially in type II patients, who are more likely to have a lasting response without the need for retreatment [8]. This evidence suggests that long-term success depends not only on the type of intervention but also on the patient’s adherence to the postoperative regimen, as evidenced in the case presented, who maintained a fractional diet, regular check-ups, and endoscopic surveillance.
Similar case reports in Latin America, such as the one published by Pérez Cardoso et al., describe a patient with type II achalasia treated with laparoscopic Heller myotomy and Dor fundoplication, who also experienced complete resolution of dysphagia and a significant improvement in quality of life [9]. The similarities with our case highlight the consistency of results in different clinical contexts. However, unlike the present case, that report did not include one-year follow-up or systematic evaluation of residual symptoms such as spasms or precordial pain.
Finally, compared to less invasive options such as pneumatic dilation or botulinum toxin injection, laparoscopic Heller myotomy has demonstrated greater sustained efficacy and less need for retreatment, especially in young patients and those with type II achalasia. The choice of this technique in the patient presented in this case was based on this evidence, with the aim of providing a lasting solution and reducing the risk of long-term complications such as bronchoaspiration or significant weight loss.
Conclusions
Type II esophageal achalasia is a primary disorder of esophageal motility with a high therapeutic response to surgical intervention. Its timely recognition and diagnosis using high-resolution manometry allow an effective therapeutic strategy to be established that significantly improves the patient’s quality of life.
Laparoscopic Heller myotomy combined with Dor-type fundoplication proved to be a safe and effective therapeutic option in this case, achieving sustained resolution of dysphagia and preventing the onset of gastroesophageal reflux, a common complication in other endoscopic treatment modalities.
Structured postoperative management, with a progressive diet, nutritional education, and medical follow-up, was crucial in maintaining the clinical benefits achieved. The patient’s adherence to the care regimen was key to avoiding symptomatic recurrences and functional complications.
The implementation of fundoplication as part of the surgical approach allowed for effective control of post-myotomy reflux, which represents an advantage over procedures such as POEM, in which the absence of an antireflux valve increases the risk of subsequent esophagitis.
This case highlights the importance of early diagnosis and a multidisciplinary approach in patients with esophageal motor disorders. Early detection of symptoms and appropriate referral to specialized centers can optimize therapeutic outcomes and reduce long-term sequelae.

