Comunicaciones breves
← vista completaPublicado el 9 de enero de 2021 | http://doi.org/10.5867/medwave.2021.01.8097
Impacto de pandemia COVID-19 en la formación de residentes: análisis de una encuesta nacional a residentes de otorrinolaringología en Chile
How the COVID-19 pandemic affects specialty training: An analysis of a nationwide survey among otolaryngology residents in Chile
Resumen
Introducción La enfermedad por coronavirus 2019, o COVID-19, se ha convertido en una pandemia. Dada que la mayor carga viral de coronavirus de tipo 2 causante del síndrome respiratorio agudo severo (SARS-CoV-2) se encuentra en la vía aérea, los otorrinolaringólogos tienen un elevado riesgo de infección. Múltiples recomendaciones han surgido con respecto a las medidas de protección, incluidos la suspensión de procedimientos y cirugías electivas.
Objetivos Evaluar el impacto de la pandemia de COVID-19 en los programas de formación de otorrinolaringología a nivel nacional.
Métodos Estudio transversal de encuesta en línea a residentes de otorrinolaringología realizado durante abril de 2020. Se analizaron datos demográficos, actividades clínicas, turnos de llamado, infección por COVID-19, exposición a pacientes COVID-19 positivos, despliegue a otras especialidades, procedimientos y cirugías realizadas. Se utilizaron los portafolios quirúrgicos de años previos para comparar los resultados.
Resultados Completaron la encuesta 47 residentes, con 84% de tasa de respuesta; el 64% refirió haber acudido a su centro asistencial 10 días o menos durante el mes de abril de 2020. Con relación a procedimientos frecuentes tales como nasofibroscopía, endoscopia nasal rígida y drenaje de absceso periamigdalino, no fueron realizados por más del 40% de los residentes en el mes. Solo el 38% participó en cirugías, con un promedio de 0,6 procedimientos como primer cirujano; se constata una drástica disminución al comparar los registros de años anteriores. La mayoría de los residentes refieren estas medidas educativas complementarias: videoconferencias bibliográficas (87%), seminarios de casos clínicos en línea (60%), revisión de artículos (38%), entre otros.
Conclusiones La formación clínica y quirúrgica disminuyó drásticamente durante abril de 2020. Se deben considerar ajustes a los planes de estudio para disminuir el impacto negativo de la pandemia en la formación de los residentes.
Ideas clave
- Hasta el momento de elaboración de este estudio, no existen artículos que presenten el efecto de la pandemia por COVID-19 en la educación de residentes sanitarios en Chile.
- En este estudio presentamos un registro objetivo de la disminución de procedimientos y cirugías en residentes chilenos de otorrinolaringología, producto de la pandemia por COVID-19.
- Constituyen limitaciones de este trabajo la extensión temporal de sólo un mes, y de seguimiento durante la evolución de la pandemia.
- También constituyen limitantes la ausencia de datos comparativos sobre cirugía endoscópica funcional y cirugía oncológica de cabeza y cuello, esto debido a datos incompletos en el autorreporte histórico en esas áreas.
Introducción
El 11 de marzo de 2020, la Organización Mundial de la Salud (OMS) declaró a la enfermedad por coronavirus (COVID-19), causante del síndrome respiratorio agudo severo (SARS-CoV-2), como una pandemia global[1]. Dado la alta carga viral que se encuentra en la vía aérea[2], los otorrinolaringólogos se encuentran en alto riesgo de infección. Esto, dado que múltiples procedimientos de la especialidad como endoscopía nasal rígida, nasofibroscopia, taponamiento nasal anterior, traqueostomía, entre otros; involucran la vía aérea. Esto se suma a que dichos procedimientos, además, pueden causar aerolización de partículas virales[3],[4].
En respuesta, han surgido múltiples guías clínicas y recomendaciones de sociedades científicas referidas a las medidas protectoras requeridas para realizar dichos procedimientos. Dentro de las medidas recomendadas destacan suspensión de procedimientos electivos y cirugías, reducción de personal durante turnos presenciales, creación de rotaciones de cohorte semanales para residentes, realización de cirugías en el menor tiempo posible y por el cirujano más experimentado, entre otras[5],[6],[7],[8].
Considerando lo anterior, y sumando que la mayoría de la consultas otorrinolaringológicas ambulatorias, procedimientos y cirugías son electivas, sospechamos que la pandemia COVID-19 está afectando negativamente la formación de residentes debido a la reducción significativa de la oportunidad quirúrgica y exposición a pacientes ambulatorios[9].
A nuestro conocimiento, hasta la fecha que este estudio fue completado, no existían artículos describiendo el efecto de la pandemia por COVID-19 en la educación de residentes en Chile.
El objetivo de este estudio es evaluar el impacto de la pandemia por COVID-19 en los programas de formación de otorrinolaringología nacionales y describir la reducción de la oportunidad quirúrgica.
Métodos
Encuesta de oportunidades clínicas
Se realizó un estudio transversal basado en encuestas, evaluando el periodo entre el 1 y el 30 de abril de 2020. En la actualidad existen cinco programas de otorrinolaringología en Chile, desde los cuales se reclutaron a los residentes, a través de una encuesta en línea por la plataforma Google, enviada por correo electrónico. La información de contacto fue facilitada por los jefes de programa de cada universidad.
Se obtuvieron datos demográficos, años de formación y la siguiente información correspondiente al mes de abril de 2020: actividad clínica, turnos de llamado, estado de infección COVID-19, exposición a pacientes COVID-19, despliegue a otras especialidades como apoyo, procedimientos diagnósticos/terapéuticos realizados y participación en cirugías (primer o segundo cirujano). Se definió como paciente COVID-19 positivo a aquellos con reacción en cadena de la polimerasa con transcriptasa inversa (RT-PCR) confirmada, y casos sospechosos con resultado pendiente. La encuesta estuvo abierta a respuesta desde el 11 al 18 de mayo de 2020.
Registros clínicos históricos
Con respecto a los registros clínicos históricos de procedimientos diagnósticos/terapéuticos de la especialidad, se lograron obtener solamente de los portafolios autoreportados del programa de formación de la Pontificia Universidad Católica de Chile de los años 2017 a 2019. En relación al registro de cirugías realizadas por los residentes en los años de formación previos, se obtuvieron datos, también de portafolios quirúrgicos autorreportados, de dos programas de formación: Pontificia Universidad Católica de Chile y Universidad de Chile para los períodos 2017 a 2019 y 2006 a 2016, respectivamente. Ambos portafolios corresponden a información registrada personalmente por los residentes luego de asistir a cirugías o realizar procedimientos. No se requirió determinación de tamaño muestral, dada la naturaleza del estudio.
Análisis estadístico
La recolección de datos fue realizada anónimamente en una base encriptada. Al analizar los datos, si estos presentaban distribución normal, la estadística descriptiva se expresó usando el promedio y desviación estándar; si no existía distribución normal se informó la mediana. Para comparar variables categóricas se utilizó el test de Chi-cuadrado. Los promedios obtenidos se compararon usando el test de T-student. Fue considerado significativo un valor p < 0,05 (significancia de 5%).
Resultados
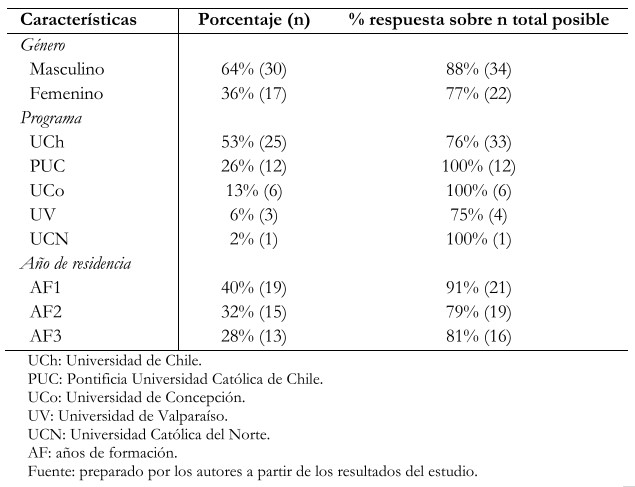
Respondieron la encuesta 47 residentes, correspondiente a una tasa de respuesta del 84%. La edad promedio fue de 29,7 ± 3,2 años (rango 25 a 35). Los detalles demográficos se observan en la Tabla 1. El 6% de los residentes fue enviado a cuarentena preventiva, debido a pertenecer a algún grupo de riesgo para la infección por SARS-CoV-2. El 50% (n = 23) atendió a pacientes confirmados o sospechosos de COVID-19 durante abril de 2020; de ellos solo el 13% (n = 6) requirió cumplir cuarentena preventiva por contacto estrecho sin uso de elementos de protección personal adecuados, y un residente resultó infectado por COVID-19.
El promedio de pacientes confirmados/sospechosos evaluados por residente fue de 8,1 ± 8,7 (rango 1 a 30). El 13% (n = 6) de los residentes fue derivado a apoyar otros servicios, siendo medicina interna el más frecuente (5/6).
 Tamaño completo
Tamaño completo Actividades clínicas
El resumen de actividades clínicas realizadas durante abril de 2020 se observa en la Tabla 2. El 65% de los residentes acudió menos de 10 días del mes a sus respectivos centros de formación y el 68% examinó menos de 11 pacientes durante su práctica ambulatoria en todo el mes.
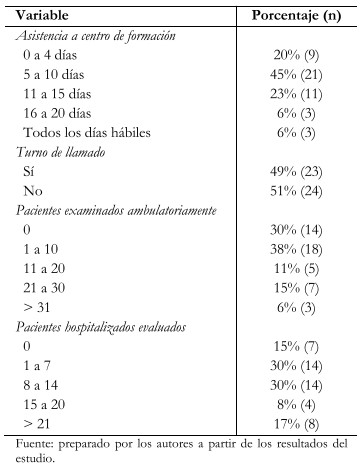 Tamaño completo
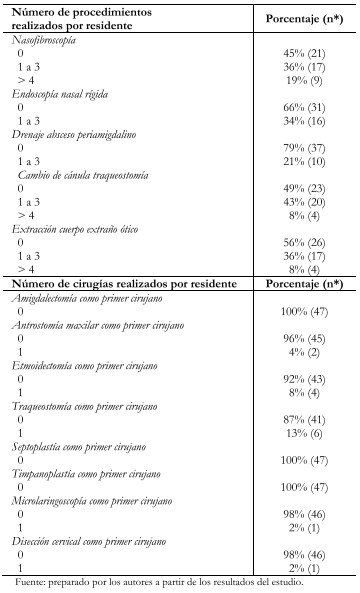
Tamaño completo Con respecto a los procedimientos efectuados, solo el 55% de los residentes realizó nasofibroscopias, 34% endoscopía nasal rígida y 21% drenaje de absceso periamigdalino como se observa en la Tabla 3. Si analizamos los datos obtenidos del programa de la Pontificia Universidad Católica de Chile, se observa una disminución significativa del promedio de procedimientos por residente para nasofibroscopía (13,1 ± 7,5 versus 1,4 ± 1,5; p = 0,001), endoscopía nasal rígida (3,6 ± 2,9 versus 0,4 ± 0,7; p = 0,001), cauterización nasal anterior (0,8 ± 0,5 versus 0,1 ± 0,3, p = 0,002), evaluación endoscópica de la deglución (3,6 ± 2 versus 0 ± 0,1; p = 0,000).
 Tamaño completo
Tamaño completo Actividad quirúrgica
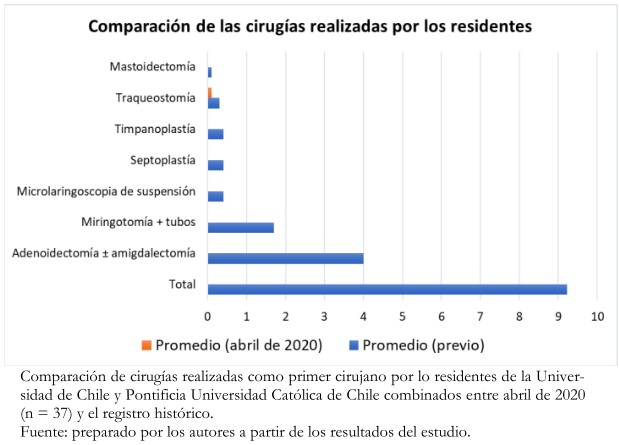
De los residentes encuestados, el 62% (n = 29) no participó en cirugías. De los 18 que sí participaron, el 67% (n = 12) lo hizo como primer cirujano, con un promedio de 0,6 + 1,2 (rango 0 a 5) cirugías por residente. La intervención más frecuente fue la traqueostomía quirúrgica (n = 6), seguido por la etmoidectomía (n = 4) como se ve en la Tabla 3. Se utilizaron los datos históricos autoreportados por la Universidad de Chile y la Pontificia Universidad Católica de Chile para comparar el número de cirugías de abril de 2020 con el promedio histórico, observándose una disminución drástica en la exposición quirúrgica, lo que se grafica en la Figura 1.
 Tamaño completo
Tamaño completo Herramientas educacionales
En la encuesta se les solicitó a los residentes proveer las medidas tomadas por sus programas para promover la educación continua y formación a distancia. La mayoría de los residentes refirió videoconferencias bibliográficas (87%, n = 41) y seminarios en línea de casos clínicos (60%, n = 28). Otras medidas mencionadas fueron Journal Club semanales (38%, n = 18), revisiones bibliográficas (34%, n = 16), análisis de videos de técnicas quirúrgicas (15%, n = 7), oportunidades de simulación (17%, n = 8), entre otros (8%, n = 4).
Discusión
En esta encuesta, describimos como la pandemia actual ha perjudicado la educación de residentes en otorrinolaringología, dada la contracción de oportunidades clínicas y quirúrgicas. Esto se vio reflejado en la reducción de procedimientos realizados por los residentes con una disminución significativa de en nasofibroscopías, endoscopia nasal rígida, entre otros. Creemos que el ítem más importante afectado es la oportunidad quirúrgica. Solo el 38% de los residentes tuvo exposición a pabellón, siendo solo el 25% primer cirujano en un mes completo. Se evaluó si existía asociación o no entre ser primer cirujano y años de formación, sin embargo, esta asociación no fue estadísticamente significativa (p = 0,0631). Creemos que dentro de los factores posiblemente involucrados en el impacto podrían estar la cantidad de residentes por centro formativo, extensión de cuarentenas obligatorias en las ciudades y tamaño de población atendida los hospitales docentes.
Dado que no sabemos cuándo será el fin de esta pandemia, se debe prestar atención en buscar nuevas herramientas educacionales a los residentes, en especial con respecto a las habilidades quirúrgicas. Algunas de las medidas tomadas por los jefes de programa de los respectivos departamentos durante el mes de abril son videoconferencias (bibliográficas, seminarios de casos, journal club semanales), revisiones bibliográficas, análisis de técnica quirúrgica y oportunidades de simulación.
El SARS-CoV-2 arribó a Chile el 3 de marzo de 2020, solo habiendo 16 025 reportados a finales de abril. Al momento que la encuesta fue completada, existían 65 393 casos confirmados[10]. Sospechamos que el nivel de actividad de la especialidad y de los residentes fue severamente afectado, puesto que el máximo de infección fue en junio. Debido a que, de momento, múltiples instituciones siguen restringiendo la actividad ambulatoria, no sabemos cuán profundamente esta pandemia afectará a los programas de formación. Creemos que el Ministerio de Salud debe tomar medidas al respecto, en orden a asegurar una educación completa y competente para la cohorte actual de residentes. Otorrinolaringología es una de muchas especialidades quirúrgicas que deben haber sido afectadas por la disminución de casos que requieren de cirugías.
Describimos la primera experiencia que objetiva la disminución de exposición clínica y quirúrgica de los residentes en Chile debido a la pandemia por COVID-19. En el mundo existe preocupación por la educación y seguridad de los estudiantes de postgrado. En este contexto, Cai y colaboradores[11] realizaron una encuesta que evaluó a 82 residentes de 51 programas, reportando que el 98% de los programas estadounidenses han ejecutado políticas que incluyen reducción de residentes en cirugías, uso de mascarillas autofiltrantes para procedimientos productores de aerosoles y reducción de frecuencia en cambios de cánula de traqueostomía. Si bien la mayoría de los residentes según su encuesta se sintió satisfecho con las medidas tomadas, existía una mayor percepción de riesgo a enfermar en comparación a sus docentes. No se evaluaron cirugías ni procedimientos en este trabajo.
Dentro de las limitaciones de nuestro trabajo incluimos la extensión temporal de sólo un mes y de seguimiento durante la evolución de la pandemia. Además, la ausencia de datos comparativos sobre cirugía endoscópica funcional y cirugía oncológica de cabeza y cuello, esto debido a datos incompletos en el autorreporte histórico en esas áreas.
Conclusiones
La pandemia COVID-19 es una contingencia nueva, agresiva y aparentemente duradera. No existe certeza con respecto a cuán profunda va a ser su repercusión en la formación de residentes. Describimos una importante disminución en la atención de pacientes, procedimientos y cirugías en otorrinolaringología.
Se requieren de medidas adicionales y seguimiento cercano para sobrellevar esta adversidad. Los programas de residencia, con el apoyo de la autoridad sanitaria, necesitan modificar el currículo actual, de modo de asegurar la seguridad de sus residentes y también para proveer oportunidades educacionales compensatorias.
Anexo
Anexo: Encuesta Oportunidades de atención en el programa de formación de otorrinolaringología durante pandemia COVID-19.

