Estudios originales
← vista completaPublicado el 23 de mayo de 2019 | http://doi.org/10.5867/medwave.2019.04.7637
Determinantes de la salud en adultos de la ciudad de Chimbote, Perú: estudio descriptivo
Health determinants in adults in Chimbote, Peru: A descriptive study
Resumen
Objetivo Describir los determinantes de la salud en adultos de la jurisdicción de la Red de Salud Pacifico Norte y Sur de la ciudad de Chimbote.
Métodos Se realizó un estudio descriptivo no controlado. Los determinantes de la salud fueron descritos mediante las dimensiones: del entorno biosocioeconómico, de los estilos de vida y de las redes sociales y comunitarias. Para el análisis descriptivo de variables categóricas se utilizaron frecuencias relativas y absolutas.
Resultados Se incluyeron 1496 adultos. En los determinantes del entorno biosocioeconómico, el 62,2% son mujeres y 53,3% adultos mayores. En determinantes de estilos de vida, el 52,4% no fuma, ni ha fumado nunca de manera habitual, 50,5% no consumen bebidas alcohólicas y 66,9% duerme de seis a ocho horas. En determinantes de apoyo comunitario, el 53% se atendió en estos 12 últimos meses en un puesto de salud, 47,5% considera que el lugar donde se atendió se encuentra a regular distancia desde su vivienda y 64,6% tiene Seguro Integral de Salud del Ministerio de Salud peruano, SIS–MINSA.
Conclusión La mayoría de las personas estudiadas culminó estudios secundarios y no accedió a mejores escalas salariales. La mayoría cuenta con vivienda propia y servicios básicos, pero viven en hacinamiento. Predomina el sedentarismo y alimentación elevada en carbohidratos.
|
Ideas clave
|
Introducción
La salud es el estado completo de bienestar físico, mental y social de la persona[1]. La salud se ve condicionada por determinantes sociales de la salud , los que para efectos de este trabajo se entienden como “un conjunto de factores sociales, económicos, políticos y de estilos de vida“, que se constituyen en el transcurso de la vida del ser humano, y a futuro se traducen en impactos en la salud[2].
Considerando todas las edades, la población a nivel mundial se incrementó en 1,2% entre el año 2000 y 2017, totalizando 7 530 millones de habitantes en el mundo. De ellos, el 65% tiene entre 18 y 64 años[3]. Las personas usualmente adoptan comportamientos no saludables (consumo de tabaco, alcohol, adopción de dietas no saludables)[4],[5],[6], y están expuestos a determinantes sociales (pobreza, lugar de residencia, sexo, educación, entre otros) que influyen en su salud. Además, estos son precedentes de la ocurrencia y co-ocurrencia de enfermedades no transmisibles y enfermedades transmisibles en la edad adulta[7],[8],[9].
A pesar de los adelantos en el diagnóstico y tratamiento de las enfermedades, hay estudios que mencionan que los determinantes sociales de la salud en las personas no han cambiado, sino por el contrario, son más complejos[10]. Debido a la situación de salud insatisfactoria de la población, el sistema de salud ha fortalecido la atención integral primaria de la salud, trasladando la prioridad de atención a la promoción y prevención de la salud de la enfermedad[2],[11]. El objetivo del presente estudio fue describir los determinantes de la salud en adultos de la jurisdicción de la Red de Salud Pacífico Norte y Sur de la ciudad de Chimbote, Perú.
Métodos
Diseño y contexto del estudio
Estudio descriptivo con diseño de una sola casilla[9]. El presente trabajo se desarrolló en la ciudad de Chimbote. Chimbote está constituida por la Red de Salud Pacífico Norte y Red de Salud Pacífico Sur. Ambas están integradas por seis micro redes, y solo cuatro de ellas (Red de Salud Pacífico Norte: El Progreso, Magdalena Nueva y Miraflores; y Red de Salud Pacífico Sur: Yugoslavia) se ubican en la ciudad de Chimbote y participaron del estudio. El marco muestral estuvo conformado por los adultos (mayores de 18 años) de las micro redes de salud, seleccionadas. Para el estudio se obtuvo una muestra probabilística de 1 496 adultos mediante un muestreo aleatorio simple.
Participantes
Para el estudio, se consideraron elegibles hombres y mujeres a partir de los 18 años, atendidos en las redes de salud seleccionadas. Se excluyeron a las personas con trastornos mentales que estuvieran impedidas de completar los procedimientos del estudio.
Procedimientos
Para llevar a cabo el presente estudio, primero se contó con el permiso de la Red de Salud Pacífico Norte y Red de Salud Pacífico Sur. Posteriormente, la investigadora principal obtuvo el consentimiento informado y luego procedió a aplicar el instrumento de evaluación Determinantes de Salud en Adultos del Perú a los participantes seleccionados. El periodo de ejecución del estudio se dio entre abril y septiembre de 2016. Ninguna encuesta fue excluida del estudio.
Instrumentos
El cuestionario de Determinantes Sociales de la Salud fue adaptado y validado por 10 expertos[12]. En seguida, por medio de la prueba estadística, se mostró una alta confiabilidad reportando un indicador mediante el α de Cronbach (α = 0,89). El instrumento consta de 30 ítems, distribuidos en cuatro partes:
- Datos de identificación.
- Determinantes del entorno biosocioeconómico: sexo, edad (adulto joven, adulto maduro y adulto mayor)[12], grado de instrucción, ingreso económico, ocupación del jefe del hogar, tipo, tenencia, material y cantidad de personas de la vivienda, servicios básicos en la vivienda, eliminación de las excretas y disposición de la basura.
- Determinantes de los estilos de vida: consumo de tabaco, consumo de alcohol, horas de sueño, frecuencia de aseo personal, uso de los servicios de salud, actividad física y consumo de alimentos.
- Determinantes de las redes sociales y comunitarias: apoyo natural, apoyo social, tiempo de espera y calidad de la atención de los servicios de apoyo y exposición a pandillaje.
Variable dependiente: determinantes de la salud
Los determinantes de la salud son un “conjunto de factores personales, sociales, económicos y ambientales que determinan el estado de salud de la persona”[2]. En este estudio describimos los “determinantes de la salud” mediante las dimensiones previamente escritas en la sección de instrumentos (determinantes del entorno biosocioeconómico, determinantes de los estilos de vida, y determinantes de las redes sociales y comunitarias). Para el análisis se usaron las categorías correspondientes a cada dimensión.
Plan de análisis
Para el análisis, se creó una base de datos en Microsoft Excel 2016 y se exportó para el procesamiento de datos al software estadístico IBM SPSS Statistics 24,0. Para el análisis descriptivo de las variables categóricas se utilizaron frecuencias relativas y absolutas.
Consideraciones éticas
Se respetó la confidencialidad ofrecida en el consentimiento del estudio original, a través de la anonimización de los datos, su manejo restringido y registro encriptado. El presente estudio fue revisado por el Comité Institucional de Ética en Investigación de la Universidad Católica Los Ángeles de Chimbote (CIEI-ULADECH Católica), quién emitió sendos informes de autorización N°006-2016-CEI-VI-ULADECH-Católica, previamente a su ejecución.
Resultados
En cuanto a los determinantes del entorno biosocioeconómico, el 62,2% son mujeres; 53,3% son adultos mayores; 52,2% tienen como grado de instrucción secundaria completa/secundaria incompleta; y 38,8% tiene un ingreso económico menor a 750 nuevos soles (Tabla 1).
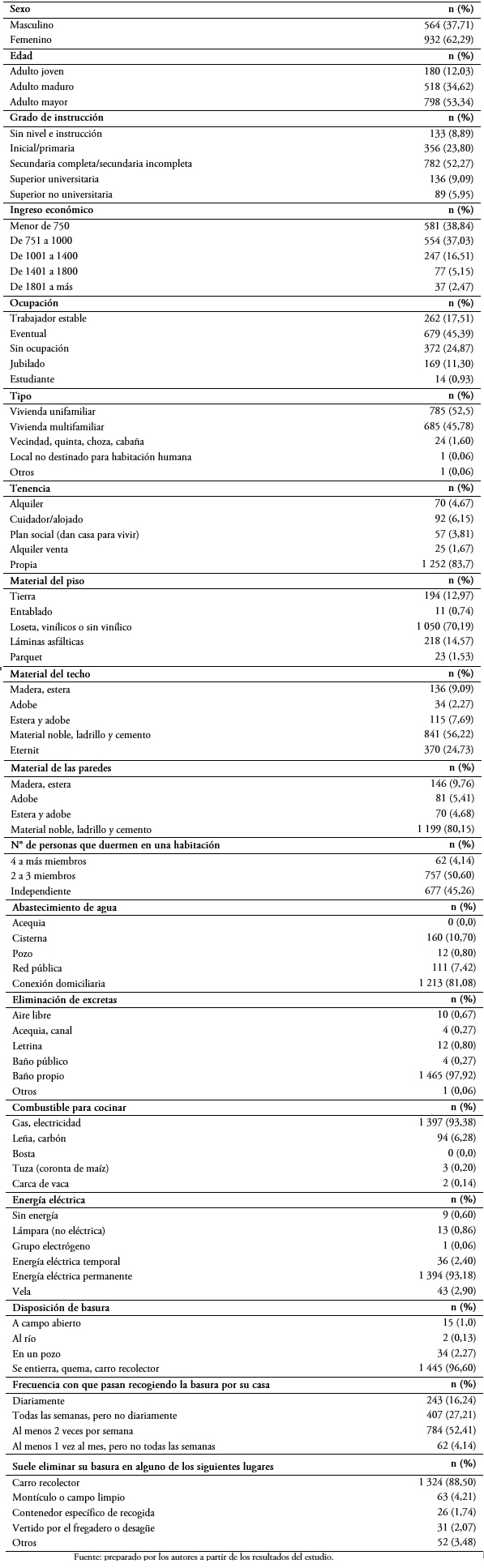 Tamaño completo
Tamaño completo En los determinantes de estilos de vida, el 50,5% no consume bebidas alcohólicas; 66,9% duerme de seis a ocho horas; 54,4% no se realiza exámenes médicos periódicos. En cuanto a su alimentación, 27,4% consume frutas tres o más veces a la semana y 28,5% consume dulces y gaseosas menos de una vez a la semana (Tabla 2).
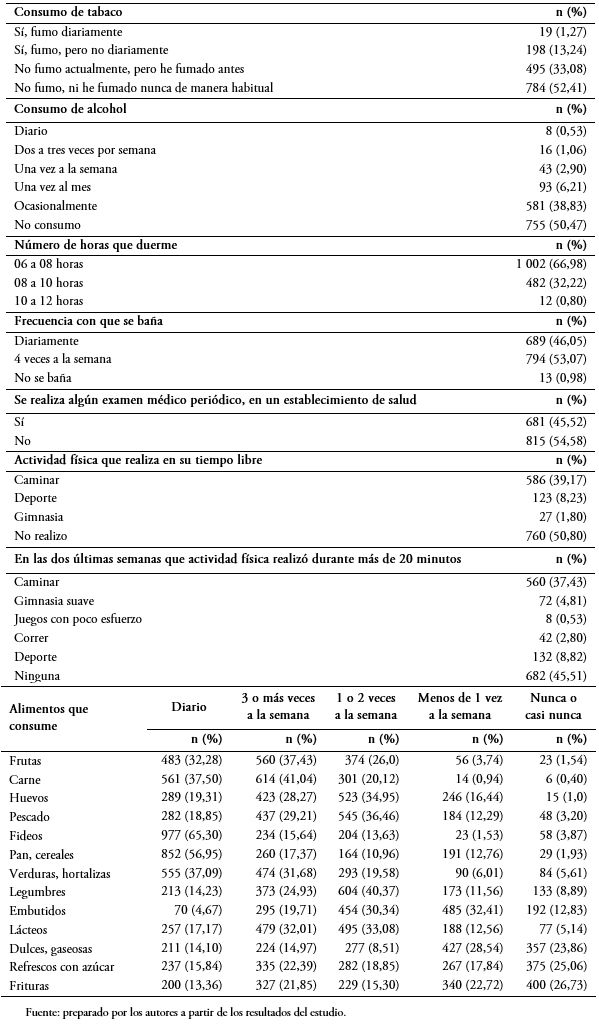 Tamaño completo
Tamaño completo Respecto a los determinantes de apoyo comunitario, el 53% se atendió en los últimos 12 meses en un puesto de salud; el 64,6% cuenta con el Seguro Integral de Salud (SIS) del Ministerio de Salud (MINSA); el 52,5% indicó que sí existe pandillaje o delincuencia cerca de su casa; y 96,9% no recibe ningún tipo de apoyo social organizado (Tabla 3).
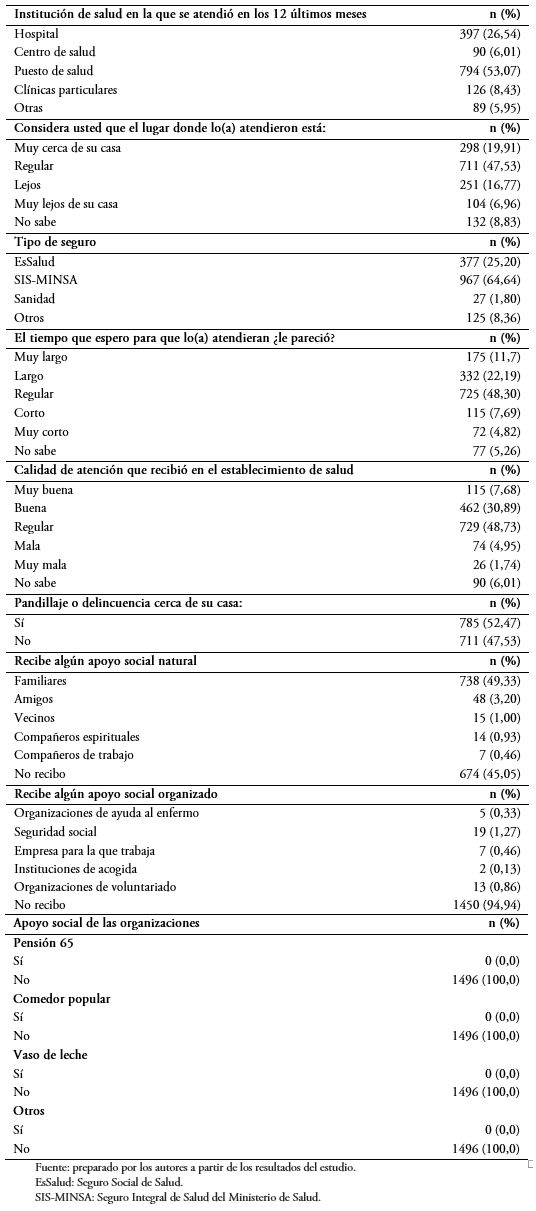 Tamaño completo
Tamaño completo Discusión
El incremento de la esperanza de vida junto con el descenso de la natalidad implica un envejecimiento de la población y, con ello, nuevos problemas para una sociedad moderna y cambiante que ha situado a los adultos mayores en una escala de bajo reconocimiento social. Aquí radica la importancia de hacer un análisis de las condiciones biosocioculturales, alimentarias y sociales en las que se desarrolla este grupo de población[6],[13].
En los determinantes biosocioeconómicos, encontramos que más de la mitad de los encuestados fueron adultos mayores, la mayoría pertenecen al sexo femenino y más de la mitad tuvo acceso a educación secundaria completa/secundaria incompleta; lo cual es similar a lo reportado en pobladores de una comunidad de Trujillo, Perú[14], excepto que en su población mayoritaria fueron adultos maduros (100%). Asimismo, los datos concuerdan con Quiroz R, en cuyo estudio más de la mitad de los participantes fueron mujeres, el 41% de la población incluida alcanzó estudios del nivel secundario y 75,8% perteneció a la etapa adulta joven. Otro estudio de determinantes sociales de la salud desarrollado en Colombia menciona que el 48,9% de su población de estudio fue adulto de mediana edad (entre 41 y 64 años), más de la mitad fue de sexo femenino (61,4%) y 35,2% alcanzó estudios superiores universitarios de pregrado y postgrado[15]. Nuestros resultados y los estudios previamente descritos demuestran que la edad influye en las variaciones de las brechas en educación, y este último en los ingresos económicos afectando la calidad general de vida de los individuos[16].
Con relación al ingreso económico, la mayoría reportó percibir ingresos menores del sueldo mínimo (750,00 soles peruanos). Asimismo, gran parte de los entrevistados refirió laborar eventualmente. Ello concuerda con lo reportado por los pobladores de Piura[17], quiénes manifiestan percibir cifras menores al sueldo mínimo, refirieron trabajar eventualmente (74,9%) y la minoría reportó estar desempleado (0,9%). Sin embargo, en un estudio realizado en Colombia, los participantes pertenecieron al nivel socioeconómico alto (88,9%), percibieron más de seis sueldos mínimos (37,3%), pero el 30% refirió encontrase desempleado[15]. Las disparidades de los puestos laborales, así como la remuneración percibida estarían en función a la edad y a los grados académicos alcanzados, mientras que, las personas que no logran este nivel de preparación estarían obligados a aceptar condiciones laborales deficientes con remuneraciones por debajo del sueldo mínimo. Estudios previos concluyeron que, las personas que logran ingresos económicos superiores, tendrían mejor autocuidado de su salud[18].
Referente al tipo de vivienda, la mayoría de los participantes reside en viviendas unifamiliares, aunque, un poco más de la mitad refirió compartir habitación con más de tres miembros de su familia. Esto es similar a los estudios de Piura[17] y Colombia[17]. La obtención de sus viviendas propias podría deberse al menor costo de los terrenos en aquellos años o mediante las invasiones que con el tiempo lograron acceder al título de propiedad, por ende, las viviendas mayormente fueron construidas sin asesoría de expertos. Por esta razón, no previeron el incremento de los miembros de la familia destinándolos al hacinamiento en áreas reducidas[19],[20].
Por otro lado, más de la mitad refirió abastecerse de agua potable a través de conexiones domiciliarias. Respecto a la eliminación de excretas, la mayoría informó contar con baño propio. El combustible que utilizan para cocinar sería el gas o la electricidad, las viviendas contarían con energía eléctrica permanente, y casi la mayoría usa el carro recolector para la eliminación de desechos. Esto es similar a lo reportado en pobladores de Piura[17] y en el estudio realizado en una comunidad rural en Colombia[21], el 97% tiene servicio eléctrico y más de la mitad recolecta la basura de forma adecuada (58,6%), pero la mayoría carece de acceso al agua potable (69%), así como del servicio de alcantarillado (20,7%). Estas diferencias de los niveles de organización entre gobiernos estarían dadas por las políticas sociales orientadas a la superación de la pobreza, la calidad de vida y al desarrollo social que algunos gobiernos han trabajado en los últimos años. No obstante ello, aún resulta necesario el compromiso en las autoridades para mejorar la calidad de vida de los ciudadanos para que resuelvan de manera eficiente los problemas de índole social[22].
En cuanto a los determinantes del estilo de vida, un poco más de la mitad de los encuestados refirieron no fumar, ni consumir bebidas alcohólicas y la mayoría duerme de seis a ocho horas. Asimismo, más de la mitad no se realizan exámenes médicos periódicos; la mitad de los encuestados tampoco sale a caminar en su tiempo libre. Datos similares fueron reportados por Navarro D.[17] en una población de Piura. Sin embargo, esta población refirió consumir bebidas alcohólicas de forma ocasional (49,8%), pero la mayoría se preocupa por realizarse un examen médico periódico en un establecimiento de salud (79,6%). Otro estudio en Perú demostró que la inactividad física está presente en la mayoría de las personas (93,7%) de sectores urbanos y semiurbanos[23]. Mientras que otro estudio en pobladores rurales en China, reportó que más de la mitad se abstuvo de consumir alcohol (86,2%), pero la cuarta parte (25,5%) hizo actividad física al aire libre[24]. Un estilo de vida más proactivo, es decir, con la presencia de ejercicio físico de manera regular, con una mejor calidad de sueño, se relacionaría con mejoras en la percepción de la propia salud[25].
Referente a la alimentación, casi la mayoría refirió consumir fideos a diario, pan y cereales. Cerca de la mitad de adultos reportó consumir carne tres o más veces a la semana y una cuarta parte de los encuestados dijo no consumir frituras. Nuestros datos difieren con un estudio realizado en la población de Piura[17] donde más de la mitad (66,8%) señaló consumir frutas diariamente. Además, el 38,4% consumió pescado tres o más veces por semana, el 57% dijo consumir dulces y gaseosas menos de una vez por semana. Otro estudio similar en pobladores de Trujillo[14] reportó que la mayoría (99%) consume frutas y verduras tres veces por semana. La dieta saludable es un determinante conocido para gozar de buena salud[25].
De acuerdo a los determinantes de apoyo comunitario, más de la mitad de los adultos se atendió en los últimos 12 meses en un puesto de salud de primer nivel. Estos datos difieren a lo reportado por Navarro D.[17] y Flores B.[14], donde la mayoría de los encuestados refirieron haberse atendido en el último año en un centro de salud. Nuestros resultados representan un indicador que señala que al menos parte de la población de estudio busca ser atendido por especialistas de salud, junto con recibir conocimientos y actividades preventivo-promocionales para su salud. En cuanto a la distancia de la vivienda y el establecimiento de salud, un poco menos de la mitad de los participantes mencionó que vive a regular distancia, resultado similar al de Flores B.[14], pero difiere al reportado por Navarro D.[17], quien refiere que el lugar de atención se ubica muy cerca de sus casas (78%). Es una fortaleza vivir cerca al establecimiento de salud, dado que, de presentarse alguna emergencia, los pacientes llegarían rápidamente para ser atendidos por un especialista sanitario. Por otro lado, gozaría de la atención y actividades preventivas ofrecidas por el establecimiento.
En relación al seguro de salud, la mayoría de los adultos cuenta con Seguro Integral de Salud del Ministerio de Salud. Estos datos son similares a los reportados por Flores B.[14] y Navarro D.[17]. Las políticas actuales del gobierno peruano respecto del aseguramiento universal de la población peruana es un factor que promueve la atención sanitaria gratuita[26]. En cuanto al tiempo de espera para la atención, un poco menos de la mitad de los participantes mencionó que el tiempo de espera es regular, así como la calidad de atención. Un estudio hecho en Piura[17] reportó resultados similares, mientras que otro estudio realizado en Trujillo[14] difiere con nuestros resultados, pues menciona que los participantes consideran el tiempo de espera muy largo (46%). Sin embargo, la calidad de atención fue buena (61%; n = 83). Pero la mayoría de los encuestados refirió no recibir ningún tipo de apoyo social organizado, mientras que, los pobladores de zonas más pobres en China estaban respaldados por el apoyo social (48%), significando mejor salud[24] y aunque cada persona es responsable de garantizarse los medios y las formas de obtener servicios de salud de calidad que le permitan obtener mejores condiciones de vida. En muchos casos, las barreras al disfrute de buena salud van más allá de las disposiciones y capacidades individuales[21].
Una de las fortalezas del presente estudio, es haber incluido resultados de una gran muestra de hombres y mujeres. Consideramos que nuestros hallazgos permiten visibilizar la magnitud del problema y es un precedente para futuras investigaciones que evalúen adultos mayores con características similares y el desarrollo de la causalidad entre otras variables.
La principal limitación del presente estudio es haber trabajado solo con las redes de salud que pertenecen al Ministerio de Salud del Perú, y no se incluyó otros establecimientos de salud. Junto con lo anterior, y a pesar que se realizó un muestreo probabilístico, cabe la posibilidad de que nuestro estudio no sea representativo hacia toda la población de la ciudad de Chimbote. Además, el sesgo del recuerdo debido al autorreporte por parte de los participantes. Sin embargo, se procuró de forma permanente corroborar la información.
Conclusiones
Nuestro estudio mostró que la mayoría de las personas analizadas culminó estudios secundarios, pero este nivel educativo alcanzado fue insuficiente para el acceso a mejores escalas salariales. Asimismo, gran parte de la población estudiada cuenta con vivienda propia y con los servicios básicos (luz, agua y desagüe), pero estas familias viven en hacinamiento (más de tres personas por habitación). Según lo reportado, se debe al escaso ingreso económico que no les permite vivir ni mejorar la distribución de espacios[20].
También se encontró que existe un bajo consumo de bebidas alcohólicas y tabaco, pero la inactividad física ligada al sedentarismo fue superior, así como la alimentación elevada en carbohidratos que los expone a enfermedades infecciosas y/o crónicas. Pese a ello, estas personas no acuden a evaluaciones médicas periódicas. La salud y la pobreza se modifican de acuerdo a las condiciones sanitarias y económicas de la población. Frente a ello, es necesario que el sector educación y salud estén involucrados, a fin de lograr eficientes políticas educacionales y sanitarias para reducir los problemas de salud[2].
Notas
Contribuciones de autoría
MAVR, EZL y JBP plantearon la idea de estudio; todos los autores participaron en la recolección de datos, interpretación de resultados, redacción del manuscrito y aprobación de la versión final.
Conflictos de interés
Los autores declaran no tener conflictos de interés con respecto al presente artículo.
Fuentes de financiamiento
El presente estudio está financiado por la Universidad Católica Los Ángeles de Chimbote.

