Notas metodológicas
← vista completaPublicado el 5 de enero de 2021 | http://doi.org/10.5867/medwave.2021.01.8090
Revisiones rápidas: definiciones y usos
Rapid reviews: definitions and uses
Resumen
Este artículo es el primero de una serie metodológica colaborativa de revisiones narrativas sobre temáticas de bioestadística y epidemiología clínica. El objetivo de esta revisión es presentar las revisiones rápidas, compararlas con las revisiones sistemáticas y mencionar su uso actual. Las revisiones rápidas utilizan una metodología similar a las revisiones sistemáticas, pero mediante atajos utilizados en su desarrollo; permiten alcanzar respuestas en menos de seis meses y con menos recursos, por lo que son utilizadas por tomadores de decisiones tanto en América como Europa. No existe consenso sobre cuáles atajos tienen menor impacto en la confiabilidad de las conclusiones, por lo que las revisiones rápidas son heterogéneas entre sí. Los consumidores deben identificar estos atajos en la metodología y ser precavidos en la interpretación de las conclusiones, aunque generalmente alcanzan respuestas concordantes con las obtenidas mediante una revisión sistemática tradicional. Su principal atractivo es ajustarse a las necesidades de los tomadores de decisiones en salud, cuando el contexto exige respuestas en plazos de tiempo acotados.
Ideas clave
- Las revisiones rápidas surgen como una forma de sintetizar el conocimiento que contempla los componentes simplificados de una revisión sistemática, para producir información en menor tiempo y con menos recursos para orientar los tomadores de decisiones.
- Debido a la alta heterogeneidad de este tipo de revisiones, faltan estudios que evalúen adecuadamente qué partes del proceso de una revisión sistemática se pueden simplificar con menor impacto en sus conclusiones.
- Este trabajo presenta la utilidad de las revisiones rápidas como herramienta para sintetizar la evidencia con menos recursos en un lenguaje amigable, orientado a la formación de estudiantes de pre y posgrado.
Introducción
Las revisiones sistemáticas son consideradas actualmente la mejor opción para sustentar decisiones informadas[1], tanto a clínicos como a aquellos que toman decisiones en salud, debido a su capacidad de sintetizar la evidencia científica relevante sobre un tema, con altos estándares metodológicos en su proceso. Sin embargo, el proceso es costoso y largo, pudiendo tomar su realización hasta más de tres años[2], lo que en ocasiones demora de sobremanera las respuestas a las preguntas planteadas. Esto puede afectar la toma de decisiones clínicas y el diseño de políticas en salud.
Las revisiones rápidas surgen como una forma de sintetizar el conocimiento que contempla los componentes de una revisión sistemática, pero simplificados u omitidos para producir información en menor tiempo y con menos recursos para satisfacer las necesidades de los tomadores de decisiones[3],[4]. Estos procesos simplificados son conocidos como “atajos” y, si bien podrían disminuir la confiabilidad en las conclusiones[5], hay estudios que concluyen que, sobre todo en intervenciones terapéuticas, no cambian marcadamente el resultado[6],[7].
Sin una definición consensuada, las revisiones rápidas se presentan como un conjunto heterogéneo de productos sin una estandarización en su producción[8], ni conocimiento acabado sobre cuáles serían los “atajos” que provocan menor impacto en su calidad[9],. Existe acuerdo en contemplar un plazo entre 1 y 6 meses para su realización dependiendo de las necesidades de los tomadores de decisiones[10]. Ello ha aumentado su demanda, llevando a instituciones como la Organización Mundial de la Salud (OMS) a utilizar estos métodos para la confección de guías en un menor plazo de tiempo[11],[12]. En esta misma línea, Cochrane fundó un grupo de trabajo sobre revisiones rápidas en 2015.
Este artículo corresponde al primero de una serie metodológica de revisiones narrativas acerca de tópicos generales en bioestadística y epidemiología clínica, las que exploran y resumen en un lenguaje amigable, artículos publicados disponibles en las principales bases de datos y textos de consulta especializados. La serie está orientada a la formación de estudiantes de pre y posgrado. Es realizada por la Cátedra de Medicina Basada en la Evidencia de la Escuela de Medicina de la Universidad de Valparaíso, Chile, en colaboración con el Departamento de Investigación del Instituto Universitario del Hospital Italiano de Buenos Aires, Argentina, y el Centro Evidencia UC. El objetivo de este artículo es presentar el concepto de revisiones rápidas, sus similitudes y diferencias con las revisiones sistemáticas y su utilidad como herramienta para sintetizar la evidencia con menos recursos.
Conceptos generales de la revisión sistemática
La revisión sistemática es el mejor diseño de síntesis de evidencia para alcanzar conclusiones confiables[13], siendo particularmente valiosa al momento de diseñar políticas públicas o guías de práctica clínica[14].
Una revisión sistemática de buena calidad debe tener un protocolo explícito, establecido a priori y que, idealmente, se mantiene sin modificaciones durante el proceso, lo que permitirá a evaluadores reproducir el proceso y hacer un análisis crítico de su metodología[5]. Este protocolo debiese ser inscrito en una base de datos de registro especializada, como por ejemplo International Prospective Register Of Systematic Reviews, PROSPERO, o publicarse en revistas científicas.
La pregunta de investigación planteada debe estar bien estructurada (en formato Participants, Interventions, Comparisons, Outcomes, PICO)[15], ser clínicamente relevante y con una amplitud y/o complejidad a discreción de los autores según las necesidades de las partes interesadas[8]. La búsqueda bibliográfica debe ser exhaustiva y sensible, abarcando múltiples bases de datos electrónicas con estudios publicados, documentos no publicados en canales convencionales (literatura gris), publicaciones de revistas o sociedades científicas, e incluso en ocasiones incluir el contacto con expertos en búsqueda de estudios en proceso que no estén registrados. Esta búsqueda demanda muchos recursos para acceder a los estudios elegibles[9].
El proceso de inclusión y exclusión de los estudios y el análisis de riesgo de sesgo contempla al menos dos revisores independientes[15]. Por lo tanto, el tiempo que tome completar el proceso depende en gran medida de la cantidad de evidencia que arroje la búsqueda, los estudios seleccionados por los revisores que requieren evaluación a texto completo y de la extracción de sus resultados.
Podemos esquematizar la realización en los siguientes pasos (Figura 1):
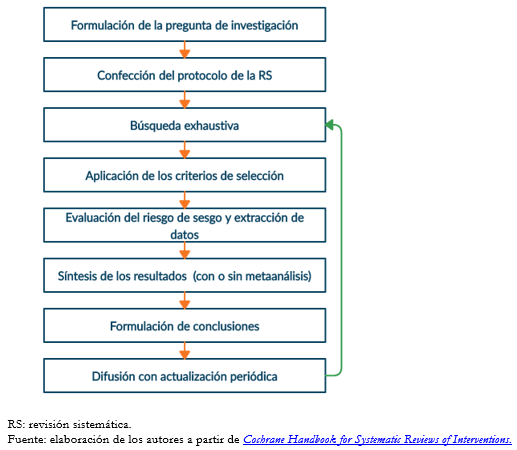 Tamaño completo
Tamaño completo Queda entonces conocer qué etapas de una revisión sistemática se pueden simplificar y qué implicancias tienen estas simplificaciones en las conclusiones obtenidas por la revisión[13].
Revisiones rápidas
Actualmente, las revisiones rápidas se utilizan para la confección de políticas públicas en salud en países de América y Europa[5],[16]: los informes de evaluación de tecnología sanitaria realizados en latinoamérica son un ejemplo del auge de este tipo de diseño metodológico. Localmente, destaca la iniciativa de Epistemonikos[17] y L OVE (Living OVerview of Evidence)[18],[19] como facilitadores en la búsqueda de este tipo de revisiones[20]. La capacidad de balancear un proceso abreviado, con un rigor metodológico suficiente, hace a las revisiones rápidas una alternativa real de síntesis de evidencia con información de moderada confianza, en plazos de tiempo acotados[10].
A pesar de esto, los autores deben explicitar las limitaciones metodológicas, y el consiguiente riesgo de sesgo propio del diseño[21],[22]. Por otro lado, los usuarios/lectores de estas síntesis deben ser precavidos al momento de analizar la metodología, y los atajos empleados por los revisores, teniendo en cuenta la confianza en las conclusiones que tienen los autores[6].
Debido a la falta de consenso en su definición, son difíciles de encontrar si no lo explicitan en su título y, por ello, la mayoría de ellas se concentra en la literatura gris[5]. Muchas no son publicadas debido a que las encargan directamente los interesados[5], como ministerios de salud o creadores de políticas públicas.
Los atajos empleados por los autores de las distintas revisiones publicadas son inconsistentes, lo que provoca una alta heterogeneidad en este tipo de síntesis de evidencia. Faltan estudios que evalúen adecuadamente qué partes del proceso de una revisión sistemática se pueden simplificar con menor impacto en sus conclusiones[10]. Sin embargo, cuando una revisión rápida incluye al menos 10 estudios tiene menos probabilidades de llevar a conclusiones diferentes a las emanadas de una revisión sistemática tradicional[6].
Como mencionamos, los métodos de una revisión rápida no están estandarizados. Sin embargo, el Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA), un proyecto que busca estandarizar el reporte de las revisiones sistemáticas, se encuentra en actualización para incorporar formatos como el de las revisiones rápidas desde 2018[23].
Registro de la revisión
Si bien bases de datos como PROSPERO aceptan el registro de protocolos de revisiones rápidas, no todas consideran este paso en su desarrollo[21]. No registrar ni publicar el protocolo aumenta el riesgo de sesgo de reporte selectivo[15].
Pregunta de investigación
Una revisión rápida incluye una pregunta con una estructura Participants, Interventions, Comparisons, Outcomes, pero debería realizarse para responder preguntas específicas, más que como una alternativa rápida a una revisión sistemática[24]. Su pregunta debe ser acotada o de alcance reducido considerando los objetivos de las partes interesadas[10]. El tiempo que tome su realización estará determinado en gran parte por este ítem. Algunos tópicos que suelen estar fuera del alcance de las revisiones rápidas son intervenciones múltiples o complejas[8].
Búsqueda bibliográfica
Inicialmente, los autores pueden buscar una revisión sistemática de alta calidad para evitar la duplicación de esfuerzos y redirigirlos a una actualización rápida de la misma; por ejemplo, corriendo una búsqueda desde la fecha de búsqueda de la revisión, pero en un número reducido de bases de datos. Esta búsqueda abreviada se puede realizar en una de las principales fuentes bibliográficas electrónicas, siendo PubMed/MEDLINE la más utilizada[25] dado que incluye, en promedio, más del 80% de los estudios habitualmente incluidos en revisiones sistemáticas[6] Otros “atajos” empleados para simplificar la búsqueda incluyen:
- Eliminar la búsqueda manual de evidencia (fuentes no electrónicas) y de literatura gris[5].
- Limitar la búsqueda a estudios en lenguajes específicos[5],[26], por ejemplo, sólo estudios en inglés.
- Limitar la fecha de publicación de los estudios a incluir[5], por ejemplo, búsqueda de publicaciones en los últimos 10 años. Este atajo es el más utilizado por autores de revisiones rápidas publicadas[21].
- Limitar el diseño de los estudios elegibles, por ejemplo, filtrar la búsqueda sólo para ensayos clínicos aleatorizados[8].
Estos atajos pueden conllevar un mayor riesgo de sesgo de publicación y sesgo de selección[6],[10].
Selección de estudios y extracción de datos
Los autores pueden decidir no realizar la selección y extracción de datos por duplicado[10]. Esta decisión puede agilizar considerablemente la realización de una revisión rápida, sin embargo, ambos pasos tendrán mayor riesgo de error y de sesgo[27],[28],[29]. Otro atajo utilizado en la selección es reducir los desenlaces que se desea evaluar al momento de seleccionar estudios[9], por ejemplo, sólo considerar mortalidad como desenlace relevante. Una desventaja de este atajo es que se pierde la posibilidad de evaluar el reporte selectivo de desenlaces de un estudio primario.
Evaluación de riesgo de sesgo
Algunas revisiones rápidas omiten este proceso como atajo. Sin embargo, no es recomendable debido al alto impacto que tiene en la confiabilidad de las conclusiones[30],[31]. Al no realizar una evaluación crítica de los estudios, se desconoce la calidad de la evidencia sobre la que se basan y formulan las conclusiones[32],[33].
Síntesis de evidencia
Las revisiones rápidas pueden optar por no hacer metanálisis y describir narrativamente los hallazgos cuantitativos. De hecho, más de dos tercios de las revisiones rápidas presentan sus resultados de manera narrativa[21].
Conclusiones de una revisión rápida
Existen pocos estudios que evalúen este tópico[9], por lo que la evidencia disponible es escasa. No obstante, existen estudios que no han encontrado que las conclusiones de una revisión rápida difieran sustancialmente de una revisión sistemática tradicional[5],[24]. Debido a las limitaciones derivadas de los atajos utilizados en el diseño, la fiabilidad en las conclusiones es menor[9], y así deben ser interpretadas por sus consumidores. La fiabilidad también dependerá de la calidad de los estudios incluidos en cada revisión rápida[32],[33].
A continuación, mostramos una tabla comparativa con las principales diferencias entre una revisión sistemática y una revisión rápida (Tabla 1).
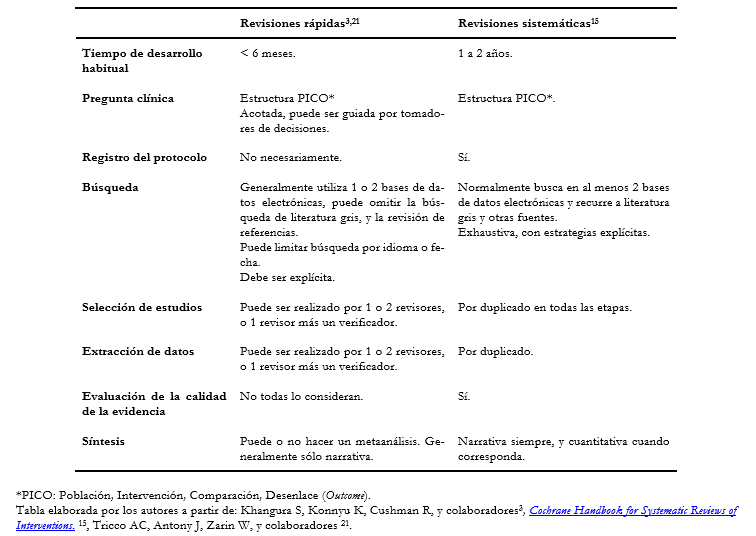 Tamaño completo
Tamaño completo ¿Cuándo es útil una revisión rápida?
Si tenemos en consideración todo lo mencionado en los puntos previos, resulta evidente que el diseño metodológico de las revisiones rápidas no es adecuado en todos los contextos. A continuación, mencionamos algunas circunstancias en que sí lo son:
● Cuando existan restricciones de tiempo para la realización de una síntesis de evidencia, por ejemplo, en contingencias sanitarias como la presentada durante la pandemia de COVID-19[4].
● Cuando existan restricciones de recursos, ya sean económicos o humanos, para llevar a cabo una síntesis de evidencia sobre un tema en específico.
● Centros de salud que evalúan su atención más allá de lo sanitario, por ejemplo, comparar la cantidad de litigios derivados de su atención con las tasas que presentan otros centros locales o internacionales[34].
● Para evaluar nueva evidencia sobre un tema del que existe amplio consenso.
Y en general, en cualquier escenario en que los tomadores de decisiones (clínicos o diseñadores de políticas en salud) puedan actuar fundados en formatos de síntesis de evidencia de menor confiabilidad para responder a los tiempos que imponga el contexto[10].
Algunas de sus limitaciones
Hay que tener en cuenta que una revisión sistemática puede realizarse de manera rápida, manteniendo el rigor metodológico que la caracteriza[35],[36], sin utilizar atajos en su metodología. Esta es una de las principales críticas actuales a la metodología de las revisiones rápidas, ya que hoy existen herramientas tecnológicas que permiten optimizar el recurso humano y agilizar muchos de los procesos de una revisión sistemática[37],[38]. En el caso de tener acceso a los recursos suficientes (humanos, tecnológicos, económicos), lo más adecuado sería no tomar atajos. Otra crítica a las revisiones rápidas es que carecen de la capacidad de abordar preguntas clínicas muy acotadas[30].
Por otro lado, actualmente no se cuenta con herramientas para evaluar de manera estandarizada la calidad metodológica de las revisiones rápidas. En contraste, existen herramientas como Risk of Bias in Systematic Reviews, ROBIS[39], y A Measurement Tool to Assess Systematic Reviews -2, AMSTAR-2[40] que permiten evaluar la calidad metodológica de las revisiones sistemáticas.
Conclusiones
Las revisiones rápidas son síntesis de evidencia abreviadas que contemplan los pasos esenciales de una revisión sistemática tradicional, pero simplifican y/u omiten etapas en su confección para lograr resultados en menos tiempo y a menor costo. No cuentan con una definición exacta y, a la fecha, no existen guías de elaboración ampliamente utilizadas, lo que las hace metodológicamente heterogéneas. Su calidad depende directamente de los atajos que se hayan utilizado y cómo estos atajos pueden afectar los resultados.
Son cada vez más comunes debido a su capacidad de responder preguntas específicas en plazos menores a seis meses. Sin embargo, deben ser interpretadas con cautela debido a las limitaciones derivadas su metodología. Los autores deben explicitar sus métodos, enumerar los atajos utilizados y advertir los posibles sesgos presentes. Con esto en consideración, las revisiones rápidas generalmente llegan a resultados concordantes con los alcanzados por una revisión sistemática tradicional, aunque con una menor confiabilidad.
Las revisiones rápidas están en auge y es de esperar que en los próximos años se estandarice su diseño y representen una de las herramientas más usadas para generar respuestas a preguntas específicas y relevantes en la toma de decisiones en salud.

