Estudios originales
← vista completaPublicado el 30 de septiembre de 2015 | http://doi.org/10.5867/medwave.2015.08.6271
Tuberculosis abdominal, un dilema diagnóstico: reporte de una serie de casos
Abdominal tuberculosis, a diagnostic dilemma: report of a series of cases
Resumen
INTRODUCCIÓN La tuberculosis abdominal es una de las variantes extrapulmonares más frecuentes. Se relaciona a estados de inmunodepresión y, dado su cuadro clínico inespecífico, su diagnóstico es difícil. Nuestro objetivo es presentar una serie de siete casos diagnosticados de tuberculosis abdominal que requirieron cirugía en el Hospital Clínico de la Pontificia Universidad Católica de Chile.
MÉTODOS Se realizó un análisis descriptivo de los siete casos de tuberculosis abdominal operados en nuestro centro entre agosto de 2001 y junio de 2013, caracterizando su presentación clínica y elementos diagnósticos requeridos.
RESULTADOS Cuatro hombres y tres mujeres (entre 29 y 68 años) fueron diagnosticados y operados de tuberculosis abdominal: tres en su forma peritoneal, dos ganglionar y dos intestinal. En tres casos la tuberculosis abdominal se asoció a inmunosupresión (VIH y artritis reumatoide en tratamiento) y en seis casos se presentó con síndrome consuntivo de al menos un mes de evolución. Tres pacientes tuvieron una presentación aguda con signos de obstrucción intestinal. El diagnóstico fue realizado mediante biopsia quirúrgica. Los siete pacientes fueron intervenidos quirúrgicamente, tres de ellos requirieron resección intestinal en el contexto de obstrucción intestinal.
CONCLUSIÓN La tuberculosis abdominal requiere de un alto índice de sospecha, principalmente en población de riesgo, para un diagnóstico oportuno.
Introducción
En Chile la morbilidad por tuberculosis ha disminuido considerablemente en las últimas décadas, de 52,2 por 100 000 habitantes en el año 1989 a 18,4 por 100 000 en 2003. La tasa de mortalidad ha descendido de igual manera, siendo 220,8 por 100 000 habitantes en 1950 y dos por 100 000 habitantes en 2002 [1].
El compromiso pulmonar de la tuberculosis es el más frecuente, el extrapulmonar es reportado entre 15 y 20% de los casos, y se ha hecho proporcionalmente más habitual debido a su asociación con estados de inmunodepresión [2]. En los pacientes infectados con VIH la variante extrapulmonar puede llegar hasta 50 o 70% [3],[4], predominando las formas diseminadas y atípicas, con menor frecuencia de cavitación y formación de granulomas.
El abdomen es la segunda ubicación más frecuente de la tuberculosis extrapulmonar, después de la vía urinaria [5]. La tuberculosis adominal puede presentarse en concomitancia con un foco pulmonar o ganglionar, o bien de manera aislada. Se ha reportado que entre 15 y 20% de los pacientes con tuberculosis abdominal tienen un foco pulmonar activo [5]. A su vez, entre 50 y 90% de los pacientes con foco pulmonar activo tienen algún grado de compromiso gastrointestinal, lo que se explicaría por la carga de microorganismos deglutidos [4],[5],[6].
La tuberculosis abdominal tiene un curso insidioso y un cuadro clínico inespecífico, razón por la cual su diagnóstico es difícil [7],[8],[9],[10],[11],[12]. La comprobación etiológica de la tuberculosis abdominal requiere del estudio histopatológico y bacteriológico, por lo que la endoscopía y la laparoscopía juegan un rol clave para la toma de muestras para biopsia [4],[7],[13],[14],[15].
El objetivo de este trabajo es realizar una descripción de una serie de casos de tuberculosis abdominal, operados en el Hospital Clínico de la Pontificia Universidad Católica de Chile.
Métodos
Se revisaron en forma retrospectiva los registros clínicos de pacientes intervenidos por tuberculosis abdominal, en el Servicio de Cirugía Digestiva del Hospital Clínico de la Pontificia Universidad Católica de Chile, entre agosto de 2001 y junio de 2013.
El análisis de las biopsias contó con estudios histopatológico; histoquímico con tinción de Ziehl-Neelsen para bacilos resistentes al ácido y al alcohol; y de biología molecular tuberculosis-632 con reacción en cadena de la polimerasa (PCR), para detectar la presencia de Mycobacterium tuberculosis por amplificación en duplicado de las secuencias IS6110, con control positivo interno y negativo externo.
Resultados
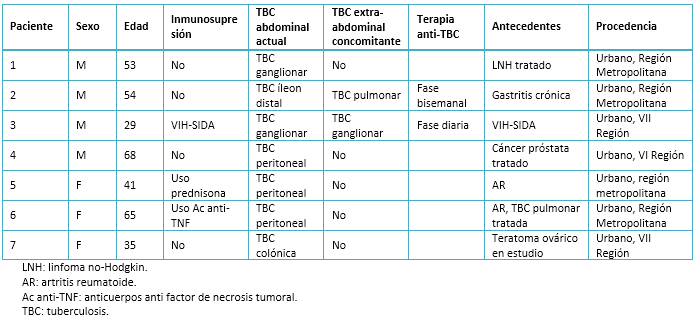
La serie consta de siete pacientes que fueron intervenidos en nuestro centro, cuyo diagnóstico postoperatorio fue de tuberculosis abdominal: tres mujeres y cuatro hombres. El rango de edad fue entre 29 y 58 años. En cuanto a la ubicación, tres pacientes presentaron tuberculosis peritoneal, dos tuberculosis ganglionar y dos tuberculosis intestinal. Dos de ellos estaban en tratamiento por tuberculosis extraabdominal al momento de presentar síntomas abdominales (Tabla 1). Un paciente, sin tuberculosis concomitante, tenía historia antigua de tuberculosis pulmonar tratada con manejo médico y quirúrgico (neumonectomía) hace más de 30 años. Sólo tres pacientes de la serie cursaban con inmunosupresión (terapia inmunosupresora o VIH). La terapia inmunosupresora consistía en prednisona o anticuerpos anti factor de necrosis tumoral como manejo crónico de artritis reumatoide. El paciente con VIH, en tratamiento por tuberculosis ganglionar extraabdominal concomitante, se encontraba en etapa SIDA a pesar de terapia antirretroviral.
 Tamaño completo
Tamaño completo Con respecto al cuadro clínico, astenia y baja de peso estuvo presente en cinco pacientes, aquéllos sin esta clínica correspondían a los con tratamiento anti tuberculosis por tuberculosis concomitante. El dolor abdominal se manifestó en cuatro de siete pacientes, tres de los cuales presentaron irritación peritoneal franca asociada a fiebre. Los casos sin dolor abdominal cursaron cuadros larvados, uno con fiebre, baja de peso y sudoración nocturna, y los otros dos con ascitis asociada a síndrome consuntivo. La sintomatología abdominal se relacionó con la presencia de una complicación aguda de la tuberculosis abdominal: perforación intestinal, fístula cecal, peritonitis tuberculosa y obstrucción intestinal.
Todos los pacientes fueron estudiados con laboratorio básico el que resultó inespecífico, evidenciando y orientando el manejo en los casos con complicación aguda subyacente. A todos se les realizó tomografía axial computarizada de abdomen y pelvis con contraste, el que sugirió el diagnóstico de tuberculosis en cuatro casos, tres de ellos con engrosamiento parietal intestinal sugerente y el otro con adenopatías retroperitoneales y fístula cecal en el contexto de tuberculosis ganglionar en tratamiento. Se realizó colonoscopía en tres casos, evidenciando alteraciones (aftas y úlceras) en un paciente cuya biopsia sólo evidenció colitis inespecífica.
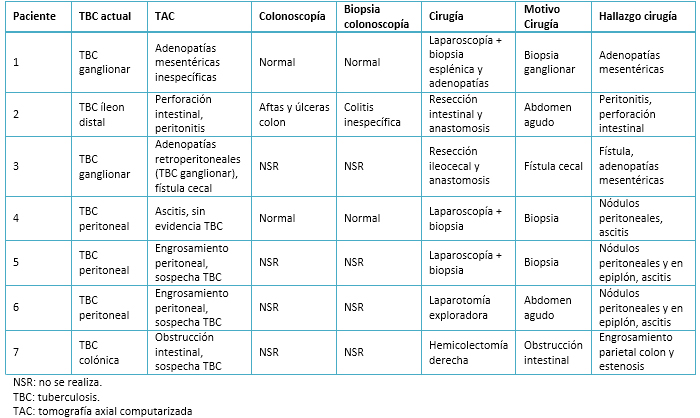
Los siete pacientes fueron llevados a pabellón y en todos ellos se obtuvieron muestras para estudio anatomopatológico. Los detalles de las intervenciones realizadas se presentan en la Tabla 2.
 Tamaño completo
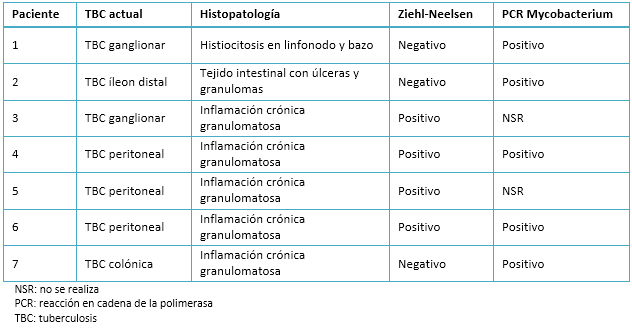
Tamaño completo Entre los hallazgos intraoperatorios destaca la presencia de nódulos peritoneales, implantes en epiplón y ascitis en los casos de tuberculosis peritoneal; y adenopatías asociadas o no a engrosamiento parietal intestinal en los casos de tuberculosis ganglionar e intestinal. El resumen del estudio anatomopatológico, se expone en la Tabla 3.
 Tamaño completo
Tamaño completo Discusión
La tuberculosis abdominal es un reto diagnóstico, requiere de un alto índice de sospecha y un estudio secuencial y estandarizado. Existen varios elementos que se hacen comunes en las presentaciones abdominales que deben ser tenidos en cuenta para orientar el estudio [3],[9],[14].
La población mayoritariamente comprometida es la inmunodeprimida: VIH (+), con terapia inmunosupresora y estados caquécticos. Si bien es cierto que el estado de inmunosupresión debe ser un elemento de sospecha de tuberculosis en todas sus formas, se deben considerar particularmente las presentaciones atípicas en este contexto [5],[6],[16],[17]. En nuestra serie, casi la mitad de los casos estaban asociados a un contexto de inmunosupresión; la mayoría presentaba un cuadro consuntivo además del evento agudo que constituía el motivo de consulta.
Los exámenes de laboratorio y de imágenes son de gran importancia para evaluar el contexto del paciente, las eventuales complicaciones presentes, descartar otras patologías y orientar el estudio. Las imágenes de mayor resolución, como la tomografía axial computarizada, pueden evidenciar hallazgos compatibles con tuberculosis que orienten el adecuado estudio histopatológico [1],[3],[4] y permiten el diagnóstico de las complicaciones asociadas. En nuestra serie, la tomografía axial computarizada evidenció elementos sugerentes de tuberculosis abdominal en cuatro de los pacientes.
Con respecto al estudio endoscópico, se han descrito hallazgos sugerentes de enteritis tuberculosa, en los que el estudio anatomopatológico puede confirmar el diagnóstico en un número importante de casos [4],[13],[15],[18]. En otros, será difícil distinguir de otras causas de inflamación crónica intestinal, como la enfermedad de Crohn [19],[20],[21],[22]. En nuestra experiencia, si bien la colonoscopía no fue realizada en todos los casos, cuando se realizó, permitió orientar la conducta terapéutica.
La confirmación etiológica debe considerar además de los análisis microbiológicos habituales, el análisis molecular que debe incluirse en el estudio anatomopatológico en los casos no concluyentes [4],[6],[18]. En esta serie, la reacción en cadena de la polimerasa para Mycobacterium fue necesaria para la confirmación diagnóstica en cinco pacientes. En dos casos el diagnóstico se realizó exclusivamente fundado en este examen.
Es importante considerar que existe un porcentaje de pacientes en quienes no se logrará confirmar el diagnóstico de tuberculosis, por lo que con una alta sospecha clínica se puede iniciar tratamiento y valorar la respuesta clínica (“prueba terapéutica”) [1],[23],[24]. Esta situación debe contar con adecuados elementos que permitan evaluar el seguimiento. En este sentido, los parámetros de laboratorio y principalmente los de imágenes y endoscópicos juegan un rol importante [5],[6]. En nuestra serie la exploración quirúrgica fue una herramienta adecuada para la toma de muestras para el análisis histopatológico y molecular, siendo clave en la confirmación de la tuberculosis.
Conclusiones
La tuberculosis abdominal requiere un alto índice de sospecha para un diagnóstico oportuno, en especial en población de riesgo. Un elemento importante es el contexto clínico en que se presenta, asociado a un curso insidioso, progresivo y consuntivo [24],[25]. La tomografía axial computarizada y la adecuada toma de muestras para biopsias son factores claves para la confirmación diagnóstica.
Notas
Aspectos éticos
El manuscrito original fue evaluado por el editor de ética de la Revista. Se considera que, dado que los casos fueron analizados retrospectivamente a partir de fichas clínicas, las identidades de los pacientes no son discernibles ni trazables a partir de la información entregada en el artículo. Este hecho resguarda la confidencialidad de los datos sensibles de los pacientes incluidos, que no sufren ningún tipo de intervención física ni psíquica como parte específica del estudio. En consecuencia, no se vulneran principios básicos de la ética de la investigación.
Declaración de conflictos de intereses
Los autores han completado el formulario de declaración de conflictos de intereses del ICMJE, y declaran no haber recibido financiamiento para la realización del estudio y no tener conflictos de intereses asociados al tema abordado. Los formularios pueden solicitarse al autor responsable o a la dirección editorial de la Revista.

