Revisión sistemática
← vista completaPublicado el 28 de septiembre de 2018 | http://doi.org/10.5867/medwave.2018.05.7265
Efectividad de las técnicas de movilización articular sobre el rango de movimiento de pacientes adultos con capsulitis adhesiva primaria de hombro: revisión sistemática y metanálisis
The effectiveness of joint mobilization techniques for range of motion in adult patients with primary adhesive capsulitis of the shoulder: a systematic review and meta-analysis
Resumen
OBJETIVO Determinar la efectividad de las técnicas de movilización articular en el rango de movimiento en pacientes adultos con capsulitis adhesiva primaria de hombro.
MÉTODO Revisión sistemática con metanálisis. La búsqueda fue realizada en las bases de datos MEDLINE/PubMed, PEDro, CENTRAL, LILACS, EMBASE, CINAHL, Scopus y Web of Science. Los criterios de elegibilidad fueron estudios que utilizaran una técnica de movilización articular oscilatoria y/o mantenida aplicada, sola o adicionada, a un programa de tratamiento en pacientes con capsulitis adhesiva primaria, en cualquier estadio. La selección de estudios y la extracción de datos fueron realizadas por dos autores de forma independiente. El riesgo de sesgo se evaluó según la herramienta propuesta por Cochrane.
RESULTADOS Se incluyeron 14 estudios con variados riesgos de sesgo. La movilización posterior versus otra técnica articular no presenta diferencia de media significativa (- 0,95 grados; intervalo de confianza de 95%; - 5,93 a 4,02), mientras que comparada con un grupo control la diferencia es de 26,80 grados (intervalo de confianza 95%; 22,71 a 30,89), además cuando se aplica un conjunto de técnicas articulares versus un grupo control, para la abducción la diferencia es de 20,14 grados (intervalo de confianza 95%; 10,22 a 30,05). En ambos casos, los resultados son estadísticamente significativos y se aprecia un tamaño de efecto moderado.
CONCLUSIONES La evidencia científica no es concluyente acerca de la efectividad de la movilización articular, dada la heterogeneidad en la metodología y sesgo de los artículos incluidos en esta revisión. Al compararla con tratamientos que no incluyen terapia manual, parecieran favorecer la mejoría del rango de movimiento y reducción del dolor, en pacientes con capsulitis adhesiva primaria de hombro.
|
Ideas clave
|
Introducción
La capsulitis adhesiva es una condición musculoesquelética común, caracterizada por dolor de inicio espontáneo asociado a una pérdida progresiva del movimiento glenohumeral de etiología desconocida[1]. Neviaser fue el primero en usar el término capsulitis adhesiva, describiéndola como una inflamación crónica de la membrana sinovial con fibrosis de la cápsula articular y adherencias intraarticulares en el hombro[2]. Años más tarde, sería definida por el Consenso de la Sociedad Americana de Cirujanos de Hombro y Codo como “una condición de etiología desconocida, caracterizada por una restricción significativa del rango de movimiento pasivo y activo del hombro que se produce en ausencia de una patología intrínseca conocida”[3]. Zuckerman propuso un esquema de clasificación donde la capsulitis adhesiva primaria o idiopática no está asociada a una condición sistémica o historia de daño, es decir, no existe ningún evento precedente al que se pueda atribuir el cuadro. Desde el punto de vista del diagnóstico, se considera en todos los casos que la etiología asociada o subyacente a esta condición no pueda ser identificada[3],[4].
El conocimiento de la historia natural de la enfermedad es relevante para evaluar la efectividad real de las diferentes modalidades terapéuticas usadas en el manejo clínico de esta patología. En el caso de la capsulitis adhesiva primaria, su naturaleza benigna y curso autolimitado resulta controversial[5],[6],[7],[8],[9]. Codman y Grey, fueron los primeros en afirmar que todos los pacientes con capsulitis adhesiva primaria tienen una recuperación completa del dolor y el rango de movimiento a los dos años de iniciados los síntomas[10],[11]. Sin embargo, estudios prospectivos y de largo plazo han reportado porcentajes variables de pérdida del rango de movimiento, dolor y discapacidad en pacientes con capsulitis adhesiva primaria[6],[12],[13],[14],[15]. En cuanto a las restricciones del movimiento, los autores informan una restricción significativa en el 90% de los pacientes a los siete meses de seguimiento[7], y entre un 30 a un 50% de los pacientes presentan restricción leve y/o moderada en un seguimiento de tres a 10 años[6],[7],[8],[12],[13]. Este antecedente resulta relevante, más aún cuando evidencia de moderada calidad plantea que la teoría de la auto-resolución es cada vez más incierta y que los mejores resultados terapéuticos se obtienen al intervenir en etapas tempranas y no tardías[16].
En este sentido, cabe destacar que los movimientos rotacionales, específicamente la rotación externa, no han mostrado cambios significativos antes de las cuatro semanas de tratamiento fisioterapéutico[17]. Algunas intervenciones terapéuticas como inyección de corticosteroides, diferentes modalidades de electroterapia, distensión artrográfica, tratamiento de puntos gatillo muscular y técnicas de terapia manual, también se han recomendado para la mejoría del rango de movimiento y disminución del dolor[18],[19],[20],[21],[22]. En los últimos años, varios estudios han mostrado resultados beneficiosos utilizando técnicas de terapia manual para corregir los déficits del rango de movimiento rotacional glenohumeral, especialmente la rotación externa[23],[24],[25],[26],[27],[28]. Dichas técnicas han demostrado ser efectivas en el manejo de las restricciones capsulares, específicamente cuando son provistas por un fisioterapeuta[29].
La literatura describe tres tipos de técnicas de movilización articular: oscilatorias, mantenidas y manipulativas. Las técnicas oscilatorias son movimientos pasivos repetitivos de amplitud variada y a baja velocidad[30],[31],[32]. Las movilizaciones mantenidas son un tipo de tracción de amplitud variable y baja velocidad, que disminuyen las fuerzas compresivas intraarticulares y quitan la distensión de los tejidos periarticulares[33]. Estas han sido graduadas de acuerdo con la amplitud del movimiento y el grado de tensión del tejido periarticular[31],[34]. Finalmente, las técnicas de manipulación son aquellas que implican movimientos de alta velocidad y baja amplitud asociados a un thrust en el final del rango de movimiento disponible articular[31].
De lo anteriormente expuesto, nacen nuestras preguntas de investigación: en pacientes con capsulitis adhesiva primaria de hombro ¿las técnicas de movilización articular mantenidas son más efectivas que las oscilatorias para la mejoría del rango de movimiento, dolor y función del hombro?, ¿adicionar técnicas de movilización articular a un programa de tratamiento produce alguna mejoría del rango de movimiento, dolor y función del hombro?
Tratar de dilucidar estas interrogantes fue lo que motivó la realización de la presente revisión sistemática, la que tiene por objetivo principal determinar la efectividad de las técnicas de movilización articular en la mejoría del rango de movimiento, ya sea aplicadas por si solas o adicionadas a un programa de tratamiento. Como objetivos secundarios se pretende determinar el efecto de las técnicas sobre la mejoría de la función y la disminución del dolor, además de la dosificación utilizada.
Métodos
Protocolo
La presente revisión sistemática será reportada según la normativa preferente para revisiones sistemáticas y metanálisis[35]. Cabe mencionar que no se registró el protocolo previo a la realización de la presente revisión.
Criterios de elegibilidad
Para la realización de la revisión sistemática se desarrolló una estrategia de búsqueda en la cual se incluyeron los siguientes criterios de elegibilidad:
- Población: pacientes mayores de 18 años con diagnóstico de capsulitis adhesiva primaria en cualquier estadio, sin distinción de género ni raza.
- Intervención: una técnica de movilización articular oscilatoria y/o mantenida aplicada sola o adicionada a un programa tratamiento.
- Comparación: con otras técnicas de terapia manual, uso de agentes físicos, diferentes modalidades de ejercicio terapéutico o tratamientos farmacológicos.
- Medidas de resultado: artículos que hayan evaluado la efectividad clínica a través del rango de movimiento, la función y el dolor del hombro.
- Tipos de estudios: ensayos clínicos controlados aleatorizados publicados en inglés o español hasta el 16 de julio de 2018.
Criterios de inclusión
- Ensayos clínicos controlados aleatorizados que comparen la efectividad clínica entre dos técnicas de movilización articular aplicadas en pacientes con capsulitis adhesiva primaria.
- Ensayos clínicos controlados aleatorizados que comparen la efectividad clínica de una o más técnicas de movilización articular aplicadas como parte de un programa de tratamiento en pacientes con capsulitis adhesiva primaria.
Criterios de exclusión
- Ensayos clínicos controlado aleatorizados que no describan el tipo de técnica de movilización articular ni especifiquen la dosis utilizada.
- Ensayos clínicos controlados aleatorizados que estudien otras técnicas de movilización articular como movilización con movimiento y/o de manipulación.
Fuentes de información
MEDLINE/PubMed (www.ncbi.nlm.nih.gov/pubmed), PEDro (www.pedro.org.au), CENTRAL (www.cochrane.org), LILACS (www.lilacs.bvsalud.org/es), EMBASE (www.elsevier.com/solutions/embase-biomedical-research echa), CINAHL (www.health.ebsco.com/products/the-cinahl-database echa), Scopus (www.scopus.com/home.uri?zone=header&origin=searchbasic) y Web of Science (www.fecyt.es/es/recurso/web-science), buscando desde el inicio de cada base de datos hasta el 16 de julio de 2018. También se revisaron las listas de referencias de los ensayos incluidos y cualquier artículo de revisión relevante recuperado en la búsqueda electrónica, con el objetivo de identificar cualquier otro ensayo potencialmente relevante. Cabe mencionar que no se realizó una búsqueda de literatura gris en la presente revisión.
Estrategias de búsqueda
Para llevar a cabo la búsqueda en la base de datos MEDLINE/PubMed, se utilizó una estrategia de búsqueda sensible propuesta en el manual de la Colaboración Cochrane[36]. Los términos de búsqueda utilizados en esta revisión fueron obtenidos de MeSH: bursitis, physical therapy modalities y musculoskeletal manipulations. Estos términos se combinaron con los términos de texto libre: frozen shoulder, adhesive capsulitis y manual therapy.
A continuación, se describe el proceso:
- Bursitis[MeSH]
- Frozen shoulder
- Adhesive capsulitis
- #1 OR #2 OR #3
- Physical therapy modalities[MeSH]
- Musculoskeletal manipulations[MeSH]
- Manual iherapy
- #5 OR #6 OR #7
- #4 AND #8
- Randomized controlled trial[pt]
- Controlled clinical trial[pt]
- Randomized[tiab]
- Randomly[tiab]
- Trial[tb]
- Groups[tiab]
- #10 OR #11 OR #12 OR #13 OR #14 OR #15
- Animals[mh] NOT humans[mh]
- #16 NOT #17
- #9 AND #18
Para las bases de datos PEDro, LILACS, CENTRAL, CINAHL, Web of Science, Scopus y EMBASE se realizó la estrategia de búsqueda combinando los términos mencionados previamente en la opción de búsqueda avanzada.
Selección de estudios
Dos de los autores (JZ y FP) realizaron la cadena de búsqueda de forma independiente, revisando el título, resumen y texto completo de los artículos. Solo fueron seleccionados los estudios que cumplieron con los criterios de elegibilidad. Los desacuerdos fueron resueltos en una discusión entre los autores. En caso de persistir el desacuerdo, se consultó a un tercer revisor independiente (CO).
Extracción de datos
La extracción de datos para los ensayos incluidos se llevó a cabo como recomienda el manual de la colaboración Cochrane para revisiones sistemáticas[36]. Dos revisores (JZ y FP), completaron de forma independiente un formulario estandarizado de resumen de datos, especialmente diseñado para esta revisión. Los datos recopilados fueron ingresados en RevMan 5.3 y, en caso de desacuerdo o discrepancia, el artículo fue evaluado por un tercer revisor (HG). Su inclusión final se decidió mediante discusión de los autores.
Evaluación del riesgo de sesgo de los estudios incluidos
Dos revisores (JZ y FP) evaluaron de forma independiente el riesgo de sesgo de los estudios incluidos, utilizando la herramienta de la colaboración Cochrane para el riesgo de sesgo, como se describe en el manual para revisiones sistemáticas[36]. Se consideraron los siguientes dominios:
- Generación de secuencia aleatoria.
- Ocultamiento de la asignación (sesgo de selección).
- Cegamiento de los participantes y el personal (sesgo de realización).
- Cegamiento de la evaluación de resultados (sesgo de detección).
- Datos de resultado incompletos (sesgo de deserción).
- Informe selectivo de los resultados (sesgo de informe).
- Otras fuentes de sesgo, cada uno de estos dominios fue evaluado como “bajo riesgo”, “alto riesgo” o “riesgo poco claro”.
Un estudio clasificado como de alto riesgo no estaría excluido de esta revisión, pero podría degradar nuestra confianza de recomendación. La información obtenida fue utilizada a través de una presentación de análisis múltiples, a partir de todos los estudios obtenidos y que permitían su análisis cuantitativo.
Medidas de resumen
Para la presente revisión se identificaron solo variables continuas (rango de movimiento, escalas dolor y función), por lo que se utilizó como principal medida de resumen la diferencia de medias entre los grupos de intervención con intervalos de confianza de 95%, para así determinar el tamaño del efecto de los resultados. Para llevar a cabo este proceso se registró el valor final y la desviación estándar del resultado de interés, además del número de participantes para cada grupo de tratamiento al final del seguimiento.
Síntesis de resultados
La síntesis de los resultados se realizó mediante metanálisis, los que se llevaron a cabo en el programa RevMan 5.3. En caso de estudios clínicamente homogéneos, se evaluó la heterogeneidad con la prueba estadística de Chi-cuadrado y el test de heterogeneidad I2, consideramos una baja heterogeneidad un valor Chi-cuadrado con un P > 0,1 y el test I2 con un valor menor o igual a un 50%. En este caso se usó un modelo de efecto fijo para el análisis de los datos, con ponderación de varianza inversa. Por el contrario, se ocupó un modelo de efecto aleatorio cuando hubo alta heterogeneidad.
Análisis adicional
Realizamos el metanálisis en función de dos comparaciones. En primer lugar, se agruparon los ensayos clínicos controlados aleatorizados que incluyeron la movilización posterior grado III según Kaltenborn. En segundo lugar, se analizaron los estudios que incluían dentro de su intervención un conjunto de técnicas de movilización articular. En ambas comparaciones se consideró el análisis por subgrupos sobre la base de la comparación con otras técnicas de movilización articular y con un tratamiento convencional que no incluía técnicas de movilización articular.
Resultados
Selección de los estudios
De acuerdo con la estrategia de búsqueda definida, se identificaron 563 registros para los términos y palabras clave, de los cuales 225 se encontraban duplicados. Una vez analizados los títulos y resúmenes de los restantes, solo 25 artículos cumplieron con los criterios de elegibilidad, los cuales fueron revisados a texto completo. Tras el análisis de los criterios de selección, 11 estudios fueron excluidos por distintos criterios, todos ellos expuestos en la Figura 1, y los 14 estudios restantes fueron incluidos en el proceso de síntesis cualitativa[37],[38],[39],[40],[41],[42],[43],[44],[45],[46],[47],[48],[49],[50].
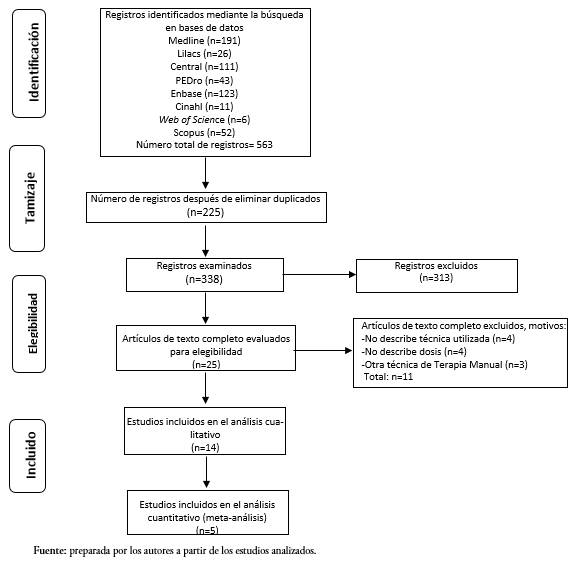 Tamaño completo
Tamaño completo Características de los estudios
Considerando los 14 ensayos clínicos controlados aleatorizados seleccionados, el número total de pacientes fue de 474, con una media de 24 pacientes por estudio y un rango entre 14 y 100 pacientes. El promedio de edad en los estudios fue de 46,9 años, con un rango entre 35 y 70 años.
Posterior al análisis de los artículos incluidos, las técnicas de movilización articular estudiadas se pudieron agrupar sobre la base de dos comparaciones: las que compararon la efectividad clínica entre dos técnicas de movilización articular[38],[39],[40],[41],[42],[44],[45],[50], y aquellas que compararon la efectividad clínica de una o más técnicas de movilización articular aplicadas como parte de un programa de tratamiento[37],[43],[46],[47],[48],[49]. La representación esquemática de estas comparaciones se puede observar en las Figuras 2 y 3.
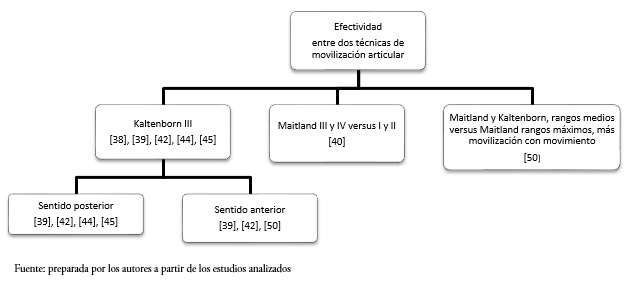 Tamaño completo
Tamaño completo 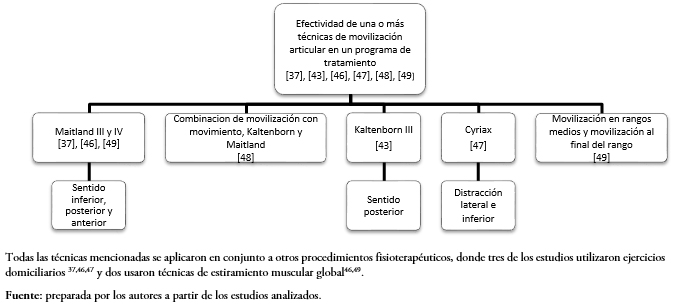 Tamaño completo
Tamaño completo Resultados de los estudios individuales
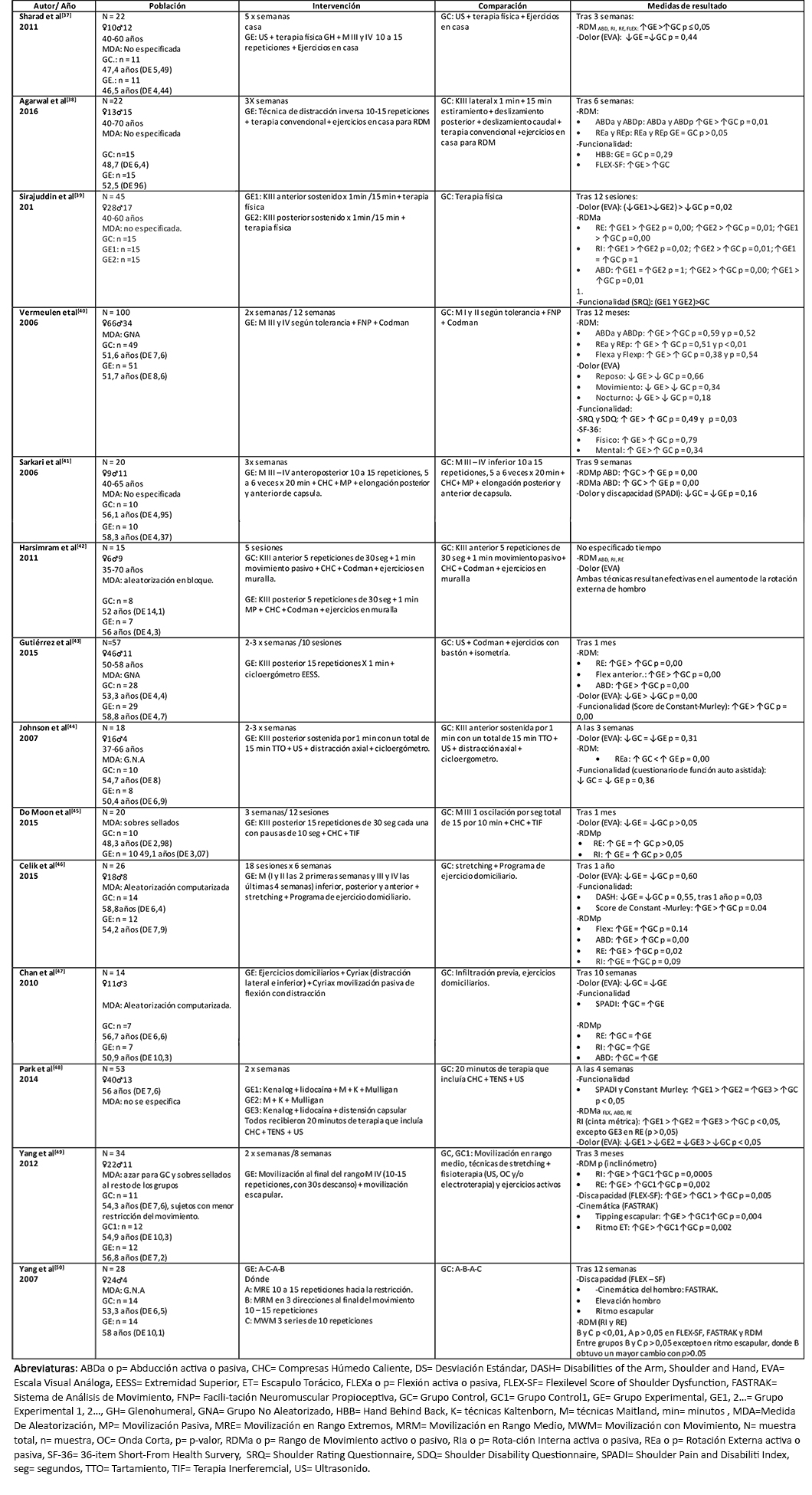
Los resultados de cada uno de los estudios incluidos se encuentran resumidos en la Tabla 1.
Riesgo de sesgo de los estudios
El riesgo de sesgo de los estudios incluidos en esta revisión se presenta en las Figuras 4 y 5. Sólo ocho de los estudios seleccionados informaron los detalles de la asignación al azar[40],[42],[43],[44],[45],[46],[47],[50], y las asignaciones se ocultaron en sólo seis[41],[43],[44],[45],[46],[47]. Dada la naturaleza de las intervenciones estudiadas, el cegamiento de los pacientes y de los tratantes es complejo. En este punto tres estudios fueron calificados de alto riesgo[37],[39],[43] y el resto de riesgo poco claro.
 Tamaño completo
Tamaño completo 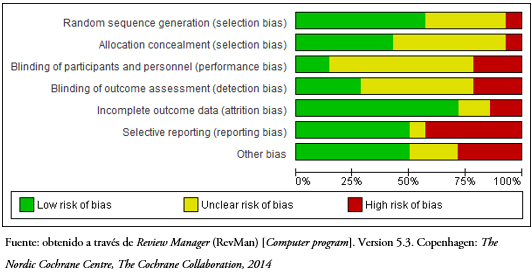 Tamaño completo
Tamaño completo 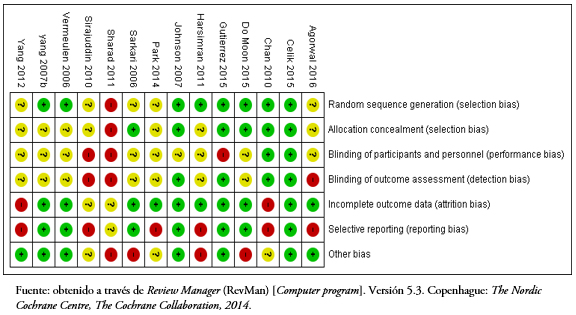 Tamaño completo
Tamaño completo Medidas de resultados de los estudios
Considerando que la restricción del movimiento es un signo patognomónico de la capsulitis adhesiva primaria, para la presente revisión sistemática se consideró como la medida de resultado primaria el rango de movimiento. Todos los estudios incluidos evaluaron el rango de movimiento glenohumeral a través de la goniometría. Se hizo especial énfasis en los movimientos osteokinemáticos de rotación externa y abducción de hombro. Considerando los cambios mal adaptativos y fisiopatológicos de la capsulitis adhesiva primaria sobre las tareas que involucran al complejo articular de hombro[38],[40],[41],[43],[44],[46],[50], se consideró como medidas de resultado secundarias la función del hombro y el dolor. La primera fue valorada en 10 de los estudios, a través de diferentes cuestionarios como Constant-Murley[43],[46], The Disabilities of the Arm, Shoulder and Hand[46], Hand behind back[38], Shoulder Pain and Disability Index[41],[46],[47],[48], entre otros. El dolor fue evaluado a través de la escala visual análoga, en 10 de los 14 estudios[37],[39],[40],[42],[43],[44],[45],[46],[47],[48].
Metanálisis de los resultados
Rango de movimiento glenohumeral
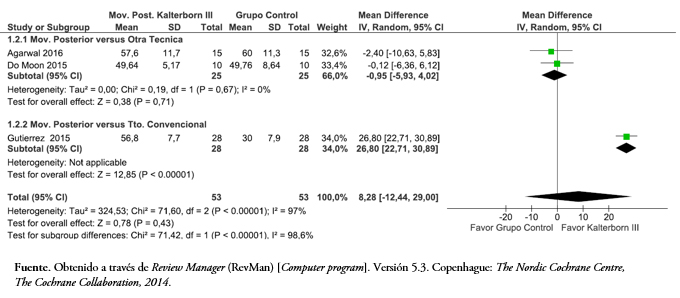
Tres de los artículos incluidos evaluaron la rotación externa glenohumeral[38],[43],[45]. Al comparar la movilización posterior versus otras técnicas articulares, la Figura 6 muestra que los resultados del metanálisis con un modelo de efecto fijo, no hubo una diferencia estadísticamente significativa en el rango de movimiento de rotación externa al final del tratamiento diferencia de media de -0,95 (intervalo de confianza 95%: -5,93 a 4,02; p = 0,71). Al comparar la movilización posterior versus un tratamiento convencional, hubo una diferencia estadísticamente significativa a favor de la movilización posterior, mostrando una diferencia de media de 26,8 grados (intervalo de confianza 95%: 22,71 a 30,89, p = < 0,05). Al considerar el efecto total con una alta heterogeneidad (I2 = 97%) no se pudo establecer una diferencia significativa (p = 0,43) en la rotación externa a favor de la movilización posterior.
 Tamaño completo
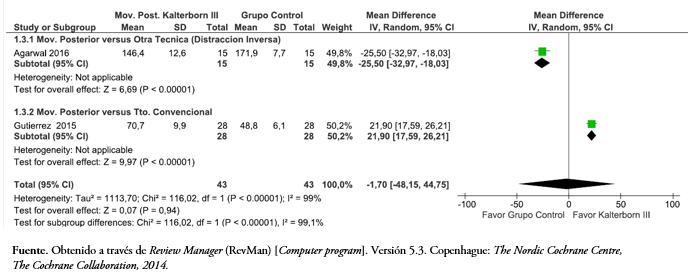
Tamaño completo Dos de los artículos incluidos evaluaron la abducción glenohumeral[38],[43]. Al comparar la movilización posterior versus la distracción inversa, la Figura 7 muestra que hubo una diferencia estadísticamente significativa a favor de la movilización posterior con una diferencia de media de 25,5 grados (intervalo de confianza 95%: 32,97 a 18,03; p < 0,05). Y cuando se comparó con un tratamiento convencional la diferencia de media es de 21,9° (intervalo de confianza 95%: 17,59 a 26,21) a favor de la movilización posterior (p < 0,05). Al considerar el efecto total con un modelo de efecto aleatorio debido a la alta heterogeneidad (I2 = 99%), no se pudo establecer una diferencia significativa (p = 0,94) en la abducción a favor de la movilización posterior.
 Tamaño completo
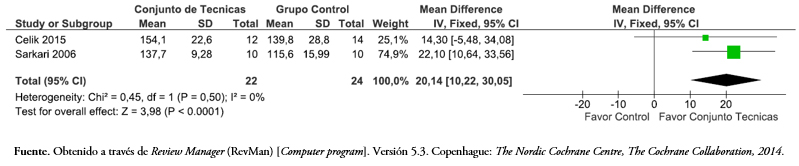
Tamaño completo Al comparar un programa de tratamiento que incluía técnicas de movilización articular versus un grupo control, la Figura 8 muestra que con un modelo de efecto fijo hubo una diferencia estadísticamente significativa de 20,14 grados (intervalo de confianza 95%: 10,64 a 33,56) en el rango de abducción glenohumeral a favor de los estudios que incluían un conjunto de técnicas articulares dentro su intervención en comparación a una intervención control (p < 0,05).
 Tamaño completo
Tamaño completo Función del hombro
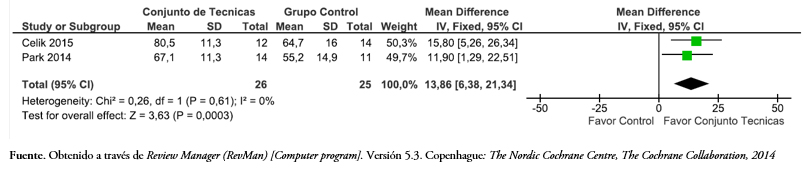
Dos de los artículos incluidos evaluaron la función del hombro con Constant-Murley,[46],[48]. Al comparar un programa de tratamiento que incluía técnicas de movilización articular versus un grupo control, la Figura 9 muestra que con un modelo de efecto fijo hubo una diferencia estadísticamente significativa de 13,86 puntos (intervalo de confianza 95%: 6,38 a 21,34) en el cuestionario de Constant-Murley a favor del uso conjunto de técnicas articulares en comparación con una intervención control (p < 0,05).
 Tamaño completo
Tamaño completo Dolor
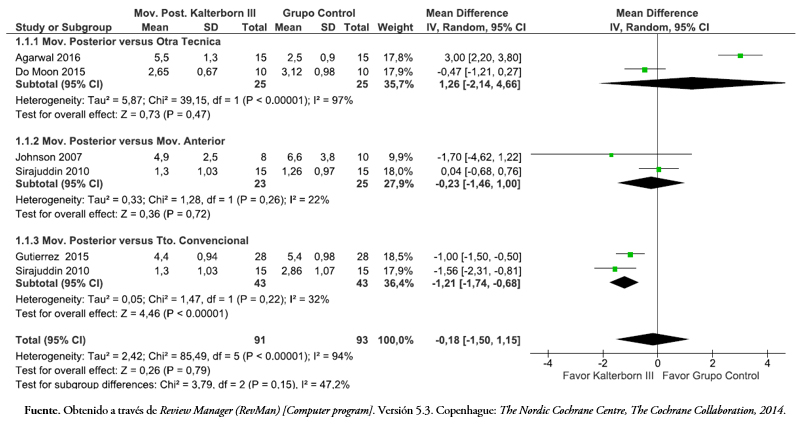
Cinco de los artículos incluidos evaluaron la intensidad del dolor con la escala visual análoga[38],[39],[43],[44],[45]. Al comparar la movilización posterior versus otras técnicas articulares, la Figura 10 muestra que, con un modelo de efecto aleatorio debido a la alta heterogeneidad, existe una diferencia de media de 1,26 centímetros (intervalo de confianza 95%: -2,14 a 4,66), y versus la movilización en sentido anterior es de -0,23 centímetros (intervalo de confianza 95%: -1,46 a 1). En ambas comparaciones, la diferencia no fue estadísticamente significativa (p > 0,05). Por el contrario, cuando se compara con tratamientos que no incluyen técnicas de movilización articular, hubo una diferencia de media de -1,21 centímetros (intervalo de confianza 95%: -1,74 a -0,68) a favor de la movilización posterior (p < 0,05).
 Tamaño completo
Tamaño completo Discusión
La presente revisión sistemática con metanálisis fue realizada sobre la base de 14 ensayos clínicos controlados aleatorizados; y tuvo como objetivo determinar la efectividad de las técnicas de movilización articular aplicadas por sí solas o adicionadas a un programa de tratamiento, en la mejoría del rango de movimiento, función y dolor del hombro. Los resultados muestran que la evidencia no es concluyente en el uso de las técnicas de movilización articular, a pesar de la alta heterogeneidad y riesgo de sesgo de los artículos incluidos, la técnica de Kaltenborn tipo III muestra una tendencia al aumento del rango de rotación externa, abducción y reducción del dolor comparado con un grupo control, aunque sin diferencias estadísticamente significativas. El uso de técnicas de movilización articular adicionadas a un programa de tratamiento muestran resultados estadística y clínicamente significativos para la abducción y la función del hombro cuando se comparan con grupos control, en pacientes con capsulitis adhesiva primaria.
De acuerdo con las revisiones sistemáticas previas que han evaluado la efectividad de las técnicas de movilización articular, los resultados han mostrado un aumento del rango de movimiento y disminución del dolor[22]. Cuando son comparadas con tratamientos convencionales han mostrado cambios de efecto moderado en el rango de movimiento de hombro, especialmente en la rotación externa (p < 0,05), a favor de los deslizamientos en sentido posterior, mostrando un aumento promedio de 26,8 grados (intervalo de confianza de 95%: 22,71 a 30,89). Aunque esta diferencia no ocurre cuando se compara entre dos técnicas de movilización articular (p = 0,71). Considerando la alta heterogeneidad de los estudios, no se puede asegurar que dichos cambios dependan sólo de la técnica, dado que no se ha podido identificar una dosificación única, mínima o necesaria para obtener estas mejorías. Sin embargo, los resultados clínicos más relevantes se obtuvieron en aquellos grupos experimentales que fueron sometidos a técnicas de alto grado de movilización y realizados al final del rango de movimiento disponible[37],[38],[39],[43],[45],[46],[49],[50].
Considerando que la restricción del movimiento rotacional es una de las características más comunes del cuadro, este déficit se puede prolongar más allá de la fase restrictiva y persistir por un período cercano a los dos años, afectando más a la rotación externa que los otros movimientos del hombro[51]. Las restricciones del tejido periarticular[38],[39],[44] junto con la consecuente disfunción de los músculos que estabilizan y movilizan la articulación glenohumeral y escapulotorácica, tienen su origen en el aumento de tensión del intervalo de los rotadores y afecta directamente al complejo articular del hombro en todos sus planos de movimiento[52]. Los cambios en el movimiento de traslación y rotacional de la cabeza humeral determinan un movimiento patomecánico caracterizado por un ascenso y anteriorización de la cabeza humeral con respecto a la superficie glenoidea, afectando su artro y osteokinemática. Lo anterior podría explicar por qué las rotaciones humerales terminan siendo los movimientos más restringidos en conjunto con la abducción, la cual no siempre muestra cambios estadísticamente significativos[39],[40],[47].
Pese al conocimiento existente y a la gran cantidad de ensayos publicados, no ha sido posible identificar ni establecer una dosificación para las técnicas encontradas, ya sea como tratamiento único o como parte de un programa de intervención. Al analizar los tratamientos complementarios a las técnicas aplicadas, un estudio que adicionó técnicas de estiramiento a la movilización articular de Maitland grado IV[46], mostró resultados favorables en ambos grupos, con cambios significativos a favor de la movilización articular en el rango de movimiento, situación similar observada en otro estudio que adicionó técnicas de Kaltenborn III y Maitland III a la aplicación de agentes físicos[45], el cual mostró cambios importantes para los dos grupos pero sin diferencias estadísticamente significativas entre ellos. En aquellos estudios que utilizaron técnicas de Maitland (en todos los grados) asociadas a un programa de ejercicios[46], y técnicas de Maitland III y IV asociadas a estiramientos musculares[41], se mostró mejoría estadísticamente significativa en el rango de movimiento de abducción. Caso similar a lo presentado en un estudio que adicionó la movilización de escápula, y que además de mejorar el rango de movimiento de abducción, también mostró mejoría en la rotación externa glenohumeral[49].
La dosificación de las técnicas utilizadas en los diferentes estudios es variada, observándose que la frecuencia de repeticiones de la misma técnica para completar una sesión de tratamiento, en el caso de las técnicas de Kaltenborn van desde cinco a 15 repeticiones, con un tiempo de mantención de 30 segundos a un minuto[38],[39],[43],[46] mostrando cambios positivos en los grupos intervenidos. El tiempo total de aplicación de la técnica fue de 15 minutos, a excepción de un estudio que consideró 20 minutos[48]. Por otra parte, aquellos que utilizaron las técnicas de Maitland describen 2 a 15 repeticiones, cuya frecuencia fue mencionada en sólo dos estudios[45],[46], las cuales van de una a dos oscilaciones por segundo, con un tiempo total de tratamiento de 20 minutos. Dos de los estudios incluidos, proponen de 10 a 15 repeticiones para las técnicas de movilización articular, pero no indican a qué técnica específica corresponde esta dosificación[38],[50].
Respecto al sentido de la maniobra, los autores que utilizaron técnicas de Kaltenborn la estudiaron en sentido anterior, posterior y lateral[40],[42] demostrando que en aquellos estudios donde se utilizó la técnica en sentido posterior la mejoría del rango de movimiento de rotación externa fue estadísticamente significativa[38],[39],[43],[44]. Esto contrasta con los resultados del estudio de Do Moon y colaboradores[45], donde no se reportaron cambios de importancia estadística al comparar técnicas de Maitland grado III en diferentes sentidos.
Las técnicas de movilización articular de alto grado ya sean de Maitland III - IV como de Kaltenborn grado III, tienen por objetivo restaurar el movimiento artrokinemático a través de la distensión y elongación de las estructuras periarticulares, aumentando la tensión de algunos componentes capsulares y ligamentosos, que estabilizan de manera pasiva la articulación[53]. Este concepto alude a los componentes físicos de la curva longitud - tensión, la cual estudia el comportamiento de un tejido cuando es sometido a una carga, demostrándose que sus propiedades varían progresando desde una fase elástica a una fase plástica, dependiendo directamente del grado, tiempo y dosificación de la movilización, así como de la posición relativa de la articulación[54]. De esto depende la remodelación de fibras colágenas y la modulación de las propiedades del tejido conectivo afectado[50]. Al analizar los estudios que utilizaron técnicas en el rango final y de alto grado de tensión en sentido posterior, todos obtuvieron mejoría en el rango de movimiento, en especial la rotación externa, no así para la abducción (p = 0,94).
Esto postula que la magnitud de la técnica y el sentido en que se realiza, puede determinar un mayor o menor cambio, donde el deslizamiento posterior influye en mayor grado en la restricción capsular, posicionando la articulación y aumentando la elongación de la cápsula articular, lo cual no sería suficiente para mostrar un efecto determinante en el movimiento de abducción, producto de la elevación de la cabeza humeral y el aumento del grosor de las fibras inferiores de la capsula articular[39],[40],[47]. No obstante, las técnicas de movilización articular lograron mejorías significativas en el rango de abducción al ser comparadas con grupos control, logrando un aumento medio de 20,14 grados (intervalo de confianza de 95%: 10,64 a 33,56).
Una de las características a considerar, y que tan sólo un estudio consignó en sus criterios de inclusión[43], fue el grado de irritabilidad de los sujetos. Kelley y colaboradores[1], proponen un sistema de clasificación al respecto, donde un bajo grado de irritabilidad es aquel que presenta dolor menor o igual a tres centímetros según la escala visual análoga, sin dolor nocturno ni en reposo, y con limitación similar del rango de movimiento activo y pasivo. En cambio, un alto grado de irritabilidad implica padecer de dolor mayor o igual a siete centímetros de escala visual análoga principalmente durante la movilidad pasiva, con dolor nocturno y en reposo, asociado a altos niveles de discapacidad, predominando el dolor por sobre la restricción del rango de movimiento.
Este hallazgo se hace relevante al momento de la asignación de un tratamiento, ya que algunos pacientes no tolerarán el grado de movilización si su nivel de irritabilidad es alto, principalmente debido a que la tolerancia a las cargas mecánicas es baja. Dado que las técnicas de alto grado de movilización se basan en un micro daño[37],[43], es probable que al ser realizadas se está influyendo negativamente en la manifestación clínica, reflejado en un aumento del dolor. Su aplicabilidad fase-dependiente podría ser un tema de estudio, avalando su aplicación en fases donde predomina la rigidez por sobre el dolor[40],[43].
Limitaciones
Los ensayos identificados para esta revisión estudiaron una amplia variedad de técnicas de movilización articular, esto sumado al riesgo de sesgo y la heterogeneidad que presentaban limitó la posibilidad de agrupar una mayor cantidad de resultados. Además, la gran variabilidad que presentaban los estudios en cuanto a la dosificación de sus intervenciones (tipo de técnica, número y frecuencia de sesiones), hizo difícil poder identificar dosis óptimas para la aplicación de alguna movilización articular en pacientes con capsulitis adhesiva primaria de hombro. Dentro de las limitaciones metodológicas, a pesar de utilizar ocho bases de datos electrónicas y el seguimiento de referencias de los estudios relevantes, es posible que se hayan pasado por alto algunos estudios. No se consideró realizar búsqueda de literatura gris y además se seleccionaron solo estudios en idioma inglés o español. Tampoco pudimos evaluar el riesgo de sesgo de publicación debido al número limitado de ensayos.
Conclusión
En resumen, se analizaron 14 ensayos clínicos controlados aleatorizados que utilizaron técnicas de movilización articular, con metodología variable en relación con potenciales fuentes de sesgo y estadísticamente heterogéneos. Al aplicar estas técnicas por sí solas o como parte de un programa de tratamiento, comparadas con tratamientos que no incluyen movilización articular, parecen mejorar el rango de movimiento, la función y disminuyen el dolor.
No hubo pruebas para comprobar o refutar una diferencia clínica de algún tipo de técnica por sobre otra, ni tampoco hay suficientes pruebas para determinar la dosis ideal de las diferentes técnicas de movilización articular ocupadas en los distintos ensayos clínicos controlados aleatorizados en pacientes con capsulitis adhesiva primaria.
Notas
Declaración de autoría
JZG: Conceptualización, Metodología, Validación de datos, Análisis formal, Investigación, Materiales, Gestión de datos, Redacción (Preparación del borrador original), Escritura (Revisión y edición), Revisión y presentación, Supervisión, Administración de proyectos.
FPB: Conceptualización, Redacción (Preparación del borrador original), Escritura (Revisión y edición), Revisión y presentación.
HGE: Conceptualización, Metodología, Análisis formal, Redacción (Preparación del borrador original), Escritura (Revisión y edición), Revisión y presentación.
COH: Software, Validación de datos, Análisis formal, Gestión de datos, Redacción (Preparación del borrador original), Escritura (Revisión y edición).
Declaración de financiamiento
Los autores declaran que no hubo fuentes de financiación externas.
Declaración de conflictos de intereses
Los autores han completado el formulario de declaración de conflictos de intereses del ICMJE, y declaran no haber recibido financiamiento para la realización del reporte; no tener relaciones financieras con organizaciones que podrían tener intereses en el artículo publicado, en los últimos tres años; y no tener otras relaciones o actividades que podrían influir sobre el artículo publicado. Los formularios pueden ser solicitados contactando al autor responsable o a la dirección editorial de la Revista.

