Resúmenes Epistemonikos
← vista completaPublicado el 29 de diciembre de 2017 | http://doi.org/10.5867/medwave.2017.09.7121
¿Es efectiva la lidocaína endovenosa para disminuir el dolor y acelerar la recuperación postoperatoria?
Is intravenous lidocaine effective for decreasing pain and speeding up recovery after surgery?
Resumen
INTRODUCCIÓN La lidocaína se utiliza ampliamente en el manejo anestésico debido a sus múltiples propiedades, especialmente analgésicas. Sin embargo, no está del todo claro cuáles son los reales beneficios de su utilización perioperatoria.
MÉTODOS Para responder esta pregunta utilizamos Epistemonikos, la mayor base de datos de revisiones sistemáticas en salud, la cual es mantenida mediante búsquedas en múltiples fuentes de información, incluyendo MEDLINE, EMBASE, Cochrane, entre otras. Extrajimos los datos desde las revisiones identificadas, reanalizamos los datos de los estudios primarios, realizamos un metanálisis y preparamos tablas de resumen de los resultados utilizando el método GRADE.
RESULTADOS Y CONCLUSIONES Identificamos 15 revisiones sistemáticas que en conjunto incluyen 53 estudios primarios, todos correspondientes a ensayos aleatorizados. Concluimos que el uso de lidocaína endovenosa perioperatoria probablemente resulta en una disminución clínicamente irrelevante del dolor y la duración de la estadía hospitalaria, pero que probablemente previene la presencia de náuseas y vómitos postoperatorios.
Problema
Existen distintas alternativas que se utilizan como coadyuvante en distintas técnicas anestésicas, con el objetivo de disminuir los síntomas postoperatorios y acelerar la recuperación. Se ha planteado que la lidocaína, un anestésico local perteneciente al grupo de las aminoamidas que actúa mediante la inhibición de canales de sodio, tendría efectos analgésicos, entre otros, que lo harían una buena opción en el contexto quirúrgico. Sin embargo, aún no está claro si realmente estos efectos se traducen en un beneficio real para los pacientes, y si constituye una intervención segura.
Metodos
Para responder esta pregunta utilizamos Epistemonikos, la mayor base de datos de revisiones sistemáticas en salud, la cual es mantenida mediante búsquedas en múltiples fuentes de información, incluyendo MEDLINE, EMBASE, Cochrane, entre otras. Extrajimos los datos desde las revisiones identificadas y reanalizamos los datos de los estudios primarios. Con esta información, generamos un resumen estructurado denominado FRISBEE (Friendly Summaries of Body of Evidence using Epistemonikos), siguiendo un formato preestablecido, que incluye mensajes clave, un resumen del conjunto de evidencia (presentado como matriz de evidencia en Epistemonikos), metanálisis del total de los estudios cuando sea posible, tablas de resumen de resultados con el método GRADE, y tabla de otras consideraciones para la toma de decisión.
|
Mensajes clave
|
Acerca del conjunto de evidencia para esta pregunta
|
Cuál es la evidencia |
Encontramos 15 revisiones sistemáticas [1],[2],[3],[4],[5],[6], Una de las revisiones [10] presentaba datos sobre un ensayo no incluido en ninguna otra (Harvey 2006), pero de una forma que no fue posible reutilizarlo. En la revisión no se encuentra la referencia, tampoco fue posible identificar el ensayo por otros medios y el autor no respondió al contactarlo. |
|
Qué tipo de pacientes incluyeron los estudios* |
Veinticinco ensayos incluyeron pacientes adultos de 18 a 75 años Siete ensayos incluyeron exclusivamente pacientes de sexo femenino [18],[21],[42],[44],[49],[50],[52], tres incluyeron solo pacientes de sexo masculino [26],[53],[60], los 43 restantes no restringieron la inclusión por sexo. Catorce ensayos incluyeron pacientes ASA I-II [16],[18],[19], En 24 ensayos los pacientes fueron sometidos a cirugía abdominal; de estos, 13 incluyeron solo cirugías digestivas [17], Veintidós ensayos excluyeron a pacientes que tenían condiciones de dolor crónico, tratamiento de dolor crónico o tratamie,nto de dolor en la última semana con cualquier droga analgésica [19], |
|
Qué tipo de intervenciones incluyeron los estudios* |
Todos los ensayos utilizaron lidocaína sistémica endovenosa. Cuarenta y siete ensayos iniciaron la lidocaína en el Cuarenta y dos ensayos utilizaron un bolo de lidocaína (1mg/kg hasta 3 mg/kg) seguido de una infusión (20 μg/kg/min hasta 4 mg/min); de estos, 17 mantuvieron la infusión solo durante el intraoperatorio [18],[25],[27],[28],[29],[34],[35],[40],[41],[42], Cuatro ensayos iniciaron lidocaína postoperatoria; uno utilizó un bolo (1,5 mg/kg) y continuó con una infusión (2mg/kg/h) por dos horas [43]; de los tres restantes, uno utilizó una infusión de lidocaína (60 mg/h) por 24 horas [54] y dos utilizaron PCA sin referir tiempo de término [45],[46]. Un ensayo inicio la lidocaína preoperatoria [58] con bolo (1,5 mg/kg) continuado por una infusión (2 mg/kg/h) solamente durante el intraoperatorio. No se pudieron recopilar datos sobre las características de un ensayo [70] debido a que se encontraba en solo una revisión sistemática [15], y no se obtuvo respuesta del autor de esta al intentar contactarlo. Un ensayo fue incluido en una revisión sistemática con datos preliminares previo a su publicación [35]. Todos los ensayos compararon contra placebo o no tratamiento. |
|
Qué tipo de desenlaces midieron |
Los desenlaces, de acuerdo a como los agruparon las revisiones sistemáticas fueron: Dolor postoperatorio, consumo de analgésicos intraoperatorios y postoperatorios, dolor crónico, incidencia de efectos adversos de opioides, incidencia de náuseas y vómitos postoperatorios, incidencia de íleo y retorno de la funcionalidad gastrointestinal (evaluado por los tiempos hasta la expulsión de gases por boca, hasta tener deposiciones, y hasta el primer movimiento intestinal), duración de la estadía hospitalaria y en la unidad de recuperación postquirúrgica, complicaciones quirúrgicas, eventos adversos, mortalidad, desenlaces cognitivos, satisfacción del paciente, cese de intervención, toxicidad sistémica de lidocaína, niveles plasmáticos de citoquinas. |
* La información sobre los estudios primarios es extraída desde las revisiones sistemáticas identificadas, no directamente desde los estudios, a menos que se especifique lo contrario.
Cuál es la evidencia
Resumen de los resultados
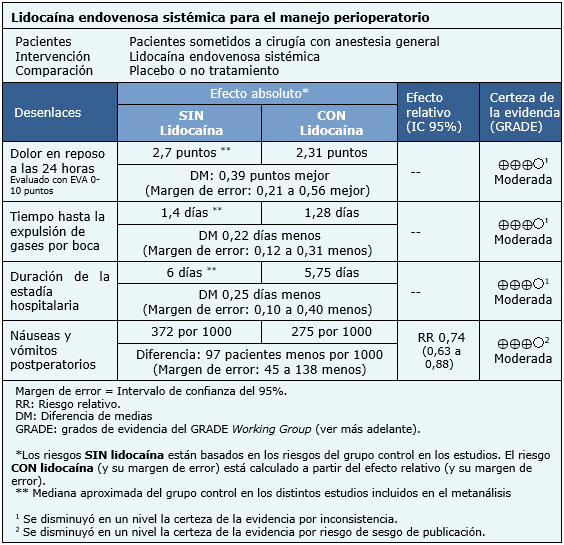
La información sobre los efectos de la lidocaína endovenosa sistémica está basada en 37 ensayos aleatorizados que incluyen 2253 pacientes [16],[17],[18],[20],[21],[22],[23],[24],[25],[27],[28],[31],[32],[33],[35],[39],[40],[41],[42],[44],[48],[49],[51],[52],[53],[54],[57],[58],[59],[60],[61],[62],[63],[65],[66],[68],[69]. Veinticinco ensayos reportaron el desenlace dolor en reposo a las 24 horas [16],[17],[18],[20],[22],[24],[25],[27],[28],[31],[35],[39],[41],[42],[44],[52],[53],[57],[58],[59],[60],[61],[65],[68],[69], 16 reportaron el desenlace tiempo hasta la expulsión de gases por boca [18],[22],[24],[25],[28],[41],[51],[53],[54],[57],[59],[60],[63],[65],[68],[69], 24 midieron el desenlace duración de la estadía hospitalaria [18],[20],[22],[23],[24],[25],[27],[28],[32],[33],[39],[40],[41],48],[51],[53],[54],[57],[58],[59],[60],[61],[62],[69] y 24 midieron el desenlace náuseas y vómitos postoperatorios [16],[17],[18],[20],[21],[24],[25],[27],[28],[31],[35],[39],[41],[44],[49],[57],[58],[59],[60],[63],[65],[66],[68],[69].
El resumen de los resultados es el siguiente:
- El uso de lidocaína perioperatoria probablemente lleva a una disminución clínicamente irrelevante del dolor en reposo a las 24 horas. La certeza de la evidencia es moderada.
- El uso de lidocaína perioperatoria probablemente lleva a una disminución clínicamente irrelevante del tiempo hasta la expulsión de gases por boca. La certeza de la evidencia es moderada.
- El uso de lidocaína perioperatoria probablemente lleva a una disminución clínicamente irrelevante en la duración de la estadía hospitalaria. La certeza de la evidencia es moderada.
- El uso de lidocaína perioperatoria probablemente previene la presencia de náuseas y vómitos postoperatorios. La certeza de la evidencia es moderada.
Otras consideraciones para la toma de decisión
|
A quién se aplica y a quién no se aplica esta evidencia |
|
| Sobre los desenlaces incluidos en este resumen |
|
| Balance riesgo/beneficio y certeza de la evidencia |
|
| Consideraciones de recursos |
|
| Qué piensan los pacientes y sus tratantes |
|
| Diferencias entre este resumen y otras fuentes |
|
| ¿Puede que cambie esta información en el futuro? |
|
Cómo realizamos este resumen
Mediante métodos automatizados y colaborativos recopilamos toda la evidencia relevante para la pregunta de interés y la presentamos en una matriz de evidencia.
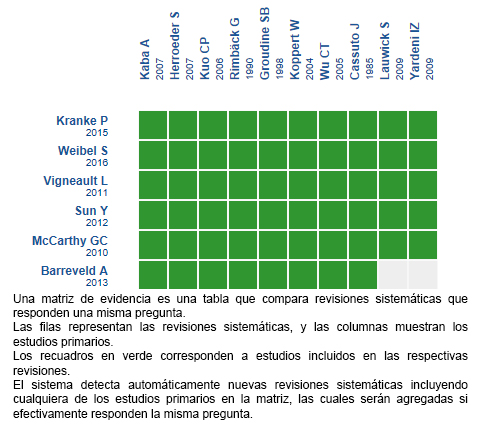
Siga el enlace para acceder a la versión interactiva: Lidocaína endovenosa sistémica perioperatoria versus placebo o no tratamiento
Notas
Si con posterioridad a la publicación de este resumen se publican nuevas revisiones sistemáticas sobre este tema, en la parte superior de la matriz se mostrará un aviso de “nueva evidencia”. Si bien el proyecto contempla la actualización periódica de estos resúmenes, los usuarios están invitados a comentar en la página web de Medwave o contactar a los autores mediante correo electrónico si creen que hay evidencia que motive una actualización más precoz.
Luego de crear una cuenta en Epistemonikos, al guardar las matrices recibirá notificaciones automáticas cada vez que exista nueva evidencia que potencialmente responda a esta pregunta.
Este artículo es parte del proyecto síntesis de evidencia de Epistemonikos. Se elabora con una metodología preestablecida, siguiendo rigurosos estándares metodológicos y proceso de revisión por pares interno. Cada uno de estos artículos corresponde a un resumen, denominado FRISBEE (Friendly Summary of Body of Evidence using Epistemonikos), cuyo principal objetivo es sintetizar el conjunto de evidencia de una pregunta específica, en un formato amigable a los profesionales clínicos. Sus principales recursos se basan en la matriz de evidencia de Epistemonikos y análisis de resultados usando metodología GRADE. Mayores detalles de los métodos para elaborar este FRISBEE están descritos aquí (http://dx.doi.org/10.5867/medwave.2014.06.5997)
La Fundación Epistemonikos es una organización que busca acercar la información a quienes toman decisiones en salud, mediante el uso de tecnologías. Su principal desarrollo es la base de datos Epistemonikos (www.epistemonikos.org).
Declaración de conflictos de intereses
Los autores declaran no tener conflictos de intereses con la materia de este artículo.

